Spinal Stenosis Treatment in Piscataway, NJ
Piscataway is a vibrant, diverse community with unique opportunities — home to Rutgers University, Johnson Park’s expansive green spaces, and a neighborhood culture that values education, recreation, and community involvement. Whether you’re a Rutgers family member, local resident, or part of Piscataway’s active population, there’s always something happening. But when spinal stenosis develops, that active community life becomes increasingly difficult. Walks through Johnson Park, once a weekend staple, now trigger leg pain and heaviness. Attending Rutgers events or local functions means standing through discomfort. The spontaneity of getting out and enjoying your community fades away. If you recognize this pattern — pain and heaviness in your legs that worsens with standing and walking but mysteriously eases when you sit — you may have spinal stenosis, a progressive narrowing of the spinal canal affecting an estimated 11 percent of adults and responsible for more spinal surgeries in seniors than any other condition. The encouraging news: physical therapy has been shown to produce outcomes matching surgical outcomes for many patients, with significantly less risk and no recovery time required. At Trinity Rehab Piscataway, our licensed physical therapists specialize in helping Middlesex County residents, especially the diverse Piscataway community, reclaim their mobility and return to the activities that keep them connected to their neighborhood and Rutgers family — without surgical intervention.
Understanding Spinal Stenosis and Its Impact on Active Living
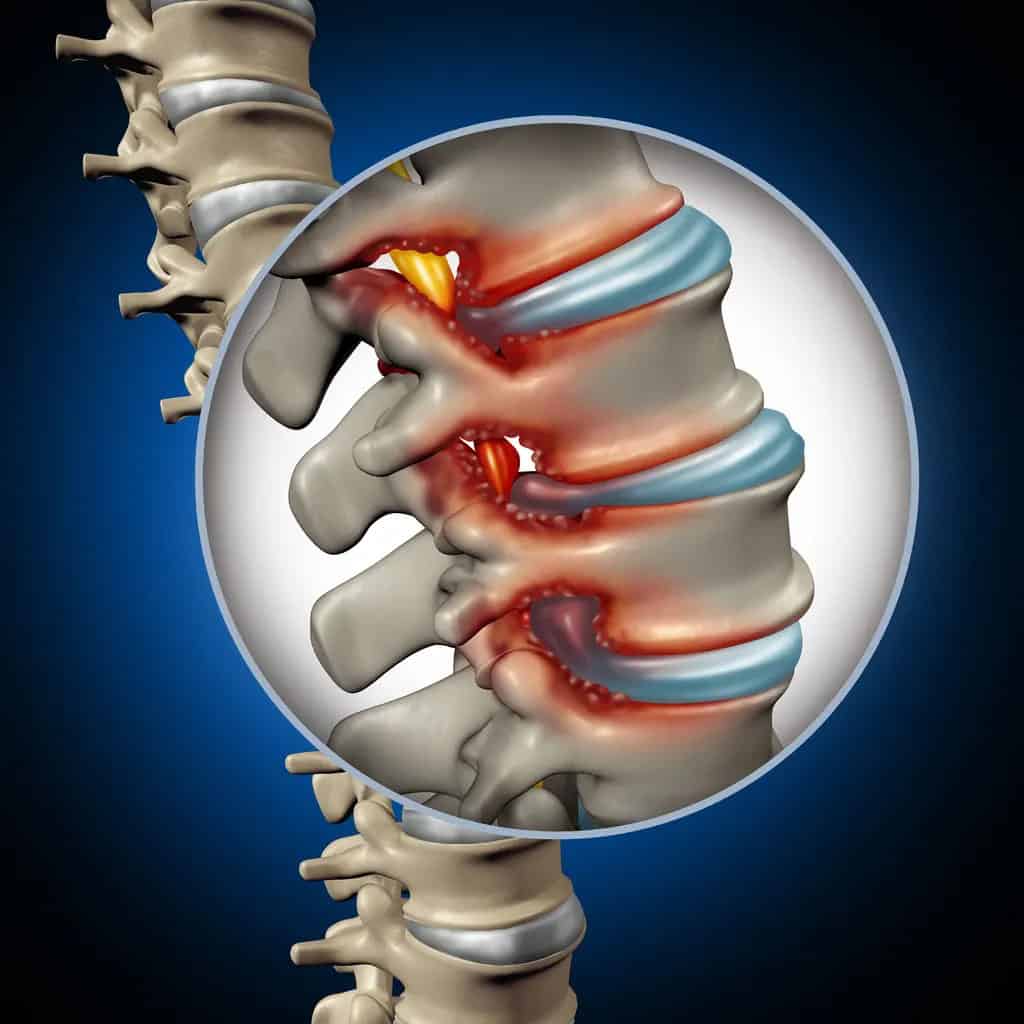
Spinal stenosis occurs when the spinal canal — the channel housing your spinal cord and nerve roots — gradually narrows, compressing the delicate neural structures inside. The narrowing usually develops in the lumbar spine (lower back), accounting for roughly 75 percent of cases. The process unfolds through cumulative age-related changes: intervertebral discs lose hydration and height, facet joints thicken with arthritis, and the ligamentum flavum — a thick band of connective tissue behind the spinal canal — buckles inward. Each change is gradual, but together they progressively reduce the space available for your spinal cord and nerve roots. For Piscataway residents who value community involvement and an active lifestyle, understanding this progression is important because it means stenosis is progressive but manageable — intervening early with physical therapy can slow progression and often prevent the need for surgery.
Risk Factors Specific to Piscataway and Middlesex County Living
Several factors increase stenosis risk, and many are particularly relevant to Piscataway residents: Urban and suburban lifestyle demands: Piscataway’s diverse character — Rutgers university activities, Johnson Park recreation, urban and suburban living patterns — creates varied physical demands. Over decades, these accumulated demands on the spine, especially without adequate core strength, can accelerate degenerative changes. Diverse occupational patterns: Piscataway’s workforce is diverse, with residents working in education, technology, healthcare, manufacturing, and service industries. Many of these occupations involve sustained sitting, repetitive motions, or physical demands that accelerate spinal degeneration. Degenerative changes: The cumulative wear on spinal structures over decades — disc degeneration, facet joint arthritis, and ligament thickening — accounts for the vast majority of stenosis cases, particularly in adults over 50. Herniated or bulging discs: When an intervertebral disc protrudes into the spinal canal, it compresses nearby nerve roots and can cause or worsen stenosis. Bone spurs (osteophytes): Osteoarthritis and chronic spinal stress stimulate extra bone growth, which can extend into the spinal canal. Thickened ligaments: The ligamentum flavum can thicken over time. When it buckles inward, it reduces canal space. Previous spinal injury or surgery: Trauma to the spine can cause immediate narrowing. Prior spinal surgeries can sometimes lead to adjacent-level degeneration. Genetic factors: Some people are born with a naturally narrower spinal canal, meaning even minor degenerative changes produce symptoms earlier in life.
Symptoms That Disrupt Your Piscataway Routine
Spinal stenosis symptoms develop gradually, and many people initially attribute them to busy schedules or aging. Early recognition makes a significant difference in treatment outcomes:
- Neurogenic claudication — aching, cramping, or heaviness in the legs and buttocks that worsens with walking or standing and improves when you sit or lean forward. This is the hallmark symptom.
- Radiating pain — pain traveling from your lower back into one or both legs, sometimes reaching your feet.
- Numbness or tingling — decreased sensation in the legs and feet, particularly noticeable during community activities or park walks.
- Weakness — difficulty lifting the front of your foot, trouble climbing stairs, or a feeling that your legs may give way.
- Balance problems — increasing unsteadiness or difficulty with coordination.
- The "shopping cart sign" — finding relief by leaning forward on a walker or cane because forward flexion opens the spinal canal and reduces compression.
- Difficulty with prolonged standing — standing through Rutgers events, community gatherings, or Johnson Park activities becomes increasingly uncomfortable.
How Trinity Rehab Piscataway Treats Spinal Stenosis
Trinity Rehab’s approach to spinal stenosis treatment is grounded in current evidence and individualized to each patient’s specific presentation, goals, and functional limitations. Physical therapy works by addressing the mechanical and muscular factors influencing nerve compression — factors that can be modified without surgery.
Phase 1: Comprehensive Evaluation and Pain Management
Your first visit begins with a thorough assessment of spinal mobility, nerve function, strength, balance, and walking patterns. Your therapist identifies which movements and positions provoke or relieve your symptoms — information that directly shapes your treatment plan. Initial treatment focuses on reducing pain and inflammation through:
- Manual therapy — skilled hands-on techniques including spinal mobilization, soft tissue release, and neural mobilization to reduce pressure on compressed nerves.
- Flexion-based positioning — using specific positioning strategies to open the spinal canal and reduce nerve compression.
- Dry needling — targeted insertion of thin filament needles into myofascial trigger points in paraspinal muscles, glutes, and hip musculature to release guarding.
- Modalities as needed — heat, electrical stimulation, or ultrasound may be used adjunctively to manage acute pain episodes.
Phase 2: Core Stabilization and Strengthening
As pain decreases, focus shifts to building the muscular support system your spine needs. Research consistently shows that strengthening deep stabilizing muscles — the multifidus, transversus abdominis, and pelvic floor — significantly improves outcomes. Your program will include:
- Core stabilization exercises — progressive training of deep spinal stabilizers.
- Hip and gluteal strengthening — hip muscles play a critical role in controlling pelvic alignment and reducing compensatory stress on the lumbar spine.
- Aquatic therapy — water’s buoyancy reduces spinal loading by up to 50 percent, allowing exercise with significantly less pain.
- Flexibility training — targeted stretching of hip flexors, hamstrings, and piriformis.
Phase 3: Functional Restoration and Endurance
The ultimate goal is returning you to activities defining your quality of life:
- Walking endurance training — systematic, progressive increases in walking distance and duration, monitored for symptom response. Many patients progress from short walks to comfortable community outings.
- Balance and fall prevention — stenosis patients face elevated fall risk. Balance training uses varying surfaces and reactive strategies.
- Activity-specific training — whether your goal is Johnson Park walks, Rutgers events, or other community involvement, your therapist designs exercises replicating those demands.
- EPAT (shockwave therapy) — for patients with concurrent tendinopathy, Extracorporeal Pulse Activation Technology can accelerate tissue healing.
Preventing Spinal Stenosis Progression While Living in Piscataway
While some spinal degeneration is inevitable with age, strong evidence shows certain habits slow stenosis progression and reduce symptom severity:
- Stay active — regular movement, particularly walking through Johnson Park, swimming, and cycling maintains spinal flexibility and muscular support. The worst thing for stenosis is prolonged inactivity.
- Maintain healthy weight — every excess pound adds approximately four pounds of compressive force to the lumbar spine.
- Practice good posture — avoiding prolonged extension and maintaining neutral spine during daily activities, whether at work or in the community, reduces canal narrowing.
- Strengthen core consistently — deep stabilizing muscles act as a natural brace. A home exercise program maintained after formal PT is crucial for long-term success.
- Modify high-risk activities — learning proper body mechanics for daily activities reduces repetitive stress.
- Address symptoms early — the earlier you address stenosis symptoms with physical therapy, the better your outcomes.
Why Piscataway Residents Choose Trinity Rehab for Spinal Stenosis
Trinity Rehab Piscataway’s approach is built on three principles that matter most to our Middlesex County patients: Individualized, one-on-one care. Every session is spent with your dedicated physical therapist — not passed between aides or assistants. Your therapist knows your history, understands your community involvement goals, and adjusts your program based on your response. Evidence-based treatment protocols. Our clinical team stays current with the latest spinal stenosis research, including landmark SPORT trial findings and current clinical practice guidelines. Your treatment reflects what the evidence shows works. Convenient access to care. Located right in Piscataway, Trinity Rehab is where you live and work. Most patients are seen within 24-48 hours of calling, and we accept most major insurance plans including Medicare.
Getting Back to Your Piscataway Life
Spinal stenosis does not have to define how you move through life. The tightness in your legs, the shortened walks, the Johnson Park strolls and community activities you have quietly given up — these are symptoms of a treatable condition, not an inevitable part of aging. At Trinity Rehab Piscataway, we have helped hundreds of Middlesex County residents reclaim the mobility and confidence that stenosis tried to take away. Our one-on-one approach means your treatment is never generic — it is built around your body, your goals, and your Piscataway community life.
Your Next Steps
Getting started is simple: 1. Call Trinity Rehab Piscataway or request an appointment online. 2. Complete your evaluation — most patients are seen within 24-48 hours. 3. Begin your personalized treatment plan — designed by your dedicated physical therapist to address your specific stenosis symptoms and goals. You do not need to keep adjusting your life around spinal stenosis. Let us help you move forward — comfortably, confidently, and on your own terms in Piscataway.
Local Spinal Stenosis Care in Piscataway, NJ
For patients in Piscataway and nearby communities such as Edison, South Plainfield, Dunellen, New Brunswick, spinal stenosis care has to fit real routines: campus-style walking, standing work, commuting, and recreational activity. Your therapist will connect your symptoms to the daily demands that matter most, including walking tolerance, balance, stairs, and reducing leg symptoms during long days.
Your first visit at Trinity Rehab Piscataway includes a review of your symptoms, walking tolerance, posture, balance, hip and core strength, and the positions that ease or worsen leg symptoms. The clinic is located at 1354 Centennial Ave Unit A3-B, Piscataway, NJ, 08854.
Call (732) 712-2170 for the Piscataway clinic, or use the clinic page for current hours and appointment details.
For directions, parking context, and the best route to the clinic, use Google Maps for Trinity Rehab Piscataway.
Spinal stenosis often overlaps with back pain, sciatica, degenerative disc disease, and lumbar disc herniation. Your plan may include mobility work, flexion-biased exercise when appropriate, balance training, core and hip strengthening, walking progression, and education on safer ways to pace activity.
Can I return to walking and community activities?
What should I avoid?
Is physical therapy as effective as surgery?
How long does treatment take?
Will my condition get worse without treatment?
Does Medicare cover PT for spinal stenosis?
Related Spine Care At This Location
Spinal stenosis symptoms may overlap with other spine and disc-related problems. Your therapist may also review:




