PLANTAR FASCIITIS TREATMENT
That sharp, stabbing heel pain with your first step out of bed? That’s plantar fasciitis — and it affects roughly 10% of adults at some point in their lives.
The good news: with the right physical therapy approach, you can eliminate the pain at its source and get back to the activities that matter most.
At Trinity Rehab, our licensed physical therapists specialize in evidence-based plantar fasciitis physical therapy designed to eliminate heel pain at its source — not just mask the symptoms. With 27 clinics across New Jersey and Pennsylvania, expert care is always close to home.

WHAT IS PLANTAR FASCIITIS?
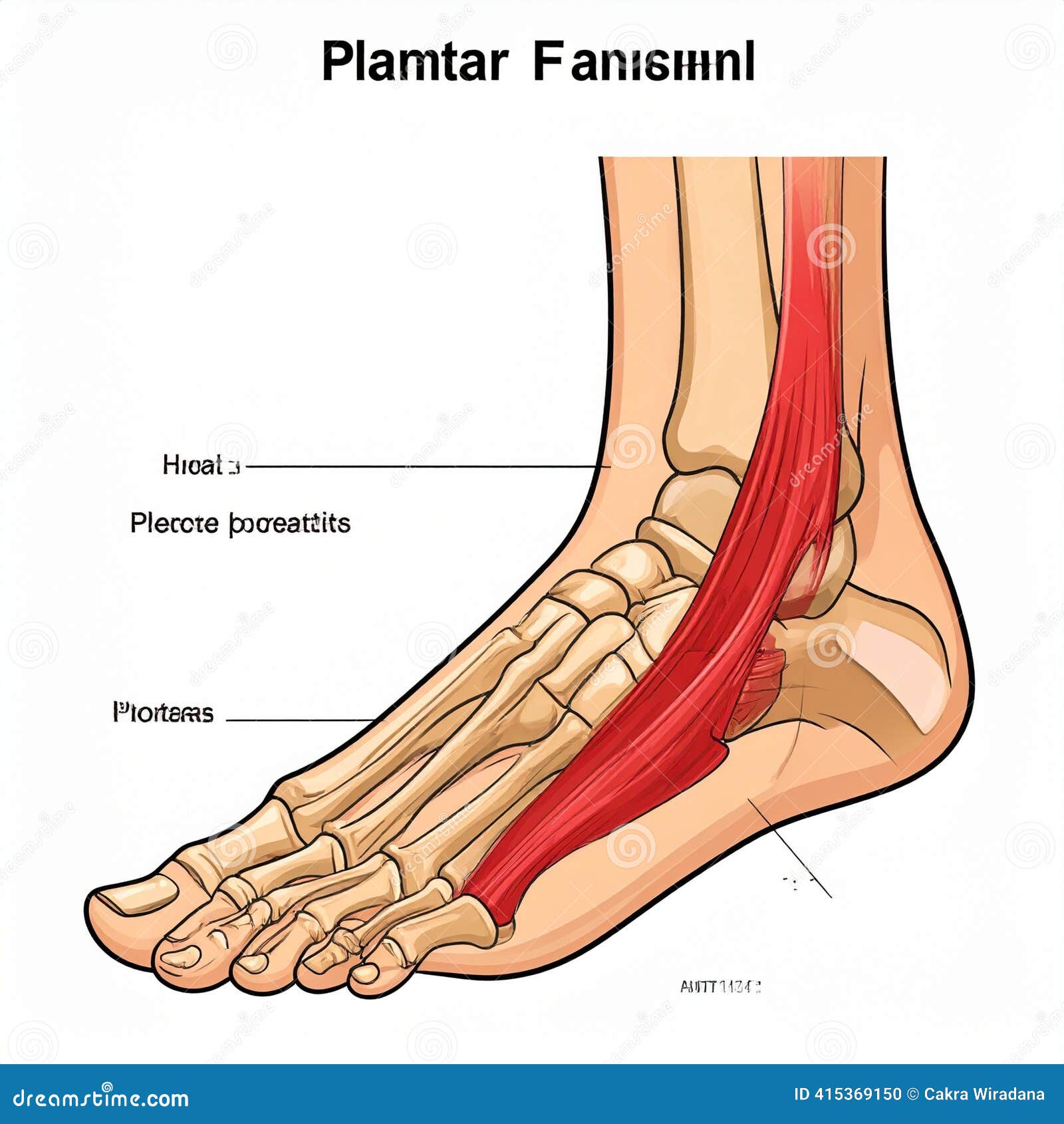
The plantar fascia is a thick band of tissue running along the bottom of your foot, connecting the heel bone to your toes. It works like a bowstring — supporting your arch and absorbing shock with every step.
Plantar fasciitis develops when repetitive stress causes micro-tears and inflammation in this tissue. Over time, the fascia thickens and degenerates, making each step increasingly painful. Without proper treatment, this cycle can persist for months or even years.
According to the American Academy of Orthopaedic Surgeons, approximately 2 million patients are treated for plantar fasciitis every year, and the condition accounts for about 11–15% of all foot symptoms requiring professional care. Research shows that early, structured physical therapy dramatically improves outcomes and reduces the risk of the condition becoming chronic.
WHY PLANTAR FASCIITIS RELIEF MATTERS
Ignoring plantar fasciitis does more than prolong heel pain. When you change how you walk to avoid discomfort, you place extra stress on your ankles, knees, hips, and lower back — triggering a chain reaction of problems well beyond your feet.
Untreated plantar fasciitis can lead to:
- Chronic heel pain and foot pain that limits daily mobility and independence
- Compensatory injuries in the ankle, knee, hip, or lower back
- Reduced activity levels that contribute to weight gain and cardiovascular decline
- Loss of participation in sports, exercise, and recreational activities
- Sleep disruption from persistent pain and morning stiffness
- Decreased quality of life and emotional well-being
Early intervention with targeted physical therapy can break this cycle, restoring healthy biomechanics before downstream complications take root.
COMMON CAUSES OF PLANTAR FASCIITIS
Plantar fasciitis rarely has a single cause. It typically results from a combination of factors that overload the plantar fascia beyond its capacity to heal:
- Repetitive impact activities — Running, jogging, jumping, and prolonged walking on hard surfaces place sustained stress on the plantar fascia, especially without adequate footwear support.
- Long periods of standing — Teachers, nurses, retail workers, factory employees, and warehouse staff who spend long periods on their feet are particularly susceptible to plantar fasciitis. Work-related injuries involving the feet are more common than many people realize.
- Tight calf muscles and Achilles tendon — Restricted ankle dorsiflexion caused by tight muscles in the gastrocnemius and soleus increases strain on the plantar fascia with every step.
- Foot mechanics and arch abnormalities — Both flat feet (pes planus) and high arches (pes cavus) alter how weight distributes across the foot. Overpronation — the inward rolling of the foot during walking — is a particularly common contributor to poor foot health.
- Excess body weight — Additional body weight amplifies the ground reaction forces transmitted through the plantar fascia during weight-bearing activities, accelerating tissue breakdown and placing extra stress on the heel and arch.
- Age-related changes — Plantar fasciitis most commonly affects adults between ages 40 and 60. The fat pad beneath the heel thins naturally with age, reducing its shock absorption capacity.
- Improper footwear — Worn-out shoes, flat sandals, flip-flops, and shoes without adequate arch support fail to protect the plantar fascia from excessive strain. Improper footwear is one of the most correctable risk factors for plantar fasciitis and a key focus of patient education during physical therapy.
- Sudden increases in activity — Training errors such as rapidly increasing running mileage, starting a new exercise program, or transitioning to minimalist footwear without gradual adaptation can overwhelm the tissue.
SYMPTOMS PATIENTS OFTEN NOTICE
Plantar fasciitis has a distinctive symptom pattern that often makes it recognizable even before a formal diagnosis. Recognizing these signs early allows you to seek treatment and begin working to manage symptoms before the condition becomes chronic.
- Sharp heel pain and foot pain with the first steps in the morning — Often described as stepping on a nail or a knife, this “first-step pain” is the most characteristic symptom of plantar fasciitis. The fascia stiffens overnight, and the initial weight-bearing load causes a sudden, intense stretch. The plantar fascia is under constant stretch during standing and walking.
- Pain after prolonged sitting or rest — Similar to morning pain, discomfort often flares after sitting at a desk, driving, or watching a movie. The first few steps are the worst, gradually easing as the tissue warms up.
- Tenderness at the base of the heel — Pressing on the painful area at the inside bottom of the heel typically reproduces the pain, corresponding to the origin point of the plantar fascia on the calcaneus.
- Pain that worsens after (not during) exercise — Many patients notice that heel pain intensifies after a run or workout rather than during the activity itself. This delayed response reflects the inflammatory cycle triggered by repetitive loading.
- Stiffness along the arch of the foot — The entire bottom of the foot may feel tight, especially in the morning or after inactivity.
- Difficulty climbing stairs, limping, or altered gait — As the condition progresses, patients unconsciously shift weight to the outside of the foot or shorten their stride to minimize heel contact.
If you experience any of these symptoms for more than two weeks, physical therapy can help prevent the condition from worsening. You can schedule an evaluation at Trinity Rehab — no referral needed.

HOW PHYSICAL THERAPY RESTORES FUNCTION
At Trinity Rehab, plantar fasciitis treatment goes well beyond generic stretching and ice packs. Our physical therapists conduct a thorough biomechanical assessment of your foot, ankle, and gait to identify the root causes driving your pain — then build a personalized treatment plan using proven clinical techniques.
MANUAL THERAPY AND SOFT TISSUE MOBILIZATION
Hands-on manual therapy is often the cornerstone of plantar fasciitis rehabilitation. Your physical therapist may use:
- Joint mobilization — Gentle, targeted movements of the ankle and subtalar joints restore range of motion and reduce stiffness. Research published in the Journal of Orthopaedic & Sports Physical Therapy (J Orthop Sports Phys Ther) confirms that subtalar mobilization combined with stretching produces significantly greater ability to improve pain and function than conventional therapy alone.
- Instrument-assisted soft tissue mobilization (IASTM) — Specialized tools break down scar tissue adhesions along the plantar fascia and calf muscles, promoting healthy tissue remodeling.
- Myofascial release — Sustained pressure techniques address trigger points in the calf, Achilles tendon, and foot intrinsic muscles that contribute to fascial tension.

TARGETED STRETCHING AND FLEXIBILITY
A structured program of stretching exercises is essential for reducing the mechanical load on the plantar fascia and improving flexibility throughout the foot and lower leg:
- Plantar fascia-specific stretch — Dorsiflexing the toes while palpating the taut fascia creates a targeted stretch through the windlass mechanism. Clinical guidelines recommend holding for 30 seconds, repeating three times, especially before the first steps of the morning.
- Gastrocnemius and soleus calf stretch — Wall stretches, step drops, and towel-assisted calf stretch variations improve ankle dorsiflexion, reducing the strain transferred to the plantar fascia during walking and running. Research shows that consistent calf stretch routines performed multiple times daily are among the most effective stretching exercises for plantar fasciitis relief.
- Achilles tendon mobilization — Eccentric calf loading and dynamic stretching address the kinetic chain connection between the Achilles tendon and the plantar fascia.
PROGRESSIVE STRENGTHENING AND ECCENTRIC LOADING
Strengthening the foot and lower leg musculature is critical for long-term recovery and prevention. Your physical therapist will progress your exercise program systematically, building load tolerance in the plantar fascia over time:
- Intrinsic foot muscle strengthening — Towel scrunches, marble pickups, and short-foot exercises build the small muscles that support the arch from beneath. These exercises also improve flexibility in the intrinsic foot muscles, helping to reduce strain on the fascia.
- Eccentric calf raises — Slowly lowering through the heel off a step builds tendon and fascial resilience, gradually increasing load tolerance in the plantar fascia.
- High load strength training — High load strength training exercises, such as heel raises performed with a rolled towel under the toes to keep only your toes elevated, have been shown in research to reduce pain and accelerate recovery. DiGiovanni BF et al. (J Bone Joint Surg Am) demonstrated that plantar fascia-specific stretching and progressive loading exercises produced superior outcomes compared to Achilles tendon stretching alone — a landmark finding that continues to shape clinical practice guidelines.
- Gait training — Your physical therapist will analyze and correct your walking and running mechanics through structured gait training, addressing the movement patterns that place extra stress on the plantar fascia.
- Your physical therapist may also incorporate toe walking drills and balance and proprioception training — Single-leg stance progressions and wobble board exercises improve neuromuscular control, reducing abnormal loading patterns that stress the fascia.
ADVANCED TREATMENT MODALITIES
For persistent or chronic plantar fasciitis, Trinity Rehab offers advanced interventions:
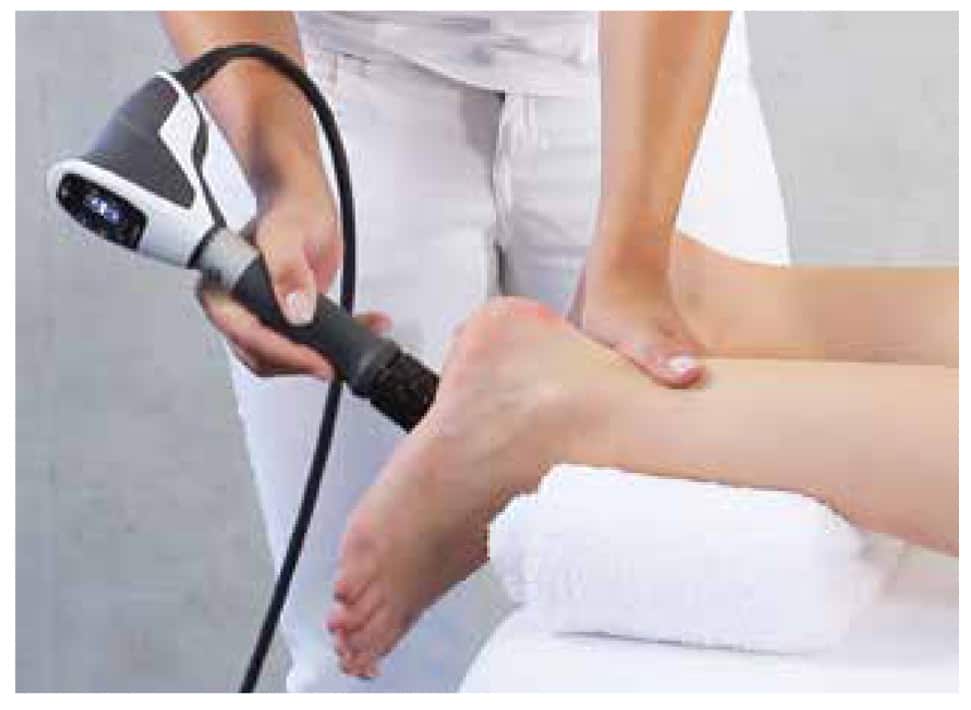
- EPAT / Extracorporeal Shockwave Therapy — Acoustic pressure waves stimulate blood flow and cellular repair in the damaged fascia. The Mayo Clinic identifies ESWT as an effective option for chronic cases that have not responded to conservative treatment.
- Dry Needling — Fine filament needles target myofascial trigger points in the calf and foot, releasing deep muscle tension that contributes to fascial overload.
- Platelet rich plasma (PRP) injection — In cases where conservative physical therapy has not fully resolved symptoms, platelet rich plasma therapy may be recommended by your healthcare provider or sports medicine physician to stimulate tissue regeneration in the damaged fascia.
- Kinesiology taping — Strategic taping provides short-term arch support and offloads the plantar fascia during activity, as recommended in the latest J Orthop Sports Phys Ther clinical practice guidelines.
- Therapeutic ultrasound — Deep tissue heating promotes blood flow and accelerates the healing process in the damaged fascial tissue.
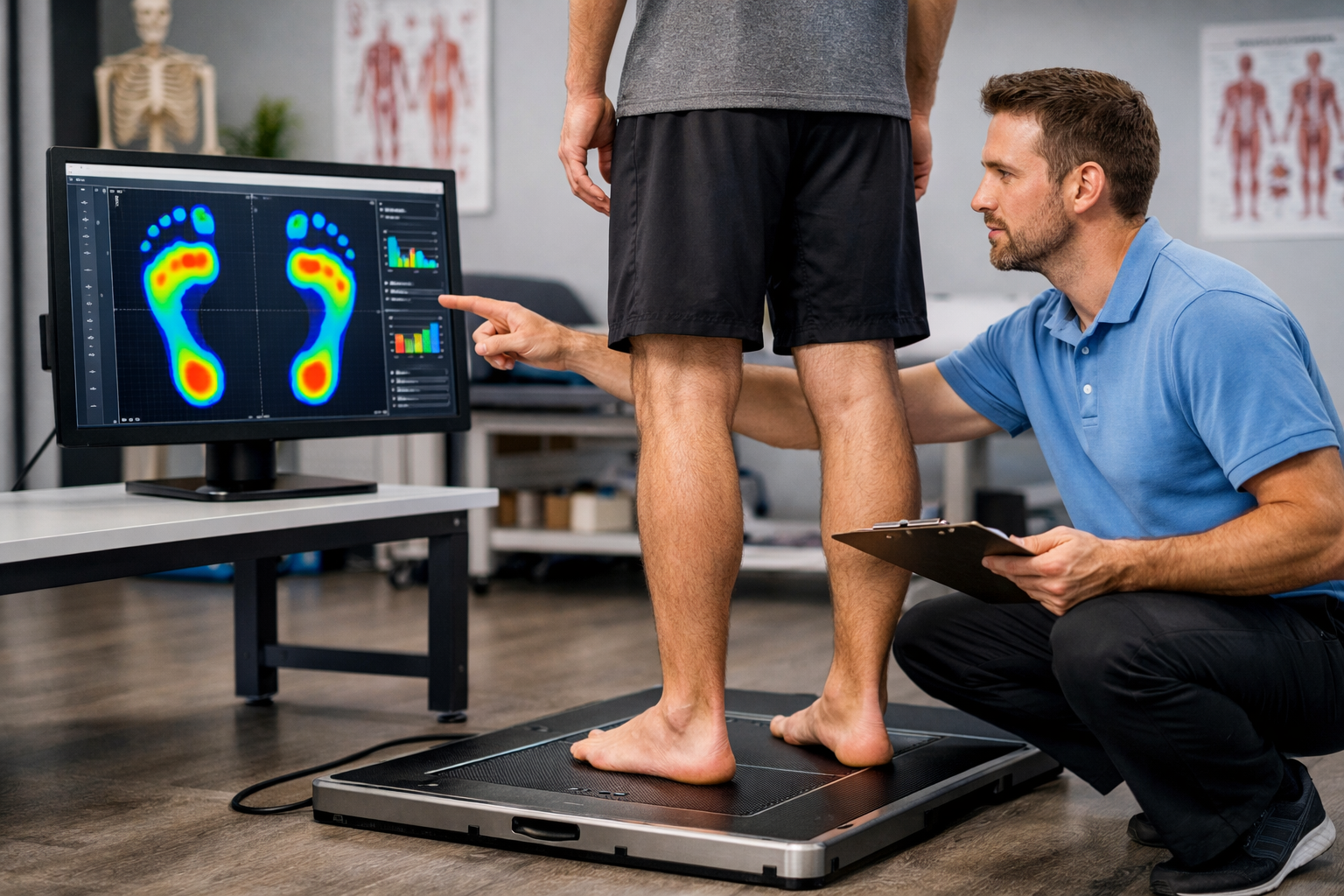
CUSTOM ORTHOTIC ASSESSMENT AND FOOTWEAR GUIDANCE
Your physical therapist will evaluate your current footwear and assess for the impact of improper footwear on your biomechanics. They may recommend custom orthotics or supportive shoe inserts to correct issues such as overpronation, flat feet, or high arches — all of which compromise long-term foot health. Night splints — specifically posterior night splints — that maintain the ankle in a dorsiflexed position may also be prescribed. Night splints are particularly effective to prevent overnight fascial contracture and reduce that characteristic first-step morning pain.
PLANTAR FASCIITIS EXERCISES YOU CAN DO AT HOME
One of the most important parts of your physical therapy exercise program is the home routine your physical therapist designs for you. Performing targeted exercises daily — especially before your first steps in the morning and after periods of rest — is one of the most effective ways to reduce pain, improve flexibility, and speed recovery. Research shows that patients who consistently follow their home exercise program achieve significantly better outcomes than those who rely on in-clinic treatment alone.
The following stretching exercises and strengthening exercises are commonly included in Trinity Rehab’s plantar fasciitis home programs. Always follow your physical therapist’s specific guidance, as your exercise program will be individualized based on your evaluation findings.

1. PLANTAR FASCIA STRETCH
Starting position: Sit down in a chair. Cross one leg over the other so that the ankle of your affected foot rests on the opposite knee.
How to do it: With your hand, gently pull your toes back toward your shin until you feel a firm stretch along the bottom of your foot. Hold for 30 seconds, then release. Repeat three times on each foot. This is most effective when performed before taking your first steps in the morning and after long periods of sitting.
Why it works: Gently pulling the toes back loads the plantar fascia through the windlass mechanism, directly stretching the inflamed tissue and improving flexibility at the foot and ankle.
2. STANDING CALF STRETCH AGAINST THE WALL
Starting position: Stand facing a wall with both hands flat on the wall for support.
How to do it: Step one foot back so your front leg is bent and your back leg is straight. Keep both feet flat on the ground throughout the movement. Lean your body forward until you feel a deep calf stretch in the straight back leg. Hold for 30 seconds, then switch legs — for example, if your left leg was the back leg first, bring the left leg forward and extend the right leg back. Repeat two to three times per leg. For a deeper soleus stretch (lower calf), perform the same calf stretch with the back leg slightly bent.
Why it works: Tight calf muscles are one of the leading contributors to plantar fasciitis. This calf stretch improves ankle dorsiflexion, directly reducing the strain on the plantar fascia during walking, running, and standing.
3. SEATED TOWEL STRETCH
Starting position: Sit down on a chair or on the edge of your bed with your leg extended in front of you.
How to do it: Loop a small towel around the ball of your foot and the base of your toes. Hold one end of the towel in each hand and gently pull the towel toward you, flexing your foot back until you feel a stretch through your calf and the bottom of your foot. Hold for 30 seconds. Repeat three times on each leg.
Why it works: The towel stretch is an excellent alternative to standing stretching exercises, making it ideal first thing in the morning before placing weight on your foot. The small towel allows precise control of the stretch intensity.
4. FROZEN WATER BOTTLE ROLL
Starting position: Sit in a chair with both feet flat on the ground.
How to do it: Place a frozen water bottle on the ground directly under one foot. Gently roll the frozen water bottle back and forth under the arch of your foot, from the heel to the ball of the foot, for two to three minutes. Switch to the other foot as needed. Repeat two to three times daily, especially after activity.
Why it works: Rolling a frozen water bottle under the foot simultaneously applies ice therapy to reduce inflammation and provides a gentle massage to the plantar fascia. This combination helps apply ice directly to the painful area, reduce pain, and loosen tight fascial tissue.
5. GOLF BALL OR TENNIS BALL ROLL
Starting position: Sit down in a chair with both feet flat on the ground.
How to do it: Place a golf ball or tennis ball on the ground under one foot. Apply moderate pressure through your foot and roll the ball slowly back and forth from the heel to the ball of the foot. If you find a particularly tender spot, hold gentle pressure on that area for 10–15 seconds before continuing. Continue for two to three minutes per foot.
Why it works: Rolling a ball under the foot provides targeted myofascial release to the plantar fascia and intrinsic foot muscles. A golf ball delivers firmer pressure, while a tennis ball is gentler — your physical therapist can guide which is appropriate for your current pain level.
6. TOWEL SCRUNCHES (TOE EXTENSION AND INTRINSIC STRENGTHENING)
Starting position: Sit down in a chair. Place a small towel flat on the floor in front of you. Put your feet flat on the towel with your toes positioned over the near edge.
How to do it: Using only your toes, scrunch and grip the towel, pulling it toward you across the ground. Straighten your toes (toe extension), then scrunch again. Continue for 30–60 seconds per foot. You can also perform this exercise by picking up marbles or small objects with only your toes.
Why it works: Towel scrunches and toe extension exercises strengthen the intrinsic muscles of the foot, building the arch support that reduces load on the plantar fascia. These exercises directly improve flexibility and neuromuscular control in the foot.
7. SINGLE-LEG CALF RAISES
Starting position: Stand near a wall or chair for balance. Shift your weight to one leg, lifting the opposite foot slightly off the ground.
How to do it: Standing on one leg, slowly rise up on your toes as high as comfortable, then lower your heel back to the ground in a controlled, slow motion over three to four seconds. Perform 10–15 repetitions per leg. As this becomes easier, progress to performing the exercise on a slightly elevated surface such as a step.
Why it works: Single-leg calf raises build strength in the gastrocnemius and soleus muscles, improving the load capacity of the Achilles tendon and plantar fascia. Performing these on one leg closely mimics the demands of walking and running, making the exercise highly functional for returning to activity.
8. HIGH LOAD STRENGTH TRAINING — HEEL RAISE WITH TOWEL
Starting position: Stand on one leg near a wall for balance. Place a small rolled towel or a folded towel under the toes of your standing foot so that only your toes are elevated while your heel remains on the ground.
How to do it: Keeping your knee straight, rise up on only your toes as high as possible, then slowly lower over three to five seconds. Perform 12–15 repetitions, then switch to the other leg. This high load strength training exercise should be performed once daily.
Why it works: High load strength training with the toes elevated increases the eccentric load on the plantar fascia, stimulating tissue remodeling and building resilience in the fascia. Research shows that this specific high load strength training protocol — first studied by Rathleff and colleagues, building on the foundational work of DiGiovanni BF and the J Orthop Sports Phys Ther clinical guidelines — produces significant and lasting reductions in plantar fasciitis pain.
Important note: Begin these exercises gently and progress gradually. If any exercise significantly increases your foot pain or heel pain, stop and contact your physical therapist. Your physical therapist will customize the sets, repetitions, and progression of your exercise program based on your individual evaluation and recovery goals.
HOW TO PREVENT PLANTAR FASCIITIS FROM RETURNING
Recovery from plantar fasciitis is only half the battle. Without addressing the underlying factors, recurrence rates remain high. Trinity Rehab’s prevention-focused approach equips you with the tools and knowledge to keep your feet healthy and maintain foot health for the long term.
- Maintain a healthy weight — Even modest weight loss significantly reduces the biomechanical stress on the plantar fascia during daily activities.
- Wear supportive footwear — Choose shoes with good arch support, cushioned soles, and a slight heel elevation. Avoid improper footwear such as worn-out shoes, unsupported sandals, or flat flip-flops. Replace running shoes every 300–500 miles to maintain foot health.
- Stretch daily — Continue your plantar fascia and calf stretch routine as part of your ongoing exercise program, even after symptoms resolve, especially before morning activities and exercise.
- Progress activity gradually — Follow the 10% rule: increase weekly exercise volume (mileage, duration, intensity) by no more than 10% to allow tissues to adapt.
- Strengthen your feet — Maintain an intrinsic foot and plantar muscles strengthening routine to provide ongoing arch support and improve flexibility from within.
- Modify high-impact activities — Alternate running with low-impact cross-training such as cycling, swimming, or rowing to reduce cumulative fascial loading.
- Use orthotics when needed — If you have structural foot abnormalities (flat feet, high arches, overpronation), consistent use of custom orthotics provides ongoing biomechanical correction and supports foot health.
- Apply ice when symptoms flare — Apply ice to the heel and arch for 10–15 minutes after activity to reduce inflammation and manage symptoms early. A frozen water bottle roll is a convenient way to apply ice and massage the foot simultaneously.
- Listen to your body — Address early warning signs like mild heel tenderness or morning stiffness immediately with stretching exercises, icing, and activity modification before the condition escalates.
WHY PATIENTS CHOOSE TRINITY REHAB
Choosing the right physical therapy provider makes all the difference in your plantar fasciitis recovery. Trinity Rehab offers a patient experience designed around results, combining the expertise of sports physical therapy with the personal attention of one-on-one care.
- One-on-one care — Every session is spent directly with your licensed physical therapist, not handed off to an aide or assistant. This personalized attention ensures your treatment plan adapts to your progress at every visit.
- Evidence-based treatment — Our clinical protocols reflect the latest research and clinical practice guidelines from the American Physical Therapy Association, ensuring you receive the most effective interventions available. Research shows that structured physical therapy with targeted exercises produces outcomes superior to passive treatments alone.
- Sports physical therapy expertise — Our physical therapists have deep experience in sports physical therapy, helping athletes and active patients return to full performance after plantar fasciitis and other musculoskeletal conditions.
- Advanced technology — From EPAT shockwave therapy to dry needling and instrument-assisted soft tissue mobilization, Trinity Rehab invests in the treatment modalities that deliver faster, more complete recovery.
- Convenient locations — With 27 clinics across New Jersey and Pennsylvania, expert plantar fasciitis treatment is always close to home, work, or school.
- Flexible scheduling — Early morning, evening, and accommodating appointment times make it easy to fit physical therapy into your busy schedule.
- Most insurance accepted — We work with most major insurance carriers to keep quality care accessible and affordable.
- Patient education — We believe that informed patients recover faster. Your care team provides patient education at every stage of your treatment, from understanding what drives your pain to learning how to manage symptoms and prevent recurrence at home.
Find Plantar Fasciitis Treatment Near You
New Jersey Locations
Pennsylvania Locations
FREQUENTLY ASKED QUESTIONS
Related Conditions
How long does it take to recover from plantar fasciitis with physical therapy?
Can I still exercise with plantar fasciitis?
Do I need orthotics for plantar fasciitis?
Is plantar fasciitis the same as a heel spur?
When should I see a physical therapist for heel pain?
What is the role of sports physical therapy in plantar fasciitis treatment?
GETTING BACK TO WHAT MATTERS
Plantar fasciitis can feel like it controls your life — limiting your morning routine, your exercise program, your time on your feet at work, and your ability to enjoy the activities you love. But it does not have to. With the right treatment approach, the vast majority of patients recover fully and return to an active, pain-free lifestyle.
At Trinity Rehab, we have helped thousands of patients across New Jersey and Pennsylvania overcome plantar fasciitis and reclaim their mobility. At Trinity Rehab, we treat plantar fasciitis with a comprehensive approach. Our combination of hands-on manual therapy, targeted stretching exercises and strengthening exercises, advanced modalities like EPAT shockwave therapy and dry needling, and genuine one-on-one, hands-on care creates a recovery experience that delivers real, lasting results. From your first physical therapy session through your last, your physical therapist and care team are with you every step of the way.
YOUR NEXT STEPS
Getting started with plantar fasciitis physical therapy at Trinity Rehab is simple:
- Request an appointment — Schedule online or call your nearest Trinity Rehab location.
- Get your personalized evaluation — Your physical therapist will conduct a thorough physical examination and comprehensive assessment of your foot mechanics, movement patterns, medical history, and pain presentation.
- Begin your recovery — Start your individualized plan to treat plantar fasciitis and exercise program, and take the first step toward pain-free living.
No physician referral is required. Most major insurance plans are accepted.
Sources: Journal of Orthopaedic & Sports Physical Therapy — Clinical Practice Guidelines for Heel Pain/Plantar Fasciitis, 2023 Revision (J Orthop Sports Phys Ther) | Mayo Clinic — Plantar Fasciitis Diagnosis and Treatment | NIH/PMC — Management of Plantar Fasciitis in the Outpatient Setting | DiGiovanni BF, Nawoczenski DA, Lintal ME, et al. “Tissue-specific plantar fascia-stretching exercise enhances outcomes in patients with chronic heel pain.” J Bone Joint Surg Am. 2003;85(7):1270–1277.
FIND PLANTAR FASCIITIS TREATMENT NEAR YOU
Trinity Rehab provides specialized plantar fasciitis treatment at 27 clinics across New Jersey and Pennsylvania. Select your location below for local resources and to schedule your first appointment.
NEW JERSEY LOCATIONS
PENNSYLVANIA LOCATIONS
OTHER CONDITIONS WE TREAT
Trinity Rehab treats a wide range of musculoskeletal conditions. Explore our other condition-specific resources:
