PLANTAR FASCIITIS TREATMENT IN PISCATAWAY, NJ
On any weekend morning, Piscataway’s Johnson Park is alive with activity — RVRR members on the riverside paths, families on the trails, soccer players on the fields. Across town, logistics and distribution centers are already humming, with workers standing on concrete floors from open to close.
Piscataway puts its feet to work in remarkable ways. Rutgers students and staff cross campus on foot all day. Chiefs athletes — whose football program has produced multiple NFL players — train year-round. And the township’s pharmaceutical and biotech sector keeps professionals on their feet in labs for extended periods. When this much daily foot loading meets inadequate footwear, tight calf muscles, or structural foot issues, plantar fasciitis is often the result.
Trinity Rehab provides expert plantar fasciitis treatment in Piscataway, helping residents get back to their runs along the Raritan, through their shifts, and through their days — without that familiar stabbing heel pain.

WHAT IS PLANTAR FASCIITIS?
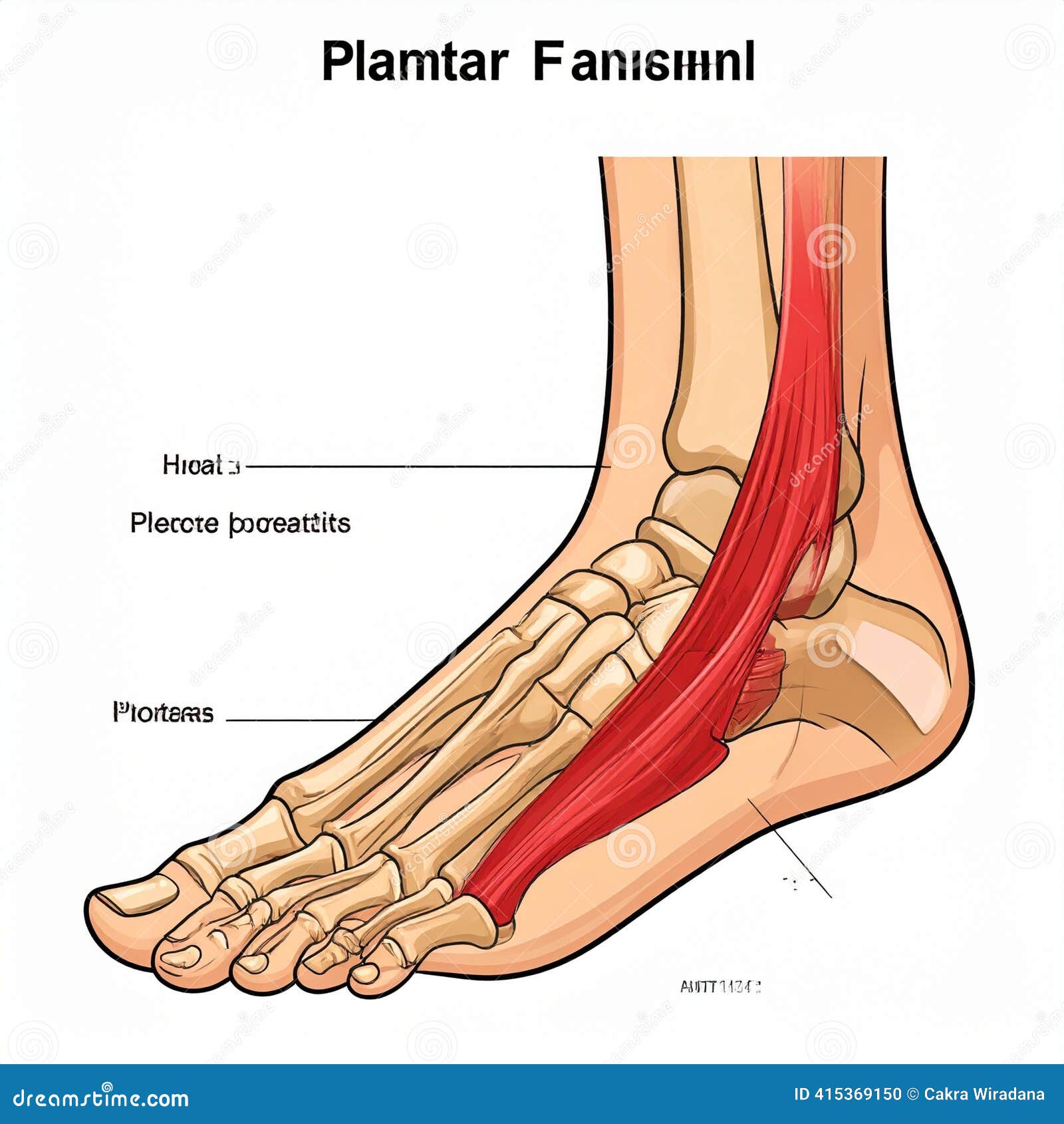
The plantar fascia is a fibrous band of connective tissue spanning the entire bottom of your foot — from the calcaneus (heel bone) to the ball of the foot. It works as both a structural support for the arch and a load-transmitting spring that drives efficient movement. Each step you take loads this tissue repeatedly. Under normal conditions, the fascia handles this demand with ease. Under conditions of sustained overload — too much activity, inadequate recovery, poor biomechanics — it accumulates micro-tears faster than the body can repair them.
The resulting inflammatory cycle is what produces the characteristic sharp, stabbing heel pain that most patients notice first with their morning step out of bed. The tissue stiffens and shortens overnight, then is abruptly stretched under body weight — creating the intense first-step pain that eases gradually as the fascia warms up. Without treatment addressing its root causes, the condition can evolve from acute inflammation into a chronic degenerative state known as plantar fasciopathy, in which the tissue thickens and loses elasticity over months.
The American Academy of Orthopaedic Surgeons estimates 2 million patients receive plantar fasciitis treatment annually. It is the most common cause of heel pain in adults and accounts for 11–15% of all foot complaints requiring professional care.
RELATED CONDITIONS & TREATMENTS
Plantar fasciitis is just one of the many conditions we treat at Trinity Rehab Piscataway. Explore our full range of conditions we treat or learn more about specific treatment approaches:
WHY PISCATAWAY RESIDENTS ARE AT RISK
Piscataway’s specific employment base, recreational habits, and athletic culture create a distinctive set of plantar fasciitis risk factors:
Warehouse and logistics work — Piscataway is home to major logistics operations including the Rockefeller Group Logistics Center, which houses employers such as Best Buy’s regional distribution and SHI International. Workers in these facilities often stand on concrete and epoxy floors for 8–10 hours per day, carrying loads and navigating large warehouse footprints. The cumulative daily loading through the heel is among the most significant occupational drivers of plantar fasciitis in any workforce.
Pharmaceutical and biotech sector — Companies like Amneal Pharmaceuticals, GenScript, and Legend Biotech operate research, manufacturing, and clinical facilities in Piscataway. Lab technicians, researchers, and quality control staff often stand for extended periods on hard laboratory flooring, in footwear that prioritizes safety compliance over biomechanical support.
Rutgers University campus life — Rutgers students, faculty, and staff navigate a large, distributed campus on foot throughout the day. Students who walk between classes on Busch, Livingston, College Avenue, and Cook-Douglass campuses accumulate significant daily mileage — often in fashion sneakers or worn-out athletic shoes that offer minimal arch support or heel cushioning.
Piscataway High School athletics — “NFL High School” — The Chiefs’ nationally recognized football program has produced multiple NFL players and claimed multiple state championships. But beyond football, Piscataway’s athletes compete in soccer, baseball, basketball, volleyball, and wrestling. Year-round, high-intensity training — particularly for running sports and position athletes who practice on turf and field — creates the repetitive heel loading that precedes plantar fasciitis.
Raritan Valley Road Runners and Johnson Park running — The RVRR is an active running club with members who regularly log miles in Johnson Park and along the Raritan River paths. The park’s 478 acres offer both paved and unpaved surfaces, and motivated runners who increase mileage aggressively — especially in spring or after winter downtime — are among the most common plantar fasciitis presentations in active communities.
Tennis and golf — Johnson Park’s tennis courts and nearby Raritan Landing Golf Course keep recreational athletes active through the warmer months. Tennis players who make frequent quick stops and direction changes, and golfers who walk 18 holes in insufficiently supportive shoes, both create concentrated fascial stress that can tip into injury over a season.
HOW PLANTAR FASCIITIS PRESENTS
Plantar fasciitis has a recognizable symptom pattern that is often specific enough to identify before any imaging or specialist evaluation. A Piscataway warehouse worker might notice that their heel is fine when they walk from the car to the facility entrance but becomes increasingly painful as the shift progresses on concrete floors. A Rutgers student might feel sharp heel pain every morning that makes the first few steps to the bathroom agonizing — then eases by the time they leave the dorm room.
Common presentations include:
- First-step morning pain — Stabbing, often severe heel discomfort with the initial weight-bearing steps after waking. Typically eases within five to fifteen minutes as the tissue warms.
- Post-rest flares throughout the day — Rising from a chair, car seat, or lecture hall bench triggers a recurrence of the first-step response.
- Localized heel tenderness — Palpating the inner base of the heel precisely reproduces the pain. This specificity is one of plantar fasciitis’s most reliable diagnostic markers.
- Arch tightness — A pulling, rope-like sensation along the bottom of the foot, most notable in the morning or after extended rest.
- Pain after activity rather than during — Runners may feel fine during a Johnson Park loop but notice intensifying heel pain in the evening afterward.
- Gait compensation and secondary pain — Altered walking mechanics protect the heel in the short term but create compensatory stress in the knee, hip, and lower back.
PHASE-BASED PHYSICAL THERAPY AT TRINITY REHAB PISCATAWAY
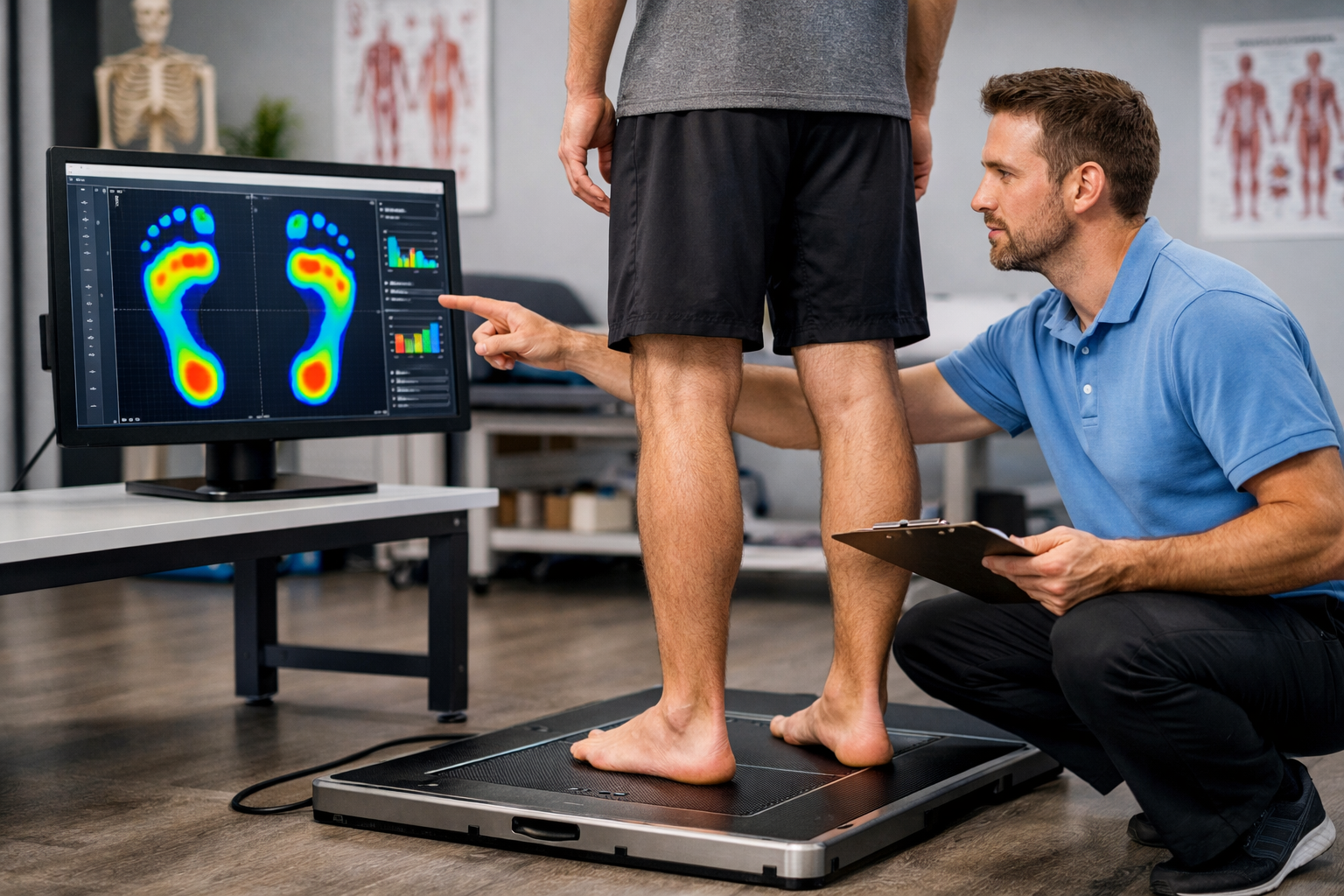
Trinity Rehab’s approach begins with a comprehensive biomechanical evaluation before any treatment starts — assessing gait, foot mechanics, ankle dorsiflexion, calf flexibility, and lower extremity strength. Treatment is structured in phases, each building on the progress of the last.
PHASE 1: REDUCE PAIN AND BEGIN TISSUE HEALING
The first priority is calming the inflammatory cycle so damaged tissue can begin recovering.
Your Piscataway physical therapist will use manual therapy — including hands-on ankle and subtalar joint mobilization — to restore range of motion and reduce mechanical fascial loading. Instrument-assisted soft tissue mobilization (IASTM) breaks down adhesions along the fascia and calf muscles, while myofascial release addresses the trigger points in the gastrocnemius and soleus that amplify heel tension. Research in the Journal of Orthopaedic & Sports Physical Therapy confirms that joint mobilization combined with stretching produces significantly better outcomes than stretching alone for plantar fasciitis.
Kinesiology taping during this phase reduces fascial tension during weight-bearing activities between sessions, allowing the tissue to begin healing without requiring complete rest from work or daily activities.

PHASE 2: RESTORE FLEXIBILITY AND BUILD STRENGTH
With acute pain controlled, treatment shifts to correcting the underlying biomechanical deficits that caused the injury.
A systematic calf stretching program targets both the gastrocnemius (two-joint) and soleus (one-joint) muscles to recover full ankle dorsiflexion. Combined with the plantar fascia-specific toe-extension stretch performed before morning weight-bearing, these exercises directly reduce the fascial tension that sustains the pain cycle. Eccentric heel-drop progressions — slowly lowering from a step under load — build tendon and fascial resilience progressively. Intrinsic foot muscle strengthening through towel scrunches, short-foot exercises, and balance training rebuilds the internal support system that keeps the arch healthy long after formal treatment ends.
For Piscataway warehouse workers, this phase also incorporates exercises that improve endurance in the foot and lower leg musculature — building the capacity to stand for a full shift without heel breakdown.
PHASE 3: RETURN TO FULL ACTIVITY
The final phase prepares patients to return to their full activity level safely and sustainably.
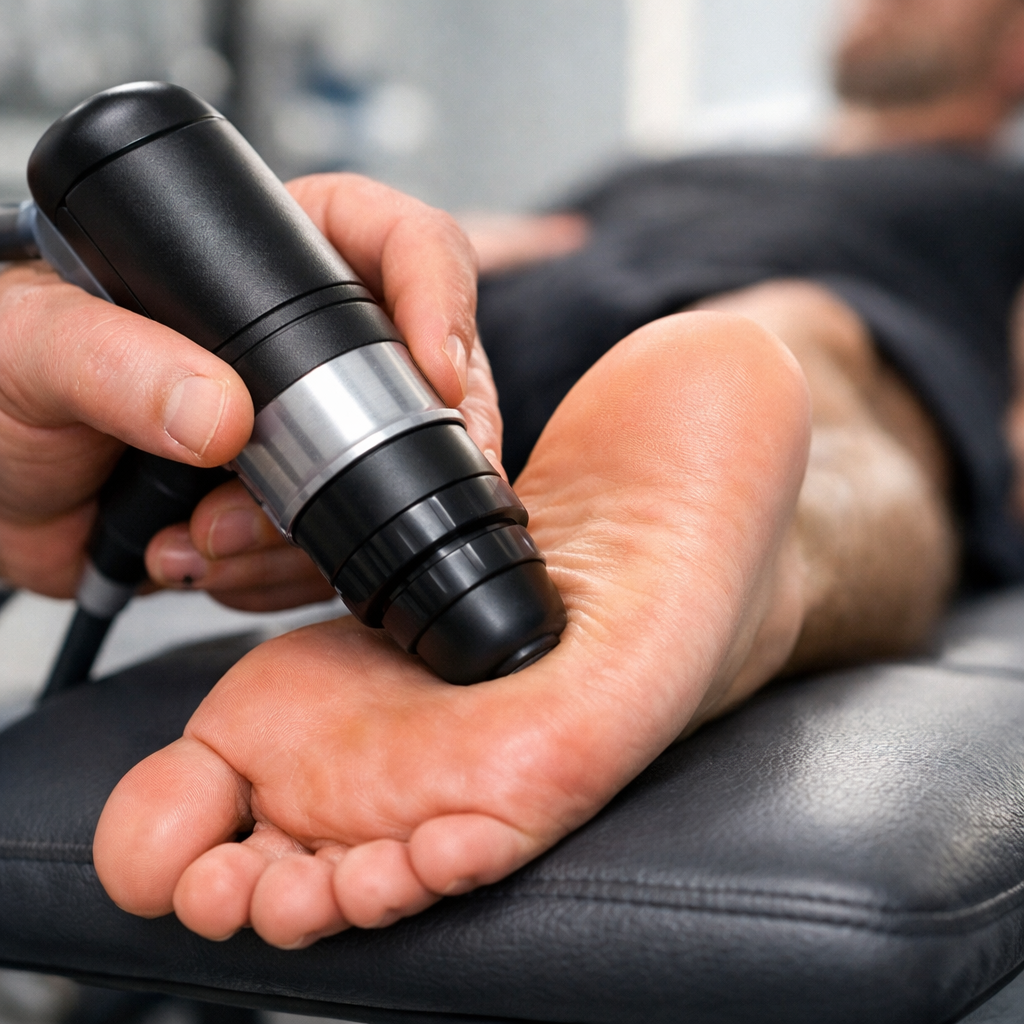
- EPAT shockwave therapy — For patients with chronic plantar fasciitis that has persisted despite earlier treatment, EPAT uses acoustic pressure waves to stimulate deep tissue repair. The Mayo Clinic identifies shockwave therapy as effective for recalcitrant plantar fasciitis. Trinity Rehab offers this treatment directly, without requiring a separate specialist visit.
- Dry needling — Targeting calf and foot trigger points with fine filament needles releases deep muscular tension that conventional stretching cannot fully address, particularly effective for runners and standing workers with chronic calf tightness.
- Activity-specific return programming — Road runners returning to RVRR group runs receive a structured mileage progression plan. Chiefs athletes returning to training receive sport-specific loading guidelines. Warehouse workers returning to full shifts receive occupational conditioning protocols.
- Orthotic and footwear assessment — Many Piscataway patients with flat feet, high arches, or significant overpronation achieve their most durable outcomes with custom orthotics combined with physical therapy. Your therapist will evaluate your mechanics and recommend the appropriate level of support.
PREVENTION: PROTECTING YOUR HEELS IN PISCATAWAY
- Occupational footwear matters — For warehouse and logistics workers, quality anti-fatigue footwear with adequate arch support is not optional. Replace work shoes on a schedule — midsole compression fails well before the exterior shows wear.
- Stretch before your first step — A 30-second plantar fascia stretch and calf elongation before stepping out of bed costs nothing and dramatically reduces first-step pain and recurrence risk.
- Follow the 10% rule at Johnson Park — Raritan Valley Road Runners members who return from winter break or increase mileage for a spring event should add no more than 10% of weekly volume per week. The riverside paths are forgiving, but the fascia has limits.
- Respect the campus mileage — Rutgers students who discover after a semester of daily campus walking that their heels hurt should pay attention to their footwear. A supportive insole in everyday shoes costs less than a month of missed training.
- Warm up before tennis and golf — A brief dynamic warm-up including calf stretches before a tennis session at Johnson Park or a round at Raritan Landing significantly reduces the risk of fascial injury from cold-tissue loading.
WHY PISCATAWAY PATIENTS CHOOSE TRINITY REHAB
Trinity Rehab delivers one-on-one physical therapy — your licensed therapist with you every session, no aides or generic programs. Your plan is built from your evaluation and reflects your life: whether you’re a Chiefs athlete, a Rutgers student, a warehouse shift worker, or an RVRR weekend runner.
We accept most major insurance plans, require no physician referral, and offer scheduling flexibility for shift workers and commuters. View all foot and ankle conditions we treat or explore the full range of conditions.
Inside Our Piscataway Clinic


FREQUENTLY ASKED QUESTIONS
Where can I get plantar fasciitis treatment in Piscataway, NJ?
I work warehouse shifts and can’t take time off — can I still get treatment?
My heels hurt after every run but feel fine during — is that plantar fasciitis?
How is EPAT different from ultrasound therapy?
Can plantar fasciitis cause knee or back pain?
YOUR RECOVERY STARTS IN PISCATAWAY
Whether it’s Johnson Park, the Piscataway High School track, the warehouse floor, or the Rutgers campus route, your daily movement deserves to be pain-free. Trinity Rehab is ready to help.
No physician referral needed. Most major insurance plans accepted.
Sources: Journal of Orthopaedic & Sports Physical Therapy — Clinical Practice Guidelines, Heel Pain/Plantar Fasciitis 2023 | Mayo Clinic — Plantar Fasciitis | American Academy of Orthopaedic Surgeons — Plantar Fasciitis and Bone Spurs | NIH/PMC — Management of Plantar Fasciitis in the Outpatient Setting
What Our Patients Say




