Spinal Stenosis Treatment
Walking used to be something you never thought twice about. Now, every trip to the grocery store, every flight of stairs comes with a familiar ache in your lower back that radiates into your legs — growing heavier with each step until you have no choice but to stop, lean forward, and wait for the pressure to ease.
If this sounds like your daily reality, you may be dealing with spinal stenosis — a progressive narrowing of the spaces within your spine that puts pressure on the nerves. According to the NIH, lumbar spinal stenosis affects 11 percent of the general population and is the most common reason for spinal surgery in adults over 65. But surgery is far from the only option. Physical therapy for spinal stenosis has been shown to produce outcomes comparable to surgery, with significantly less risk and recovery time. At Trinity Rehab, our licensed physical therapists across 27 locations in New Jersey and Pennsylvania specialize in helping patients regain mobility and return to what matters most — without surgical intervention.
What Is Spinal Stenosis?
Spinal stenosis occurs when the spinal canal — the hollow channel that houses the spinal cord and nerve roots — gradually narrows, compressing the delicate neural structures inside. The condition most commonly develops in two areas: the lumbar spine (lower back), which accounts for roughly 75 percent of cases, and the cervical spine (neck). The narrowing itself does not happen overnight. It is usually the cumulative result of age-related changes to the spine’s anatomy. As we get older, the intervertebral discs lose hydration and height, the facet joints thicken with arthritis, and the ligamentum flavum — a thick band of connective tissue running along the back of the spinal canal — can buckle inward. Each of these changes individually may not cause problems, but together they gradually reduce the available space for the spinal cord and nerve roots. There are two primary types of spinal stenosis: Lumbar spinal stenosis affects the lower back and is the more common form. Symptoms typically include pain, numbness, or weakness in the legs and buttocks that worsens with standing and walking (a pattern called neurogenic claudication) and improves when sitting or leaning forward. Cervical spinal stenosis affects the neck region and can produce more serious symptoms including difficulty with balance and coordination, hand weakness, and in severe cases, changes in bladder or bowel function that require immediate medical attention.
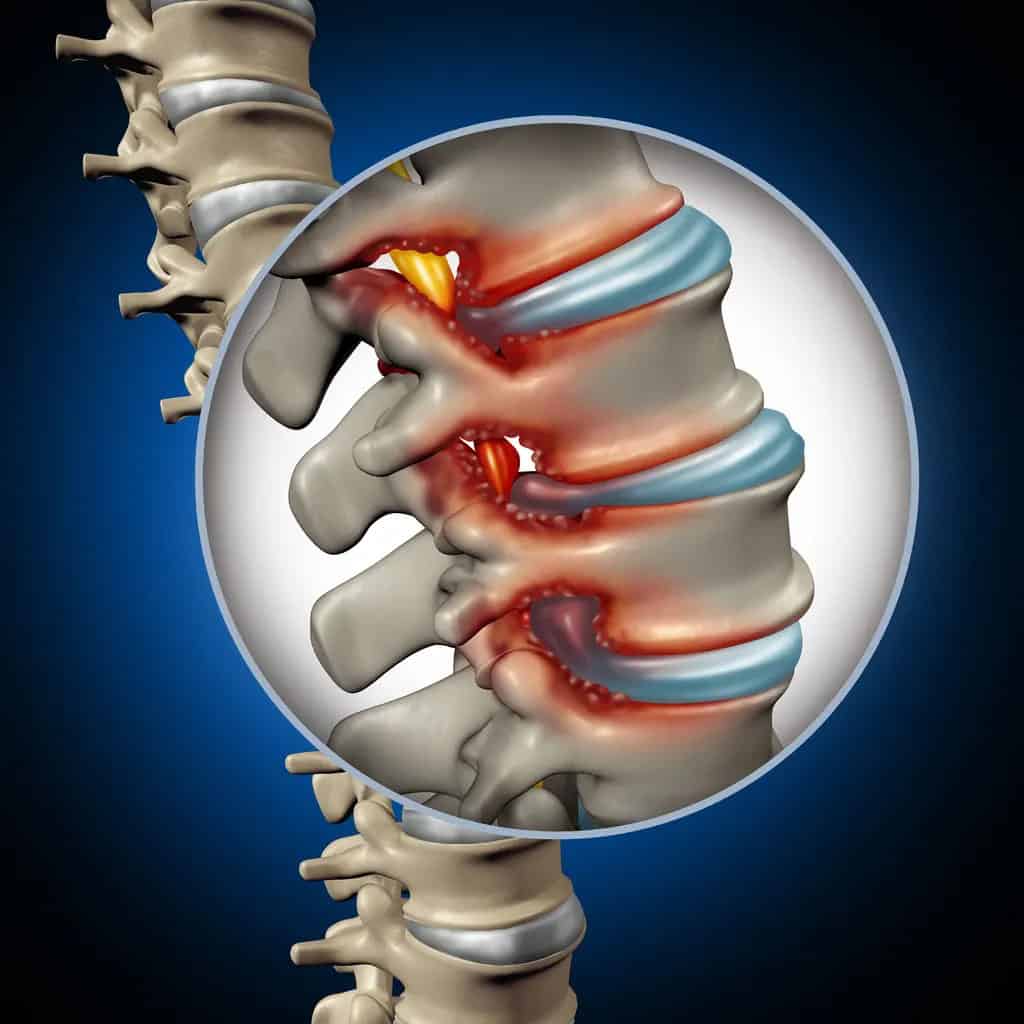
Why Spinal Stenosis Treatment Matters
Left unaddressed, spinal stenosis tends to follow a predictable pattern. The walking distances that trigger symptoms gradually shorten. Activities you once enjoyed — gardening, playing with grandchildren, taking the dog out — become sources of anxiety rather than pleasure. The natural response is to move less, but reduced activity accelerates the cycle: muscles weaken, joints stiffen, balance deteriorates, and the risk of falls increases. Research published in the *Journal of Orthopaedic & Sports Physical Therapy* demonstrates that patients who engage in structured physical therapy programs experience meaningful improvements in walking capacity, pain levels, and overall function — results that, for many patients with mild to moderate stenosis, match or exceed the outcomes of surgical decompression at two-year follow-up. The key is intervening early, before the deconditioning cycle takes hold.
Common Causes and Risk Factors
Understanding what contributes to spinal stenosis helps patients take an active role in managing their condition. The most common causes include:
- Degenerative changes: The single largest contributor. Cumulative wear on spinal structures — disc degeneration, facet joint arthritis, and ligament thickening — accounts for the vast majority of cases, especially in adults over 50.
- Herniated or bulging discs: When a disc pushes outward into the spinal canal, it compresses nearby nerve roots and can cause or worsen stenosis symptoms.
- Bone spurs (osteophytes): Osteoarthritis and chronic spinal stress stimulate extra bone growth along the vertebral edges, narrowing the space available for nerves.
- Thickened ligaments: The ligamentum flavum can stiffen and buckle inward over time, reducing canal space — a common finding in lumbar stenosis.
- Previous spinal injury or surgery: Vertebral fractures can cause immediate narrowing, and prior surgeries can lead to scar tissue or adjacent-level degeneration.
- Genetic factors: Some people are born with a naturally narrower spinal canal, meaning even minor degenerative changes produce symptoms earlier.
- Occupations and activities: Repetitive heavy lifting, prolonged standing, or sustained spinal loading can accelerate the degenerative process.
Symptoms Patients Often Notice
Spinal stenosis symptoms develop gradually, and many patients initially attribute them to "just getting older." Recognizing these patterns early can make a significant difference in treatment outcomes:
- Neurogenic claudication — aching, cramping, or heaviness in the legs and buttocks that worsens with walking or standing and improves with sitting or bending forward. This is the hallmark symptom of lumbar stenosis and distinguishes it from vascular claudication.
- Radiating pain — pain that travels from the lower back into one or both legs, sometimes reaching the feet. The pattern often follows a specific nerve root distribution.
- Numbness or tingling — decreased sensation in the legs, feet, or (in cervical stenosis) the hands and arms.
- Weakness — difficulty lifting the front of the foot (foot drop), trouble climbing stairs, or a feeling that the legs may give way.
- Balance problems — particularly with cervical stenosis, patients may notice increasing unsteadiness or difficulty with coordination.
- The "shopping cart sign" — patients find relief by leaning forward on a shopping cart, bicycle handlebars, or walker because forward flexion opens the spinal canal and reduces nerve compression.
- Difficulty with prolonged standing — standing in line, cooking at the counter, or watching a grandchild’s game becomes increasingly uncomfortable.

How Physical Therapy Treats Spinal Stenosis
At Trinity Rehab, our approach to spinal stenosis treatment is grounded in current evidence and tailored to each patient’s specific presentation, goals, and functional limitations. Physical therapy for spinal stenosis works by addressing the mechanical and muscular factors that influence nerve compression — factors that can be modified without surgery.
Phase 1: Comprehensive Evaluation and Pain Management
Your first visit begins with a thorough assessment of your spinal mobility, nerve function, strength, balance, and walking patterns. Your therapist will identify which movements and positions provoke or relieve your symptoms — information that directly shapes your treatment plan. Initial treatment focuses on reducing pain and inflammation through:
- Manual therapy — skilled hands-on techniques including spinal mobilization, soft tissue release, and neural mobilization to reduce pressure on compressed nerves and restore segmental mobility.
- Flexion-based positioning — because spinal stenosis symptoms improve with forward bending, your therapist may use specific positioning strategies (such as the Williams flexion exercises) to open the spinal canal and reduce nerve compression.
- Dry needling — targeted insertion of thin filament needles into myofascial trigger points in the paraspinal muscles, glutes, and hip musculature to release guarding and reduce referred pain patterns.
- Modalities as needed — heat, electrical stimulation, or ultrasound may be used adjunctively to manage acute pain episodes, though active treatment is always the foundation.
Phase 2: Core Stabilization and Strengthening
As pain decreases, the focus shifts to building the muscular support system your spine needs. Research consistently shows that strengthening the deep stabilizing muscles — the multifidus, transversus abdominis, and pelvic floor — significantly improves outcomes for stenosis patients. Your program will include:
- Core stabilization exercises — progressive training of the deep spinal stabilizers, beginning with isolated activation and advancing to functional integration.
- Hip and gluteal strengthening — the hip muscles play a critical role in controlling pelvic alignment and reducing compensatory stress on the lumbar spine. Weakness in the gluteus medius and hip external rotators is common in stenosis patients.
- Aquatic therapy — the buoyancy of water reduces spinal loading by up to 50 percent, allowing patients to exercise with less pain. Water-based programs have shown particular benefit for patients with stenosis who cannot tolerate land-based exercise initially.
- Flexibility training — targeted stretching of the hip flexors, hamstrings, and piriformis to address muscular tightness patterns that commonly accompany stenosis.

Phase 3: Functional Restoration and Endurance
The ultimate goal is not just pain reduction — it is returning you to the activities and roles that define your quality of life. This phase focuses on:
- Walking endurance training — systematic, progressive increases in walking distance and duration, monitored for symptom response. Many patients who initially could walk only one or two blocks progress to walking a mile or more.
- Balance and fall prevention — given that stenosis patients face an elevated fall risk, we incorporate balance training using varying surfaces, dual-task challenges, and reactive balance strategies.
- Activity-specific training — whether your goal is returning to golf, gardening, traveling, or simply keeping up with your grandchildren, your therapist designs exercises that replicate the demands of those activities.
- EPAT (shockwave therapy) — for patients with concurrent tendinopathy or chronic soft tissue involvement, Extracorporeal Pulse Activation Technology can accelerate tissue healing and reduce persistent pain.
How to Prevent Spinal Stenosis from Progressing
While some degree of spinal degeneration is inevitable with age, there is strong evidence that certain habits can slow the progression of stenosis and reduce symptom severity:
- Stay active — regular movement, particularly walking, swimming, and cycling, maintains spinal flexibility and muscular support. The worst thing for stenosis is prolonged inactivity.
- Maintain a healthy weight — every excess pound adds approximately four pounds of compressive force to the lumbar spine. Weight management directly reduces spinal loading.
- Practice good posture — avoiding prolonged extension (standing with an exaggerated arch) and learning to maintain a neutral spine during daily activities reduces canal narrowing.
- Strengthen your core consistently — the deep stabilizing muscles act as a natural brace for the spine. A structured home exercise program, maintained after formal PT concludes, is one of the strongest predictors of long-term success.
- Modify high-risk activities — learning proper body mechanics for lifting, bending, and carrying can reduce the repetitive stress that accelerates degeneration.
- Don’t ignore early symptoms — the earlier you address stenosis symptoms with physical therapy, the better the outcomes. Waiting until symptoms are severe limits treatment options.
Why Patients Choose Trinity Rehab for Spinal Stenosis Treatment
Trinity Rehab’s approach to spinal stenosis is built on the principles that matter most to our patients:
- Individualized, one-on-one care. Every session is with your dedicated physical therapist — not passed between aides or assistants. Your therapist knows your history and adjusts your program based on how you respond.
- Evidence-based treatment protocols. Our clinical team stays current with the latest spinal stenosis research, including the SPORT trial and current JOSPT clinical practice guidelines.
- Convenient access across NJ and PA. With 27 locations, most patients are seen within 24–48 hours. We accept most major insurance plans including Medicare.
- A track record with spinal conditions. Back pain, sciatica, herniated discs, and stenosis are among our most commonly treated conditions. Our therapists understand the nuances of spinal rehabilitation.
Getting Back to What Matters
Spinal stenosis does not have to define how you move through life. The tightness in your legs, the shortened walks, the activities you have quietly given up — these are symptoms of a treatable condition, not an inevitable part of aging. At Trinity Rehab, we have helped thousands of patients across New Jersey and Pennsylvania reclaim the mobility and confidence that stenosis tried to take away. Our one-on-one approach means your treatment is never generic — it is built around your body, your goals, and your life.
Your Next Steps
Getting started is simple: 1. Call or request an appointment online at any of our 27 locations across New Jersey and Pennsylvania. 2. Complete your evaluation — most patients are seen within 24-48 hours. 3. Begin your personalized treatment plan — designed by your dedicated physical therapist to address your specific stenosis symptoms and goals. You do not need to keep adjusting your life around spinal stenosis. Let us help you move forward — comfortably, confidently, and on your own terms.
Find Spinal Stenosis Treatment Near You
New Jersey
- Spinal Stenosis Treatment in Brick, NJ
- Spinal Stenosis Treatment in Cherry Hill, NJ
- Spinal Stenosis Treatment in Clark, NJ
- Spinal Stenosis Treatment in Clifton, NJ
- Spinal Stenosis Treatment in East Brunswick, NJ
- Spinal Stenosis Treatment in East Windsor, NJ
- Spinal Stenosis Treatment in Emerson, NJ
- Spinal Stenosis Treatment in Flemington, NJ
- Spinal Stenosis Treatment in Hamilton, NJ
- Spinal Stenosis Treatment in Howell, NJ
- Spinal Stenosis Treatment in Manalapan, NJ
- Spinal Stenosis Treatment in Matawan, NJ
- Spinal Stenosis Treatment in Metuchen, NJ
- Spinal Stenosis Treatment in Middletown, NJ
- Spinal Stenosis Treatment in Piscataway, NJ
- Spinal Stenosis Treatment in Sewell, NJ
- Spinal Stenosis Treatment in Shrewsbury, NJ
- Spinal Stenosis Treatment in Somerset, NJ
- Spinal Stenosis Treatment in Somerville, NJ
- Spinal Stenosis Treatment in Sparta, NJ
- Spinal Stenosis Treatment in Toms River, NJ
- Spinal Stenosis Treatment in Warren, NJ
- Spinal Stenosis Treatment in Wayne, NJ
- Spinal Stenosis Treatment in Woodbridge, NJ
Pennsylvania
- Spinal Stenosis Treatment in Doylestown, PA
- Spinal Stenosis Treatment in Newtown, PA
- Spinal Stenosis Treatment in Upper Dublin, PA
Sources
1. National Institute of Arthritis and Musculoskeletal and Skin Diseases. "Spinal Stenosis." National Institutes of Health. https://www.niams.nih.gov/health-topics/spinal-stenosis 2. Delitto A, et al. "Surgery versus nonsurgical treatment of lumbar spinal stenosis (SPORT): a randomized trial." *Spine*. 2015;40(18):1471-1482.
What is the best treatment for spinal stenosis?
Can physical therapy make spinal stenosis worse?
What exercises should I avoid with spinal stenosis?
How long does physical therapy for spinal stenosis take?
Is walking good for spinal stenosis?
Can spinal stenosis be cured without surgery?
What is the difference between spinal stenosis and sciatica?
Does Medicare cover physical therapy for spinal stenosis?
Find Treatment Near You
- Spinal Stenosis Treatment in Brick, NJ
- Spinal Stenosis Treatment in Cherry, NJ
- Spinal Stenosis Treatment in Clark, NJ
- Spinal Stenosis Treatment in Clifton, NJ
- Spinal Stenosis Treatment in Doylestown, PA
- Spinal Stenosis Treatment in Upper Dublin, PA
- Spinal Stenosis Treatment in East, NJ
- Spinal Stenosis Treatment in East, NJ
- Spinal Stenosis Treatment in Emerson, NJ
- Spinal Stenosis Treatment in Flemington, NJ
- Spinal Stenosis Treatment in Hamilton, NJ
- Spinal Stenosis Treatment in Howell, NJ
- Spinal Stenosis Treatment in Manalapan, NJ
- Spinal Stenosis Treatment in Matawan, NJ
- Spinal Stenosis Treatment in Metuchen, NJ
- Spinal Stenosis Treatment in Middletown, NJ
- Spinal Stenosis Treatment in Newtown, PA
- Spinal Stenosis Treatment in Piscataway, NJ
- Spinal Stenosis Treatment in Sewell, NJ
- Spinal Stenosis Treatment in Shrewsbury, NJ
- Spinal Stenosis Treatment in Somerset, NJ
- Spinal Stenosis Treatment in Somerville, NJ
- Spinal Stenosis Treatment in Sparta, NJ
- Spinal Stenosis Treatment in Toms, NJ
- Spinal Stenosis Treatment in Warren, NJ
- Spinal Stenosis Treatment in Wayne, NJ
- Spinal Stenosis Treatment in Woodbridge, NJ
