Lumbar Disc Herniation Treatment | Physical Therapy in NJ & PA
When a Disc in Your Lower Back Won’t Let You Move
One morning you bend over to tie your shoes, and a bolt of pain shoots from your lower back down through your leg. Sitting becomes unbearable. Standing brings only partial relief. If this describes what you are experiencing, you may be dealing with a lumbar disc herniation — one of the most common causes of back pain and sciatica in adults. At Trinity Rehab, we specialize in personalized, one-on-one physical therapy designed to reduce your pain, restore your function, and help you get back to the life you enjoy — without relying on medications or invasive procedures.
Why Lumbar Disc Herniation Relief Matters
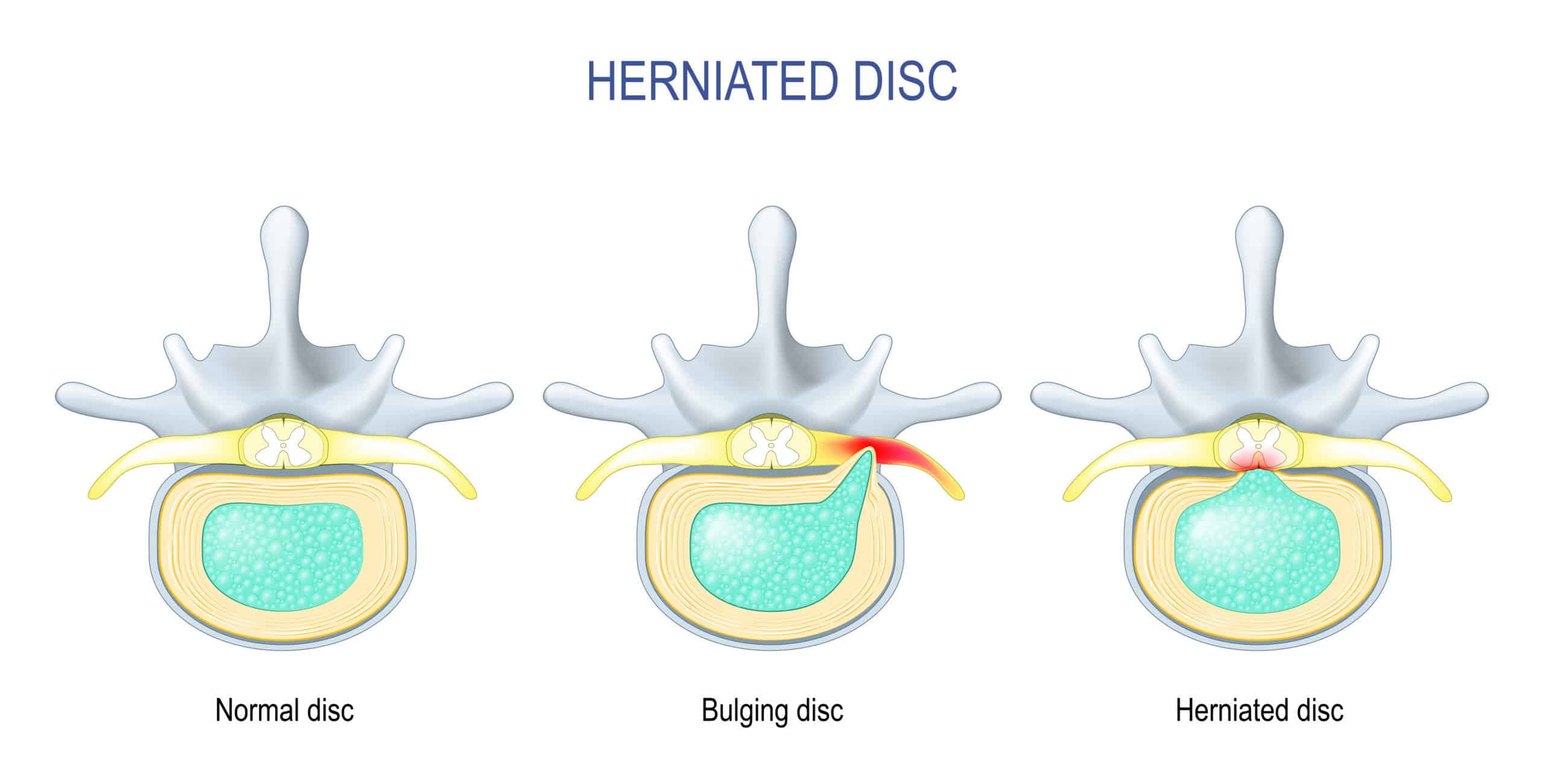
Your lumbar spine bears the majority of your body’s weight and absorbs significant forces during everyday movements. A herniated disc occurs when the gel-like material inside a spinal disc pushes through a tear in the disc’s outer layer, pressing on nearby nerves and causing pain, numbness, and weakness that radiate into your hip, buttock, and leg. Research published in Deutsches Ärzteblatt International confirms that symptoms resolve in 60 to 80 percent of patients within 6 to 12 weeks with conservative treatment. According to StatPearls (NCBI), over 85 to 90 percent of patients with an acute herniated disc experience relief without surgery.
The impact of a herniated disc extends beyond physical pain. Many patients report difficulty sleeping, reduced work productivity, anxiety about their condition, and frustration with limitations on activities they once took for granted. The good news is that a herniated disc is a treatable condition, and the vast majority of patients respond well to conservative care when guided by an experienced physical therapist.
Common Causes of Lumbar Disc Herniation
Understanding what led to your disc herniation helps guide your treatment and prevent recurrence. The most common causes include:
- Age-related disc degeneration — as you age, your spinal discs lose water content and become more vulnerable to tears. Most herniations occur between ages 30 and 50.
- Repetitive bending and lifting — jobs or activities involving frequent forward bending, heavy lifting, or twisting place repeated stress on the lumbar discs at L4-L5 and L5-S1.
- Sedentary lifestyle and prolonged sitting — sitting increases pressure on lumbar discs by up to 40 percent compared to standing.
- Poor body mechanics — lifting with your back instead of your legs increases disc strain.
- Excess body weight — additional weight shifts your center of gravity forward, placing extra compressive force on the lower lumbar segments.
- Sudden trauma — a fall, car accident, or sudden impact can cause immediate disc herniation.
- Smoking — reduces blood flow to spinal discs, accelerating disc degeneration and slowing healing.
- Genetic predisposition — some people inherit a greater susceptibility to disc problems.
Symptoms Patients Often Notice
Lumbar disc herniation symptoms vary depending on the size, location, and severity of the herniation, and whether it compresses a nearby nerve root. Common symptoms include:
- Sharp, burning, or shooting pain in the lower back that radiates into the buttock, thigh, calf, or foot (sciatica)
- Numbness or tingling in the leg or foot, following a specific nerve pathway
- Muscle weakness in the leg, making it difficult to lift your foot (foot drop) or climb stairs
- Pain that worsens with sitting, bending forward, coughing, or sneezing
- Stiffness in the lower back, especially after prolonged sitting or upon waking
- Relief when lying down or walking short distances
- Pain that follows one side of your body (unilateral symptoms are common with nerve compression)
- Difficulty finding a comfortable sleeping position
It is important to note that some patients experience mild herniation with no symptoms at all. Imaging studies show that many asymptomatic herniations are discovered incidentally and require no treatment. This is why a proper evaluation by a physical therapist is essential — we focus on your symptoms and functional limitations, not just the imaging findings.
When to Seek Physical Therapy for a Herniated Disc
Signs You Should See a Physical Therapist
If you suspect you have a lumbar disc herniation, seeking prompt evaluation and treatment can prevent symptoms from worsening and help you avoid months of lost function. Consider scheduling a physical therapy appointment if you experience:
- Pain in your lower back and leg that persists for more than two weeks, even with rest and over-the-counter medications
- Radiating pain, numbness, or tingling that follows a specific pattern down one leg (a strong sign of nerve involvement)
- Difficulty performing daily activities such as bending, lifting, sitting at a desk, or walking without pain
- Weakness in your leg that affects your ability to walk, climb stairs, or maintain your balance
- Pain that is severe enough to disrupt your sleep or interfere with work productivity
- Symptoms that are getting progressively worse despite conservative home management
Early Intervention Makes a Difference
The timing of your physical therapy intervention matters significantly. Research published in the Journal of Orthopaedic & Sports Physical Therapy demonstrates that patients who begin physical therapy within the first two to four weeks of symptom onset experience faster pain relief, return to work sooner, and are less likely to develop chronic pain patterns. When you delay treatment, pain can cause protective muscle guarding that perpetuates stiffness and weakness, creating a prolonged recovery cycle.
Early intervention also helps prevent maladaptive movement patterns. When your body hurts, you naturally move differently — favoring one side, avoiding certain positions, or limiting your range of motion. Over time, these compensatory patterns strengthen and become habitual, making recovery more difficult even after pain subsides. A physical therapist identifies and corrects these patterns early, accelerating your return to normal, pain-free movement. Additionally, starting physical therapy promptly reduces your reliance on pain medications and the risk of developing psychological fear-avoidance behaviors that can prolong disability.
Understanding the Types of Lumbar Disc Herniation
Disc Protrusion vs. Disc Extrusion vs. Sequestration
Disc herniations exist on a spectrum, categorized by the extent of damage and how the disc material has displaced:
- Disc Protrusion — The disc material pushes outward but the outer fibers (annulus fibrosus) remain largely intact. Think of it as bulging without breaking through. A protrusion typically causes localized back pain and mild to moderate referred symptoms into the leg.
- Disc Extrusion — The gel-like nucleus pulposus breaks through the outer layer of the disc and extends into the spinal canal. The material is still connected to the disc space, but now protrudes significantly into the space where nerves travel. This type typically causes more pronounced radiating pain, numbness, and weakness.
- Sequestration — A piece of the nucleus pulposus breaks off and migrates away from the disc space into the spinal canal. This is the most severe form of herniation and often causes the most significant nerve compression and symptoms. The good news is that sequestered fragments can be reabsorbed by your body over time, and physical therapy is still the first-line treatment.
Most patients with disc protrusion experience excellent recovery with physical therapy alone. Many patients with extrusion also respond well to conservative treatment. Even some patients with sequestration improve significantly with physical therapy and avoid surgery.
Which Lumbar Discs Are Most Commonly Affected
The lumbar spine has five discs, labeled L1-L2 through L5-S1 (where S1 is the sacrum). Two segments account for over 85 percent of herniated discs:
- L4-L5 (the fourth and fifth lumbar vertebrae) — This is the second most common site. Herniation here compresses the L5 nerve root, causing pain, numbness, or weakness that radiates down the outside of the leg, across the top of the foot, and into the big toe. Patients often report difficulty lifting their foot upward (foot drop is a classic sign).
- L5-S1 (the lowest lumbar disc, above the sacrum) — This is the most common herniation site because it bears the greatest load and experiences the most stress during bending and lifting. Herniation here typically compresses the S1 nerve root, causing pain that radiates into the buttock, back and outer thigh, calf, and bottom of the foot. Many patients report a burning sensation in the buttock.
Less commonly, herniations occur at L3-L4, L2-L3, or L1-L2, but these represent only about 10 to 15 percent of cases. Your physical therapist will assess your pain pattern, numbness distribution, and weakness to identify which nerve root is involved, even before reviewing imaging studies.
How Herniated Disc Physical Therapy Restores Function
At Trinity Rehab, your treatment begins with a thorough one-on-one evaluation by a licensed physical therapist who assesses your pain patterns, range of motion, strength, nerve function, and how the herniation affects your daily life. From there, we create a personalized treatment plan designed to reduce your symptoms and restore your ability to move confidently. Every patient’s herniation and recovery is unique, which is why we never use a one-size-fits-all approach.
Phase 1: Pain Reduction and Nerve Calming
During the first two to three weeks of treatment, your primary goal is reducing acute pain and inflammation irritating the affected nerve root. Your therapist uses directional preference exercises (based on the McKenzie Method) to identify specific movements that centralize your pain — moving symptoms away from your leg and back toward your lower back where they are easier to manage. This process, called centralization, signals that the disc material is repositioning favorably relative to the nerve root.
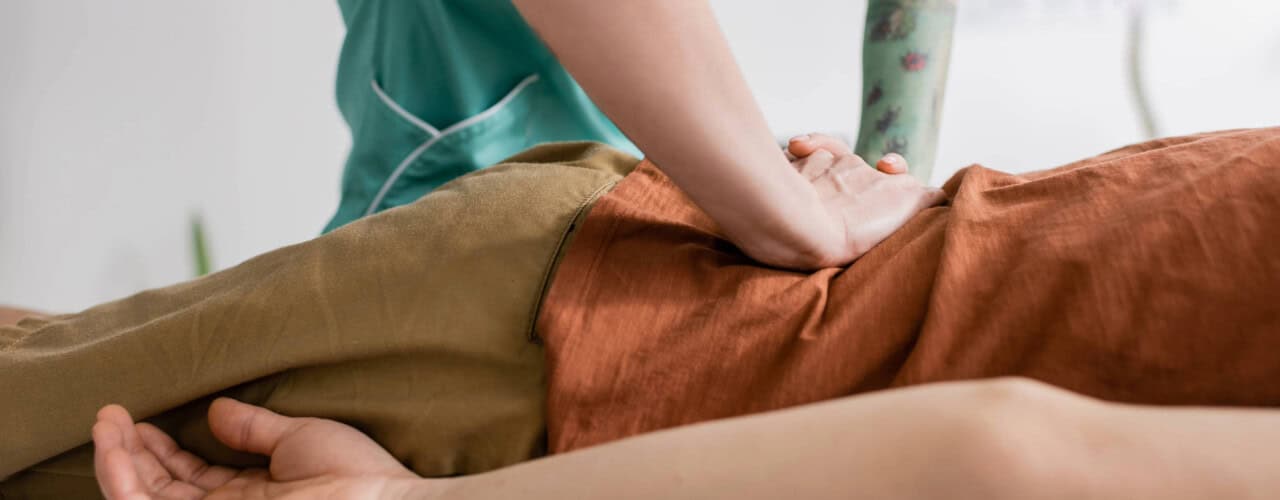
Alongside directional exercises, your therapist applies manual therapy techniques including gentle mobilization, soft tissue massage, and myofascial release to reduce muscle guarding and improve blood flow to the affected area. Postural education is critical during this phase — your therapist teaches you how to sit, stand, bend, and lie down in ways that minimize pressure on the herniated disc and relieve nerve irritation. Many patients find that specific positions provide immediate relief, while others cause pain to worsen or radiate further down the leg. Your therapist helps you identify your personal relief positions and postures to use throughout the day.
Heat and ice application, along with electrical stimulation modalities when appropriate, help reduce pain and muscle spasm during this acute phase. Most patients notice meaningful pain reduction within the first two to three weeks when Phase 1 protocols are followed consistently.
Phase 2: Core Stabilization and Progressive Strengthening
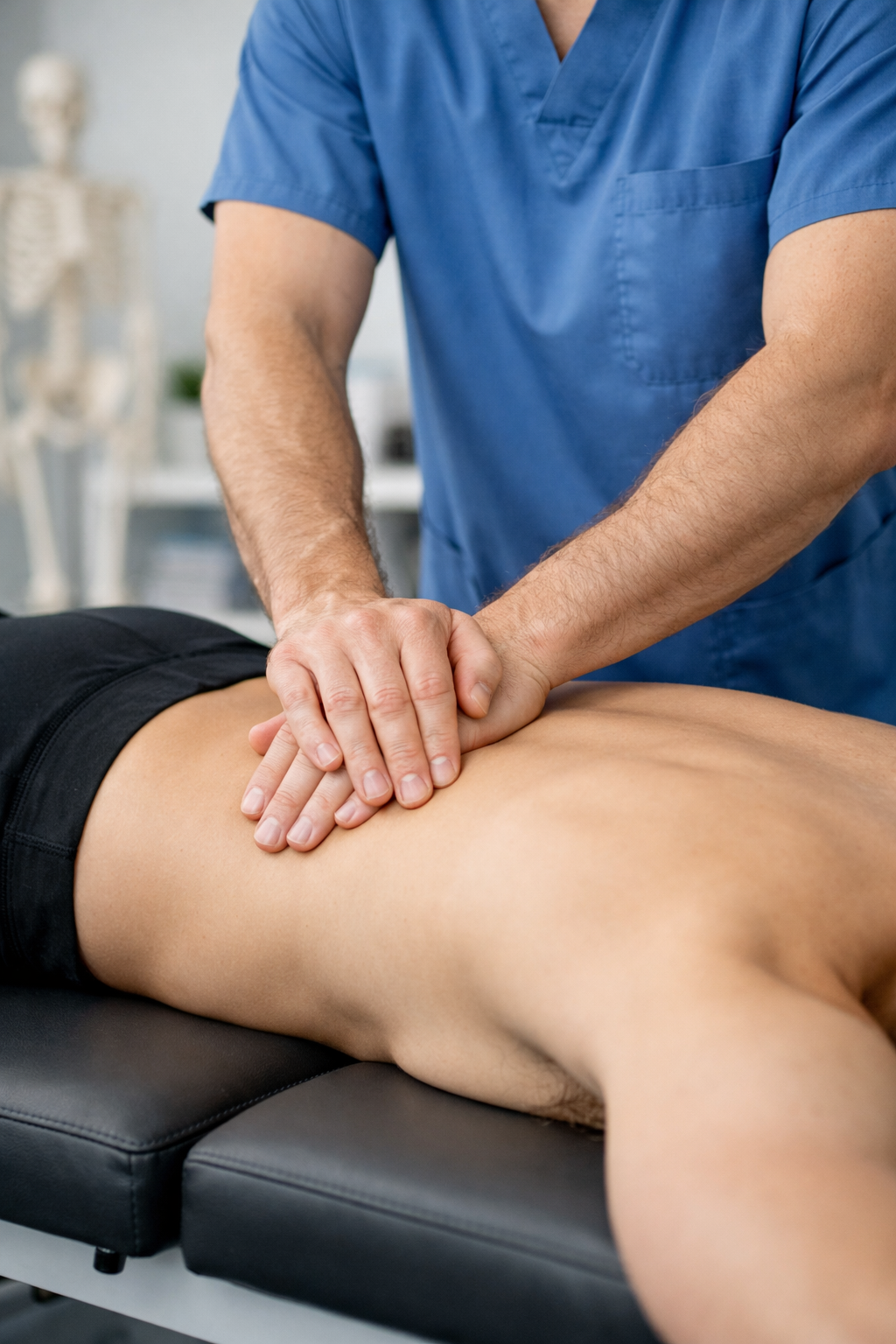
Once acute pain begins to subside (typically after weeks two to four), the focus shifts to rebuilding the muscular support system your spine depends on. Your deep core muscles — particularly the multifidus and transverse abdominis — act as natural braces for your lumbar spine. When these muscles are weak or unable to activate properly, your spine becomes unstable and vulnerable to re-injury.
Your therapist guides you through progressive core activation exercises beginning with gentle, pain-free movements. You will learn to engage your deep abdominal muscles without holding your breath, using exercises like dead bugs, bird dogs, and modified planks. As your tolerance improves, exercises progress to include hip and gluteal strengthening, quadriceps activation, and hamstring engagement — all critical for supporting your lumbar spine during functional movements.
This phase typically spans weeks three through eight, though your progression depends on your pain levels and how quickly you regain strength. Your therapist continuously monitors your movement quality and pain response, adjusting exercises to keep you challenged without aggravating your symptoms. By the end of Phase 2, most patients report significant functional improvements and return to many activities they thought were lost.
Phase 3: Return to Activity and Long-Term Prevention
The final phase, typically weeks six through twelve or beyond, prepares you to return to work, exercise, sports, and daily life with confidence. Your therapist designs sport-specific or work-specific rehabilitation programs that replicate the movements and demands you will encounter in your daily life. If you are an athlete, you will perform sport-specific drills. If you have a desk job, we will incorporate sitting tolerance and proper workstation mechanics. If your work involves heavy lifting, we will progress you through controlled lifting patterns with proper body mechanics.
Functional movement training during this phase includes dynamic balance exercises, agility work, and integrated strength training that mimics real-world demands. Your therapist also teaches you a customized independent home exercise program that becomes your maintenance routine for long-term spinal health. This program — typically 15 to 20 minutes performed three to four times per week — helps prevent recurrence and maintains the strength and mobility you have worked hard to restore.
What to Expect During Your Physical Therapy Program
Your Initial Evaluation
Your first visit at Trinity Rehab typically lasts 60 minutes and is entirely one-on-one with a licensed physical therapist. During this evaluation, your therapist conducts a detailed interview about your pain history, symptom onset, activities that make pain worse or better, your work and lifestyle demands, and your recovery goals.
Your therapist then performs a comprehensive physical examination including assessment of your posture, spinal range of motion, muscle strength testing, palpation of your lumbar spine and surrounding structures, and orthopedic special tests designed to identify nerve involvement and assess your disc herniation severity. If you have had recent imaging (MRI, CT, or X-rays), your therapist reviews these with you and explains what the findings mean in relation to your symptoms.
Based on this evaluation, your therapist explains their findings in language you can understand, answers your questions, and collaboratively develops a treatment plan. You will learn what exercises and modifications you can begin immediately, how often you should attend sessions, and realistic expectations for recovery timing.
Your Treatment Timeline
Most patients with lumbar disc herniation follow a general timeline, though individual recovery varies:
- Weeks 1-2 — You will attend physical therapy 2-3 times per week. Focus is pain reduction, nerve calming, and learning relief positions and postures. Many patients notice meaningful pain reduction by the end of week two.
- Weeks 3-4 — Frequency may decrease to 2 times per week as pain diminishes. Phase 2 core stabilization begins. Pain that was 8/10 is now 4-5/10.
- Weeks 5-8 — Sessions drop to 1-2 times per week. Most patients report 50-70 percent functional improvement by weeks 6-8.
- Weeks 9-12 — Sessions may continue 1 time per week or transition to every other week. You are cleared for full return to work and most activities.
- After 12 weeks — Most patients discharge from physical therapy or transition to maintenance programming.
Measuring Your Progress
Objective tracking of your progress motivates continued effort and helps your therapist refine your treatment plan. Your Trinity Rehab physical therapist uses several methods to measure improvement:
- Numeric Pain Rating Scale — You will rate your pain from 0-10 at each visit. Most patients track pain decreasing from initial ratings of 6-8 down to 0-2 by discharge.
- Range of Motion Testing — Your therapist measures spinal movement at baseline and tracks improvement.
- Strength Testing — Using manual muscle testing and functional strength assessments, your therapist documents increasing strength.
- Functional Assessments — Tests like the Oswestry Disability Index (ODI) measure your ability to perform daily activities.
- Walking Distance and Duration — Many patients begin therapy barely able to walk a block without pain. Tracking increasing walking tolerance is a powerful success metric.
Advanced Technology
For patients with chronic disc pain, Trinity Rehab offers advanced technologies that accelerate tissue healing and enhance pain relief when physical therapy alone reaches a plateau.
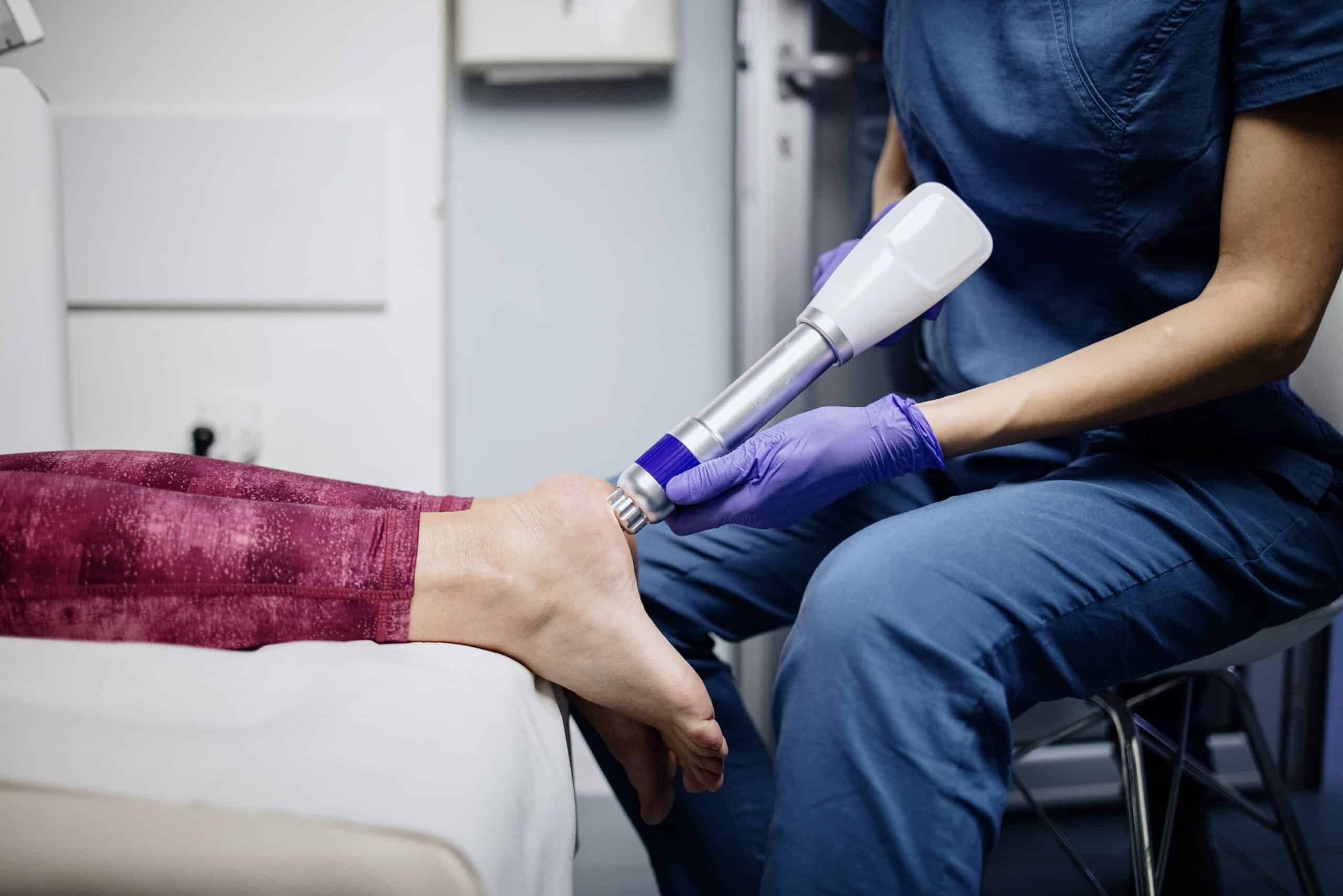
EPAT (Extracorporeal Pulse Activation Technology) uses acoustic pulse energy to stimulate blood flow, promote tissue regeneration, and reduce chronic inflammation in the lumbar region. Sessions are typically 15-20 minutes and performed once or twice weekly for three to four weeks.
Dry Needling is an advanced technique using a thin filiform needle to treat myofascial trigger points and muscle tension in the lumbar paraspinals and surrounding musculature. Patients with herniated discs often develop tight, guarded muscles that persist even as nerve pain improves. Dry needling reduces this muscle tension and improves your therapist’s ability to progress strengthening exercises.
AlterG Anti-Gravity Treadmill reduces your effective body weight, allowing you to walk or run with less pressure on your lumbar spine and lower extremities. You can start at 30-50 percent body weight and gradually increase toward full weight-bearing as tolerated.
How to Prevent Lumbar Disc Herniation From Returning
Recovery does not end when your symptoms resolve. Preventing recurrence is a critical part of your rehabilitation plan. Most reherniations occur within the first three to six months after return to activity, so maintaining your exercise routine during this window is essential.
- Maintain a strong core — continue stabilization exercises at least three times per week. This is not temporary; it is a lifelong practice that protects your spine.
- Practice proper lifting mechanics — always bend at the hips and knees, keep the load close to your body, and avoid twisting while holding weight.
- Stay active and avoid prolonged sitting — stand and move every 30 to 45 minutes. Walking, swimming, and cycling are excellent low-impact activities.
- Use ergonomic support — lumbar support at your desk, in your car, and at home.
- Maintain a healthy weight — reducing excess weight decreases compressive forces on your lumbar spine.
- Practice proper sleep posture — sleep on your back with a pillow under your knees, or on your side with a pillow between your knees. Avoid sleeping on your stomach.
- Invest in proper footwear — shoes with adequate cushioning and arch support reduce impact forces transmitted to your spine.
- Incorporate regular stretching — tight hip flexors, hamstrings, and piriformis muscles increase lumbar spine stress. Dedicate 5-10 minutes daily to stretching these areas.
- Manage stress and sleep — chronic stress and poor sleep increase muscle tension and reduce your body’s healing capacity.
Why Patients Choose Trinity Rehab
- One-on-one care, every visit — you work directly with a licensed physical therapist for the full duration of every session. No aides, no group classes, no rotating between multiple clinicians. This continuity of care enables faster recovery and better outcomes.
- Evidence-based treatment protocols — McKenzie Method, manual therapy, dry needling, and EPAT technology proven to accelerate tissue healing. Our treatment approach is built on peer-reviewed evidence, not outdated protocols.
- Convenient locations across NJ and PA — with 27 clinics throughout the region, expert herniated disc treatment is always close to home or work.
- Insurance-friendly and transparent — we work with most major insurance plans and provide clear communication about your coverage and costs upfront.
- A track record of results — thousands of patients have recovered from lumbar disc herniations without surgery. Many return to us for future injuries because they have experienced our commitment firsthand.
What Our Patients Say
Frequently Asked Questions
Can a lumbar disc herniation heal without surgery?
How long does physical therapy take for a herniated disc?
Is it safe to exercise with a herniated disc?
What is the difference between a bulging disc and a herniated disc?
When should I consider surgery for a herniated disc?
Can I work while recovering from a herniated disc?
What sleeping position is best for a herniated disc?
How do I know if my herniated disc is getting better?
Getting Back to What Matters
A lumbar disc herniation can feel overwhelming, but it does not have to define your life. With the right physical therapy approach, most patients recover fully and return to the activities that matter most — whether that means playing with your kids, getting back to work, returning to the gym, or simply sitting comfortably again. At Trinity Rehab, we are committed to helping you move past the pain and reclaim your function. Our experienced physical therapists will guide you through every stage of recovery with a personalized plan built around your goals. The first step is scheduling an evaluation at one of our 27 convenient locations.
Find Lumbar Disc Herniation Treatment Near You
New Jersey Locations
- Brick, NJ
- Cherry Hill, NJ
- Clark, NJ
- Clifton, NJ
- East Brunswick, NJ
- East Windsor, NJ
- Emerson, NJ
- Flemington, NJ
- Hamilton, NJ
- Howell, NJ
- Manalapan, NJ
- Matawan, NJ
- Metuchen, NJ
- Middletown, NJ
- Piscataway, NJ
- Sewell, NJ
- Shrewsbury, NJ
- Somerset, NJ
- Somerville, NJ
- Sparta, NJ
- Toms River, NJ
- Warren, NJ
- Wayne, NJ
- Woodbridge, NJ
Pennsylvania Locations
Other Conditions We Treat
Trinity Rehab specializes in treating a wide range of orthopedic and neurological conditions. If you are experiencing pain or mobility limitations from another condition, we can help.
Sources
- Lumbar Disc Herniation — StatPearls, NCBI Bookshelf
- Lumbar Disc Herniation: The Significance of Symptom Duration — Deutsches Arzteblatt International
- Management of Lumbar Disc Herniation: A Systematic Review — Cureus
- Early Physical Therapy Intervention for Acute Disc Herniation — Journal of Orthopaedic & Sports Physical Therapy
