PLANTAR FASCIITIS TREATMENT IN UPPER DUBLIN, PA
Upper Dublin Township has built its identity around an active, engaged community. SPARK — the Upper Dublin Sports Park — draws families to synthetic turf fields and a walking trail year-round. The township’s 600-plus acres of open space and network of parks, from Twining Valley to Luther Klosterman, support runners, walkers, and youth athletes across all seasons. The Upper Dublin Sports Center’s tennis academy and pickleball courts keep adults competing well into their working years. And the sprawling Fort Washington Office Park, one of the East Coast’s original suburban business parks, employs more than 12,000 people who spend significant time on their feet in its offices, distribution facilities, and manufacturing spaces.
Plantar fasciitis threads through all of it. If you’re dealing with heel pain that peaks when you step out of bed, returns every time you sit down and stand back up, and limits how fully you can participate in the activities and work that define your Upper Dublin life — you are not alone, and you do not have to accept this as your new normal.
Trinity Rehab provides one-on-one, evidence-based plantar fasciitis treatment for Upper Dublin and Montgomery County residents. Our physical therapists identify the specific biomechanical, occupational, and activity-related factors driving your heel pain and address them directly — not just symptomatically.

WHAT IS PLANTAR FASCIITIS?
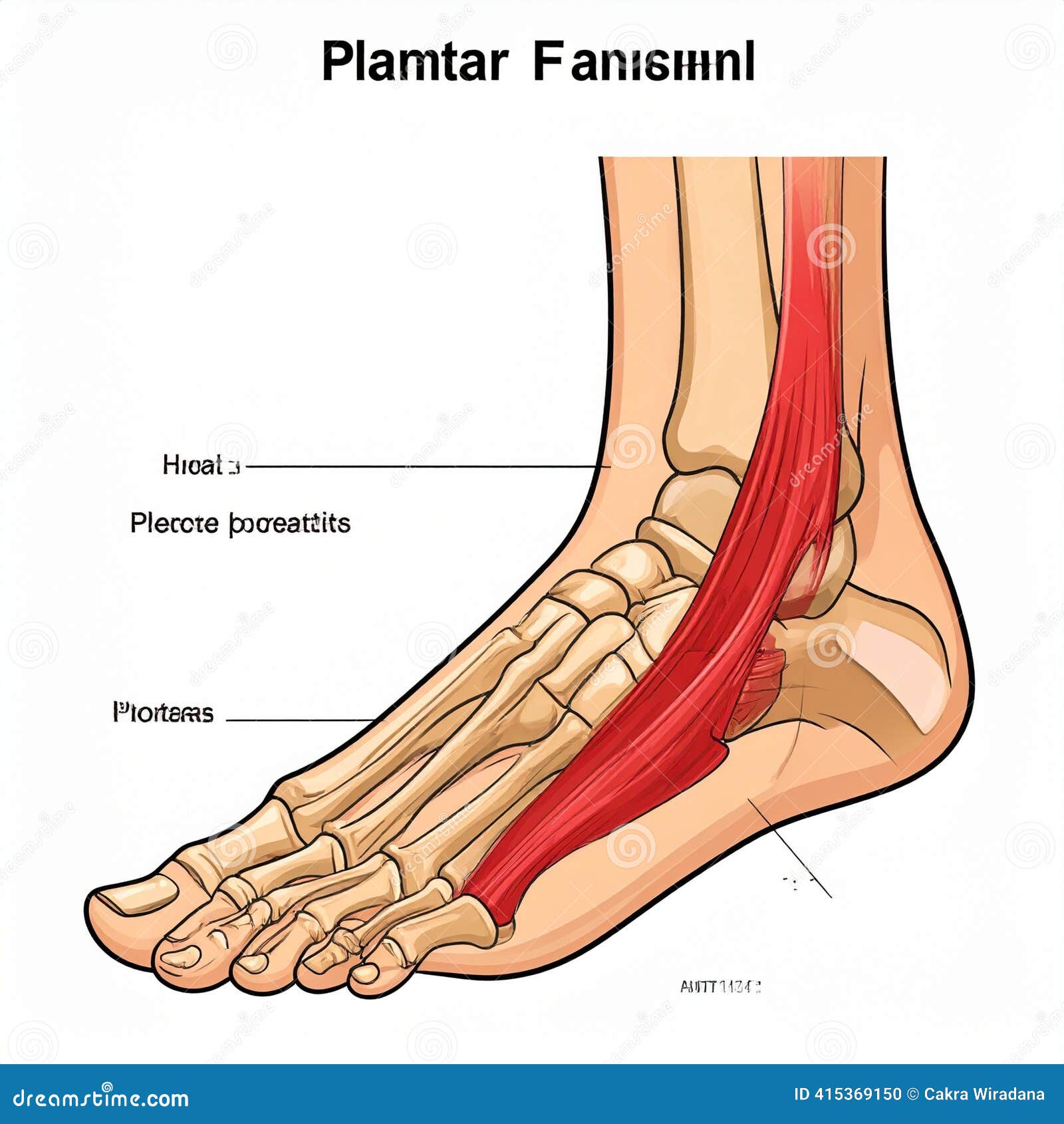
The plantar fascia is the thick, fibrous band of connective tissue running the length of your foot’s sole, from the calcaneus (heel bone) to the metatarsal heads at the base of the toes. It performs a dual function: providing passive structural support for the arch and enabling the energy-storing, spring-like mechanics of normal walking and running through the windlass mechanism.
Plantar fasciitis develops when the cumulative mechanical load on this tissue consistently exceeds its capacity for self-repair. Micro-tears accumulate at the calcaneal attachment — the most vulnerable point — triggering an inflammatory response. Without a change in loading or targeted treatment, the body’s attempt at repair is perpetually outpaced by the damage, leading to fascial thickening, loss of flexibility, and progressive degeneration. The resulting pain cycle can persist for months or years if the underlying drivers are not addressed.
The American Academy of Orthopaedic Surgeons reports that approximately 2 million people receive treatment for plantar fasciitis annually in the United States. It is the leading cause of heel pain in adults and disproportionately affects those aged 40 to 60 — a demographic that constitutes a substantial portion of Upper Dublin’s workforce and active population. Physical therapy, when applied comprehensively and beginning before the condition becomes fully chronic, resolves the vast majority of cases.
RELATED CONDITIONS & TREATMENTS
Plantar fasciitis is just one of the many conditions we treat at Trinity Rehab Upper Dublin. Explore our full range of conditions we treat or learn more about specific treatment approaches:
WHY UPPER DUBLIN RESIDENTS ARE AT RISK
Upper Dublin’s specific combination of affluent suburban living, corporate employment, and competitive athletics creates several well-defined pathways to plantar fasciitis.
Fort Washington Office Park employees — among them the 12,000-plus workers at the 230-plus businesses occupying the park’s 6 million square feet — experience a distinct occupational risk profile. Long periods of desk work alternate with significant walking through campus-style buildings, parking structures, and outdoor paths. Standing-intensive roles in distribution, manufacturing, and on-site operations involve prolonged hard-floor loading. Companies like Nutrisystem, SofterWare, and PetroChoice, along with the IT solutions and back-office operations throughout the park, collectively employ residents whose footwear and movement patterns often don’t account for the cumulative demands on the plantar fascia.
SPARK and township trail users are another primary population. The SPARK — Upper Dublin Sports Park’s synthetic turf fields and 0.5-mile walking trail — along with the Twining Valley Park trail system and the broader 40-plus park network create ample opportunity for the repetitive-impact, prolonged-walking activity that loads the plantar fascia. The Healthy Kids Running Series and adult fitness programs based in these parks bring Upper Dublin’s fitness community onto hard surfaces throughout the year.
Upper Dublin High School Cardinals athletes compete across 14 boys’ and 13 girls’ varsity sports in the Suburban One American Conference. The girls’ swimming and diving program recently won state honors, and the football, lacrosse, soccer, and wrestling programs run demanding conditioning schedules. Athletes who compete year-round across multiple sports — or who return aggressively from off-seasons — accumulate the overuse injury patterns that include plantar fasciitis. Field hockey and tennis athletes, whose sports combine lateral movement with significant impact loading, are particularly susceptible.
Upper Dublin Sports Center tennis and pickleball players make the explosive lateral movements, quick stops, and directional changes that place sharp, repetitive demands on the plantar fascia. Hard court surfaces amplify every impact. Players who participate in USTA league play or regular clinic sessions without adequate calf flexibility or foot strength conditioning are at elevated risk.
Golfers at Manufacturers Golf & Country Club and Lu Lu Country Club walk 18 holes of rolling terrain per round — five to seven miles of sustained, repetitive loading on the plantar fascia and lower limb. Golf footwear is rarely optimized for the fascial demands of the game, and the combination of prolonged walking on uneven ground with the rotational forces of the golf swing is a well-documented risk factor.
Life Time Fitness members in Fort Washington who participate in high-impact fitness classes, group running programs, or heavy gym schedules face a similar accumulation of fascial loading — particularly if calf flexibility and foot strength conditioning are not incorporated into their routine.
WHAT PLANTAR FASCIITIS FEELS LIKE
The symptom pattern is characteristic and reliably distinguishable from other causes of heel and foot pain:
Sharp, stabbing heel pain with the very first steps of the morning is the hallmark. The plantar fascia shortens and stiffens during sleep; the sudden weight of the first footfall creates an intense, abrupt stretch at the calcaneal attachment that many patients describe as stepping onto a nail or hot coal. This peak pain typically eases within 10 to 20 minutes of walking, which sometimes gives patients a false sense that the problem is resolving — until it returns after the next rest period.
Post-rest pain mirrors the morning experience. Sitting through a Fort Washington conference call, driving along Route 309 during the evening commute, or watching an Upper Dublin Cardinals game from the bleachers for 90 minutes — any sustained rest period can trigger the stiffening cycle, making the first steps after the next stand-up reliably the worst.
Other signs:
- Point tenderness at the inner (medial) base of the heel, at the fascial origin
- Persistent arch tightness through the morning, separate from the acute heel pain
- Aching that develops or intensifies 30 to 60 minutes after completing a run or long walk
- Subtle gait compensation: shortened stride, slight limp, or weight-shifting to the forefoot or lateral foot
- In severe cases, difficulty completing a full shift at work without foot pain significantly affecting function
An Upper Dublin professional who participates in regular tennis clinics at the Sports Center described the progression: “I was playing three times a week and felt fine on the court. But after two or three hours my heel would start aching, and the next morning was brutal. I thought I had a bruise. Then I realized it was happening every single day.” That delayed post-activity onset and daily morning pain pattern is textbook plantar fasciitis.
HOW PHYSICAL THERAPY RESTORES FUNCTION
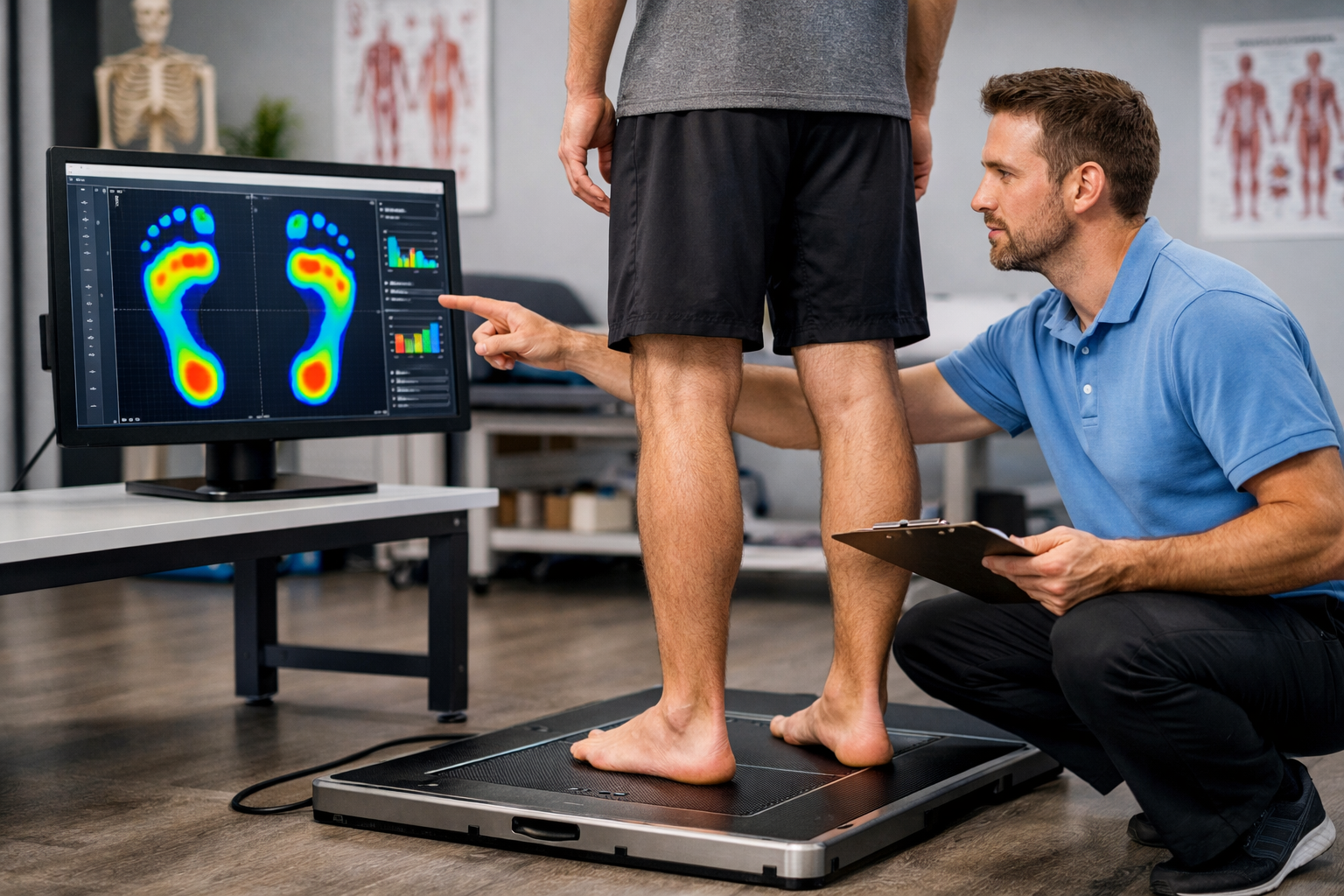
Trinity Rehab designs every treatment plan from a comprehensive evaluation — foot mechanics, ankle range of motion, calf flexibility, gait pattern, and an assessment of the specific occupational and recreational demands loading your fascia. The plan that results is specific to your body and your life, not a standardized protocol.
MANUAL THERAPY
Manual therapy is the foundation of early treatment. Ankle and subtalar joint mobilization directly addresses the dorsiflexion restriction that is among the most consistent mechanical drivers of plantar fasciitis. When the ankle can’t complete its full arc of motion, the plantar fascia compensates by absorbing the load that the joint should be managing — a pattern that accumulates injury with every step. Research in the Journal of Orthopaedic & Sports Physical Therapy confirms that joint mobilization combined with stretching produces significantly better outcomes than stretching alone.
Instrument-assisted soft tissue mobilization (IASTM) works through the fascial adhesions and scar tissue that accumulate with chronic loading, stimulating healthy collagen remodeling. Myofascial release targeting trigger points in the gastrocnemius, soleus, and foot intrinsic muscles reduces the resting fascial tension that maintains irritation between loading events.

STRETCHING
The plantar fascia-specific stretch — pulling the toes into dorsiflexion before the first step of the morning, holding 30 seconds — pre-loads the windlass mechanism and significantly reduces the severity of first-step pain. Calf stretching targeting the gastrocnemius and soleus separately restores ankle dorsiflexion and reduces the upstream tightness that drives fascial overload. Your therapist prescribes both based on your specific mobility deficits.
ECCENTRIC LOADING AND INTRINSIC STRENGTHENING
Eccentric calf raises — lowering the heel slowly off a step — are the most evidence-supported exercise intervention for plantar fasciitis. They build the tensile strength in the calf-Achilles-fascial unit that allows the tissue to handle load without breaking down. Intrinsic foot strengthening through towel scrunches, marble pickups, and the short-foot exercise develops the arch’s internal muscular support — reducing the passive load carried by the plantar fascia on every step. Progressive single-leg balance training corrects the proprioceptive deficits that develop when pain has altered gait for an extended period.
EPAT SHOCKWAVE THERAPY
For Upper Dublin patients with chronic plantar fasciitis — six months or more of symptoms without adequate response to conservative care — Trinity Rehab offers EPAT shockwave therapy. High-energy acoustic waves stimulate blood flow and cellular repair mechanisms in the damaged fascial tissue. The Mayo Clinic identifies EPAT as an evidence-supported option for chronic, treatment-resistant cases. The treatment is non-invasive and delivered in a brief in-clinic series by your physical therapist.
DRY NEEDLING
Dry needling is available for patients whose recovery is complicated by significant myofascial trigger points — bands of tight muscle tissue within the gastrocnemius, soleus, and intrinsic foot muscles that maintain fascial tension even at rest. For tennis players and runners whose calves carry chronic tightness, dry needling accelerates tissue recovery in ways that stretching and manual therapy alone cannot always achieve.
RETURN TO ACTIVITY
The final phase of treatment is the bridge from clinical recovery to unrestricted real-world function. Your therapist builds this systematically:
- For Upper Dublin Sports Center tennis and pickleball players: a return-to-court protocol with progressive session duration and movement complexity
- For Fort Washington Office Park employees: standing tolerance progression and workplace footwear guidance
- For Upper Dublin Cardinals athletes: a sport-specific return program aligned to your competitive season
- For SPARK trail walkers and township runners: a graded return-to-mileage plan that protects the tissue during the most vulnerable early-loading period
Footwear assessment and orthotic recommendations (where appropriate) are built into every return-to-activity plan.
KEEPING HEEL PAIN FROM RETURNING
Prevention in Upper Dublin’s active context requires some deliberate choices:
- Footwear at Fort Washington Office Park matters. Days that include significant walking across the campus deserve footwear with genuine arch support. The foot doesn’t distinguish between “at the office” and “on a run” — unsupportive dress shoes accumulate fascial load just as effectively.
- Warm up before SPARK and UDHS athletic sessions. Two minutes of plantar fascia stretching and calf mobilization before high-intensity activity reduces first-load tissue stress significantly.
- Stretch after tennis and pickleball. The explosive demands of court sports leave the calves tight. Post-session calf and plantar fascia stretching prevents that tension from becoming the chronic tightness that drives plantar fasciitis.
- Track mileage and replace shoes proactively. Running and trail shoes lose meaningful cushioning support between 300 and 500 miles — well before the outsole shows obvious wear. Use a mileage tracker and replace based on use, not appearance.
- Golf post-round stretch. After walking the Manufacturers Golf or Lu Lu Country Club fairways, spend five minutes stretching the calves and plantar fascia before heading to the 19th hole.
WHY UPPER DUBLIN PATIENTS CHOOSE TRINITY REHAB
Trinity Rehab’s one-on-one model means your licensed physical therapist is present and engaged at every session — not managing three patients at once while you perform exercises alone. This is particularly important in plantar fasciitis treatment, where the distinction between therapeutic loading and aggravation depends on real-time clinical judgment.
We accept most major insurance plans. Pennsylvania allows direct access to physical therapy — no physician referral required. Our protocols are grounded in the current evidence base from the American Physical Therapy Association. We also address the downstream biomechanical consequences of untreated plantar fasciitis: the lower back pain and sciatica that can emerge when altered gait mechanics persist for months are within our scope of treatment. See the full range of foot and ankle conditions and conditions we treat.
Inside Our Upper Dublin Clinic
FREQUENTLY ASKED QUESTIONS
Where can I get plantar fasciitis treatment in Upper Dublin, PA?
How long does recovery take?
Can I continue playing tennis or pickleball during treatment?
I’ve had heel pain for over a year. Is it too late for physical therapy to help?
Do I need custom orthotics?
YOUR PATH BACK TO FULL FUNCTION
The SPARK fields, the township trails, the tennis courts, the Fort Washington campus — all of it is still achievable. Plantar fasciitis is a real condition with real daily consequences, but it is also one that physical therapy consistently resolves when the right approach is applied.
Request your appointment at Trinity Rehab today — no referral needed, most insurance accepted.
Sources: JOSPT Clinical Practice Guidelines for Heel Pain/Plantar Fasciitis, 2023 | Mayo Clinic — Plantar Fasciitis | APTA Clinical Practice Guidelines | American Academy of Orthopaedic Surgeons
What Our Patients Say




