PLANTAR FASCIITIS TREATMENT IN SOMERVILLE, NJ
Picture this: it’s a Saturday morning and you’re planning a run through Washington Valley Park or a lap around Duke Island Park with the Raritan Valley Road Runners. You swing your feet over the side of the bed — and the moment your heel hits the floor, a sharp, stabbing pain stops you cold. That first step feels like stepping on broken glass. If this has become your morning routine, plantar fasciitis may be the culprit, and you don’t have to keep living around it.
At Trinity Rehab in Somerville, our physical therapists work with patients from across Somerset County every week — nurses and staff from Robert Wood Johnson University Hospital Somerset who are on their feet for 12-hour shifts, warehouse employees from the Route 22 and Route 206 corridor, Somerville High School Pioneer athletes pushing through their cross-country seasons, and longtime residents who simply want to walk through Downtown Somerville without dreading every step. Plantar fasciitis is one of the most treatable conditions we see, and recovery is very much within reach.

WHAT IS PLANTAR FASCIITIS?
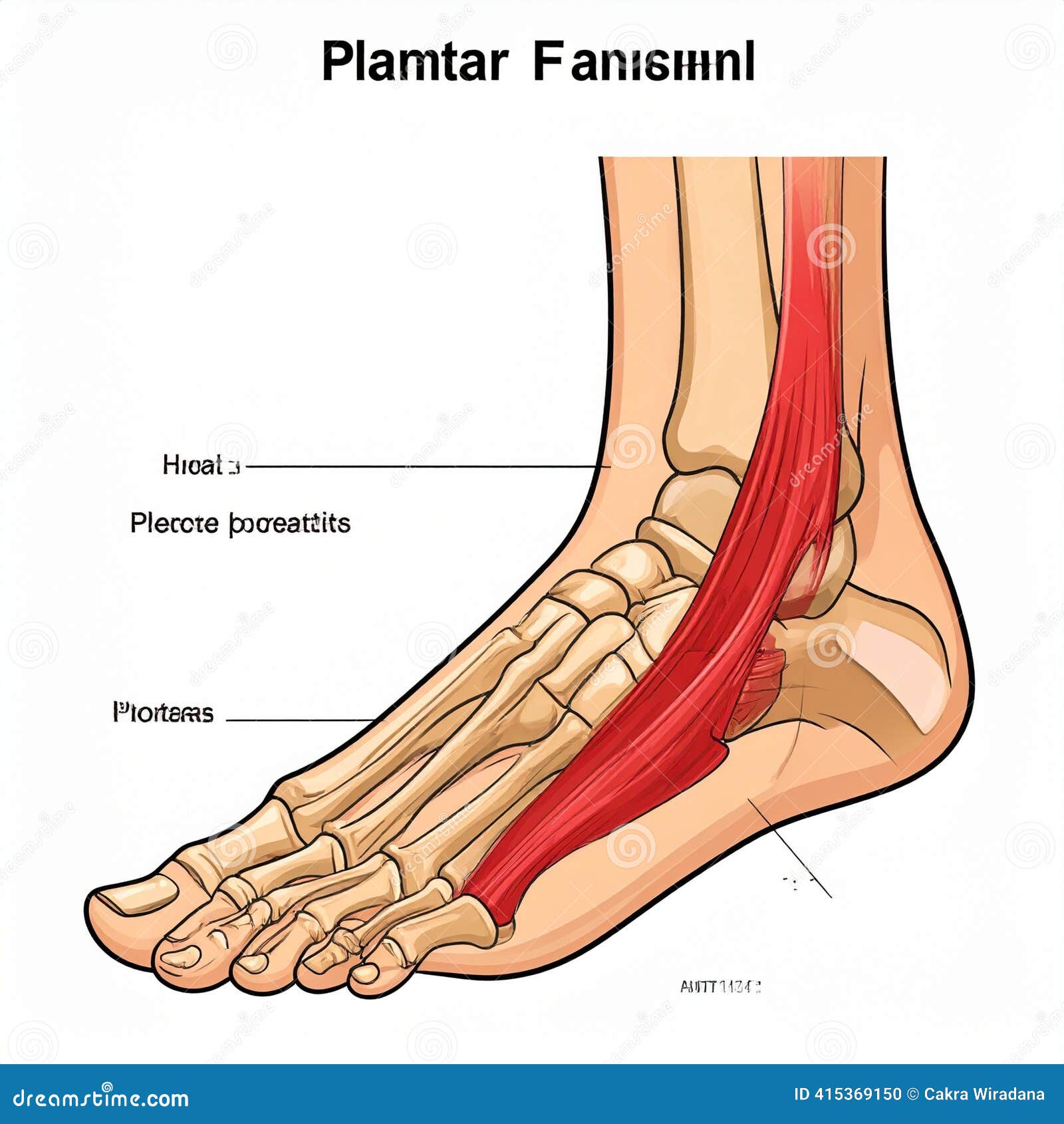
The plantar fascia is a thick band of connective tissue that runs along the sole of your foot, anchoring at the heel bone and fanning forward to your toes. It works like a natural shock absorber, supporting your arch and managing the load of each step through what biomechanists call the windlass mechanism. When that tissue is overloaded through repetitive stress, small micro-tears accumulate faster than the body can repair them, triggering the inflammation and degeneration that define plantar fasciitis.
The result is a pain cycle that can drag on for months — or longer — if it goes untreated. The American Academy of Orthopaedic Surgeons estimates that roughly 2 million Americans are treated for plantar fasciitis each year, making it the single most common source of heel pain in adults. The condition disproportionately affects people in their 40s and 50s, though it is far from limited to that age group.
The encouraging news is that physical therapy — when started early and carried out correctly — resolves the vast majority of plantar fasciitis cases without surgery or injections.
RELATED CONDITIONS & TREATMENTS
Plantar fasciitis is just one of the many conditions we treat at Trinity Rehab Somerville. Explore our full range of conditions we treat or learn more about specific treatment approaches:
WHY SOMERVILLE RESIDENTS DEVELOP HEEL PAIN
Somerville’s mix of occupations and active lifestyle creates several distinct pathways to plantar fasciitis.
Healthcare and service workers at Robert Wood Johnson University Hospital Somerset and area medical offices spend hours on hard institutional floors. Extended standing with minimal variation in weight distribution creates cumulative loading on the plantar fascia that gradually exceeds its tolerance — not through a single injury, but through the relentless addition of micro-stress.
Warehouse and industrial workers along the Route 22, 202, and 206 corridors face a similar occupational risk. Concrete warehouse floors offer essentially no give, and the combination of prolonged standing, carrying loads, and repetitive walking can accelerate tissue breakdown in the heel. Work-related foot injuries like plantar fasciitis are more prevalent in these settings than most people recognize.
Runners and trail enthusiasts who train on the paths through Washington Valley Park or Duke Island Park — or who follow group runs with the Raritan Valley Road Runners — frequently see plantar fasciitis emerge after a jump in weekly mileage, a transition to a different shoe, or a return to training after time off. The repetitive heel strike on packed surfaces stresses the fascia with every mile.
Somerville High School athletes in football, track, cross-country, and soccer spend months in sport-specific training that loads the foot in very particular ways. The Pioneer cross-country runners, in particular, rack up significant volume on varied terrain — the kind of training pattern that can provoke fascial overload if recovery protocols aren’t in place.
Other contributing factors our Somerville patients commonly share include tight calf muscles, worn-out athletic shoes, overpronation, and the natural thinning of the heel’s fat pad that accelerates after age 40.
RECOGNIZING THE SYMPTOMS
Plantar fasciitis has a signature symptom pattern that makes it identifiable — though that doesn’t mean you should wait to have it confirmed.
The defining sign is sharp heel pain with the first steps of the morning. After hours of inactivity, the plantar fascia contracts and stiffens. The sudden load of standing stretches it abruptly, producing the intense, knife-like sensation that so many patients describe as the worst moment of their day. The same phenomenon occurs after sitting at a desk, driving, or resting at midday — the first few steps after any period of non-weight-bearing are characteristically the most painful.
Other patterns to watch for:
- Tenderness directly under or just forward of the heel bone
- A dull ache along the arch that worsens as the day goes on
- Pain that spikes after — but not necessarily during — a run or long walk
- Visible changes in your gait: favoring one side, shortening your stride, or landing differently to protect the heel
- Stiffness that doesn’t fully resolve even after the initial warm-up period
A Somerset County resident who runs the Duke Island Park trails three times a week described it well: “I felt fine during the run, then by the time I got back to my car, my heel was throbbing. Every morning I’d dread getting out of bed.” That classic delayed response and morning stiffness pointed directly to plantar fasciitis, and with a targeted treatment plan, she was back to pain-free running within ten weeks.
If symptoms have persisted longer than two weeks, that’s your cue to seek a professional evaluation. Early intervention consistently leads to faster, more complete recovery.
HOW PHYSICAL THERAPY TREATS PLANTAR FASCIITIS
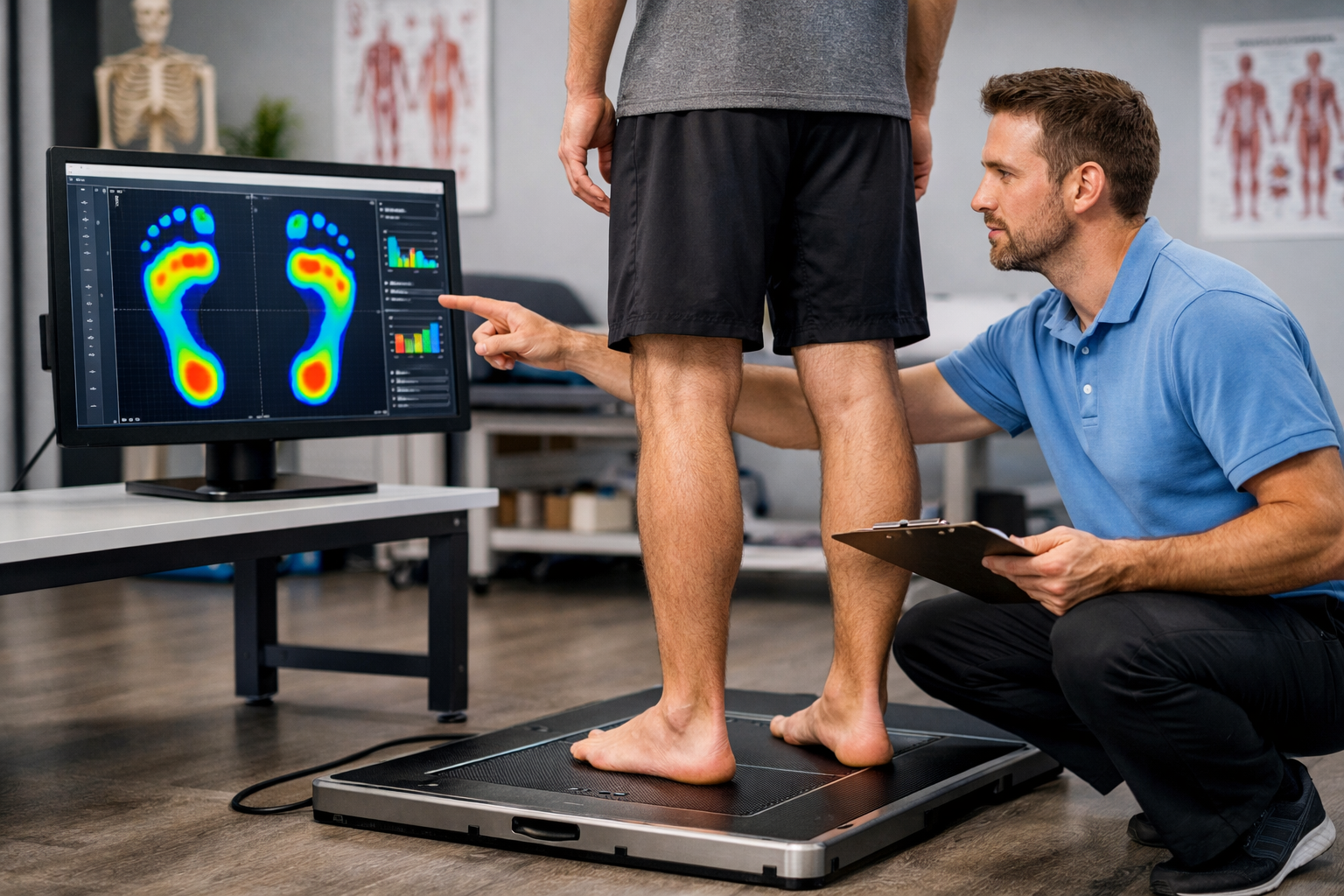
Trinity Rehab’s approach to plantar fasciitis is built around identifying and addressing the specific factors driving your pain — not just managing symptoms. Every treatment plan begins with a thorough assessment of your foot mechanics, ankle mobility, gait pattern, and the biomechanical contributors that are unique to your activity level and lifestyle.
PHASE 1: REDUCING PAIN AND CALMING TISSUE IRRITATION
The first priority is breaking the pain cycle so you can participate actively in your own recovery. During this phase your therapist may use:
Manual therapy — Hands-on joint mobilization of the ankle and subtalar joints restores the range of motion that tight structures steal away. Instrument-assisted soft tissue mobilization (IASTM) breaks down adhesions along the plantar fascia and calf, while myofascial release techniques address trigger points in the intrinsic foot muscles and the Achilles chain. Research published in the Journal of Orthopaedic & Sports Physical Therapy confirms that subtalar joint mobilization combined with stretching produces significantly greater pain relief than conventional treatment alone.
Therapeutic modalities — Therapeutic ultrasound delivers controlled deep-tissue heating that increases local blood flow and accelerates cellular repair. Kinesiology taping can offload the plantar fascia between sessions, reducing strain during daily activity.
Initial stretching — Plantar fascia-specific stretches (dorsiflexing the toes before the first step of the morning) and calf stretches begin immediately. These two interventions alone have strong clinical evidence supporting their role in reducing first-step pain.

PHASE 2: REBUILDING STRENGTH AND LOAD TOLERANCE
Once pain is manageable, the focus shifts to rebuilding the foot’s structural capacity so it can handle the demands you place on it.
Eccentric calf loading is a cornerstone of this phase — slowly lowering the heel off a step trains the calf-Achilles-fascia chain to absorb force rather than simply transfer it to already-sensitive tissue. Intrinsic foot strengthening through exercises like towel scrunches and the “short foot” technique builds the small muscles that support the arch from the inside. Progressive balance training using single-leg progressions corrects the neuromuscular deficits that often accompany altered gait and contribute to abnormal foot loading.
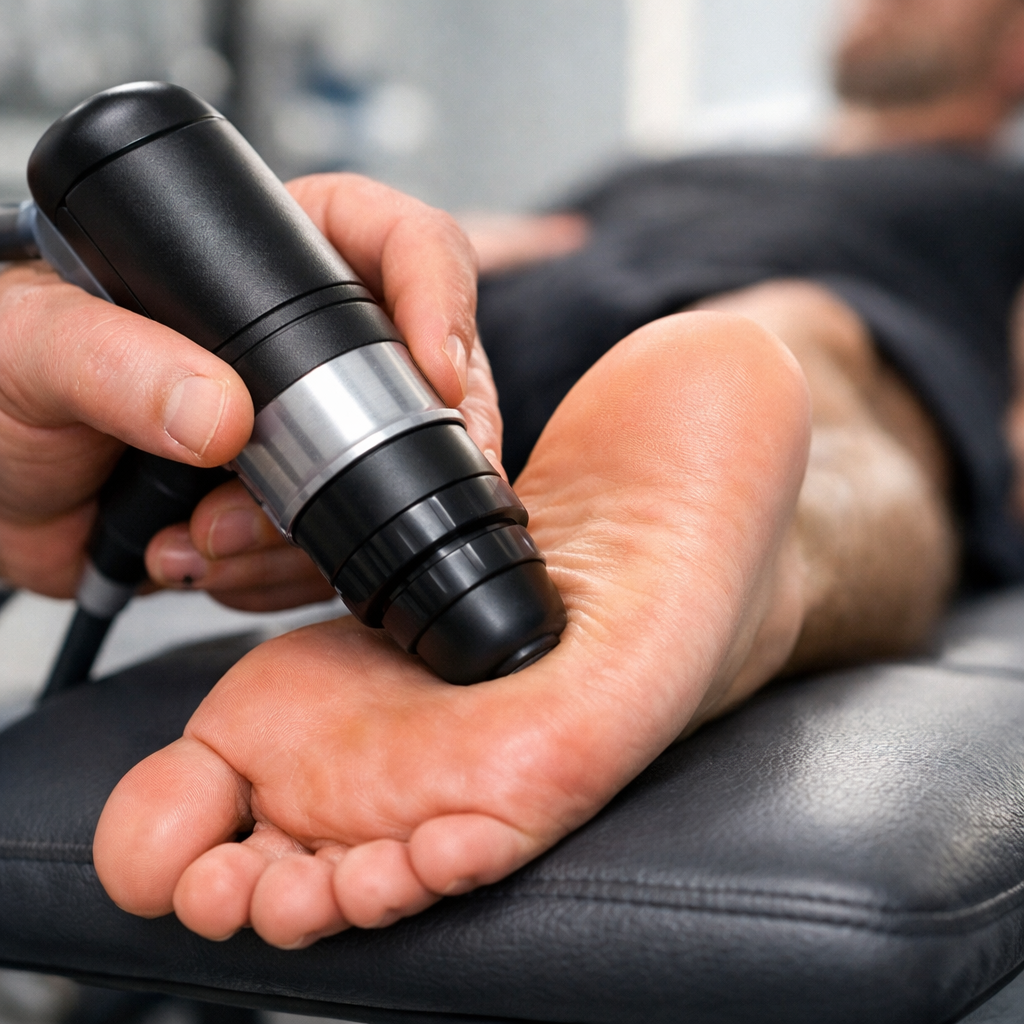
For patients with persistent or chronic presentations, EPAT shockwave therapy and dry needling are available at Trinity Rehab Somerville. EPAT uses acoustic pressure waves to stimulate blood flow and tissue regeneration in the damaged fascia — the Mayo Clinic recognizes it as an effective intervention for chronic cases. Dry needling targets trigger points in the soleus, gastrocnemius, and foot intrinsics that perpetuate fascial tension.
PHASE 3: RETURN TO ACTIVITY AND LONG-TERM PREVENTION
The final phase bridges the gap between the clinic and your real life — whether that means returning to a full nursing shift, competing in the Pioneer cross-country season, or finishing a long run through Washington Valley Park pain-free. Your therapist will build a structured return-to-activity protocol matched to your specific goals, along with footwear guidance, orthotic recommendations where appropriate, and a maintenance routine designed to prevent recurrence.
KEEPING HEEL PAIN FROM COMING BACK
Recovery is more than just the absence of pain. These prevention strategies, tailored for life in Somerville, will help protect your feet for the long term:
- Replace your running shoes on schedule. If you train with the Raritan Valley Road Runners or run the Duke Island Park trails regularly, track your mileage. Most running shoes lose meaningful cushioning support between 300 and 500 miles — well before the upper shows visible wear.
- Warm up before your Pioneer-style workouts. A brief plantar fascia stretch and calf mobilization before morning runs dramatically reduces the first-load stress on the tissue.
- Wear supportive footwear at work. If you’re on your feet at RWJ Somerset or in a warehouse environment, invest in occupational footwear with real arch support. Clogs, flat sneakers, and worn-out work shoes offer little protection against the cumulative load of a long shift.
- Increase activity gradually. Use the 10% rule — don’t add more than 10% to your weekly training volume from one week to the next, and allow adequate recovery between hard efforts.
- Address tightness proactively. If you notice calf tightness or morning heel stiffness starting to return, treat it as an early warning signal and resume your stretching routine before it escalates.
WHY SOMERVILLE PATIENTS CHOOSE TRINITY REHAB
Trinity Rehab’s Somerville clinic offers the kind of personalized attention that makes a real difference in plantar fasciitis outcomes. Every session is conducted one-on-one with your licensed physical therapist — you are never handed off to an aide or left to run through exercises unsupervised. Your therapist will monitor your progress at each visit and adapt your plan based on how your tissue is responding.
We accept most major insurance plans, no physician referral is required to start treatment, and our scheduling options accommodate the demands of busy work and family schedules common in the Somerville area. Whether you work shifts at RWJ Somerset, commute to a job in Central Jersey, or coach your child’s soccer team on the weekends, we’ll work around your calendar.
Our treatment protocols reflect the latest clinical guidelines from the American Physical Therapy Association, and our therapists have extensive experience with the full spectrum of foot and ankle conditions that affect active adults.
Inside Our Somerville Clinic
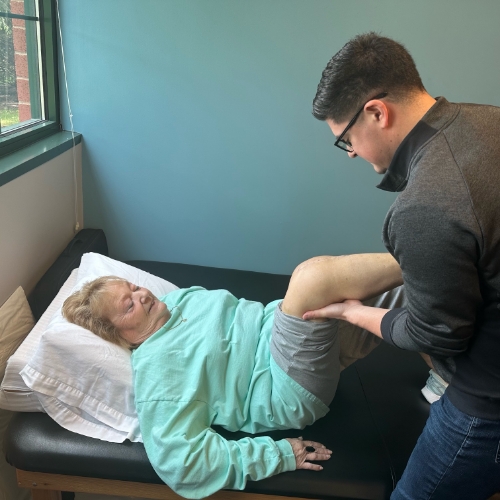
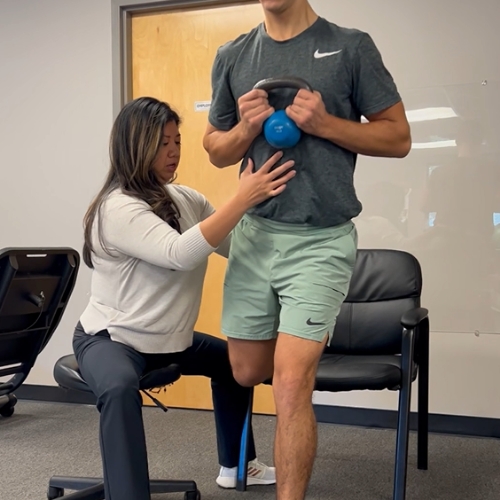
FREQUENTLY ASKED QUESTIONS
How long will it take to recover from plantar fasciitis at Trinity Rehab Somerville?
Where can I get plantar fasciitis treatment in Somerville, NJ?
I’m a runner — do I have to stop completely during treatment?
Can plantar fasciitis cause other problems beyond heel pain?
Do I need custom orthotics?
TAKE THE FIRST STEP TOWARD PAIN-FREE LIVING
Heel pain shouldn’t be the thing that keeps you off the trails, out of the gym, or dreading your morning. The team at Trinity Rehab Somerville is ready to help you get back to all of it — the Saturday runs, the long shifts, the weekend games — without pain defining your limits.
Getting started is simple: request your appointment online, come in for a thorough evaluation, and begin a treatment plan designed specifically for your body and your goals. No physician referral needed. Most insurance plans accepted.
Sources: JOSPT Clinical Practice Guidelines for Heel Pain/Plantar Fasciitis, 2023 | Mayo Clinic — Plantar Fasciitis | APTA Clinical Practice Guidelines | American Academy of Orthopaedic Surgeons
What Our Patients Say




