PLANTAR FASCIITIS TREATMENT IN WARREN, NJ
Warren Township is the kind of place where people stay active. The trails through East County Park draw morning runners and weekend hikers year-round. The Warren Health & Racquet Club courts are booked most evenings. Warrenbrook Golf Course fills up on Saturday mornings. And across the township’s neighborhoods and corporate corridors, plenty of people spend their days on their feet — commuting, coaching, working long hours at desks between periods of concentrated walking.
Plantar fasciitis threads through all of it. It’s the heel pain that announces itself the moment you step out of bed, eases reluctantly over the first ten minutes of walking, and returns hours later after you’ve been sitting in a conference room or on a drive down I-78. Over time, it starts affecting your choices — whether to lace up for the Warren Trails or stay home, whether to sign up for the 5K or skip another year.
You don’t have to manage around it indefinitely. Trinity Rehab’s physical therapists help Warren patients find the root cause of their plantar fasciitis and resolve it with a treatment approach that actually addresses the mechanics, not just the symptoms.

UNDERSTANDING PLANTAR FASCIITIS
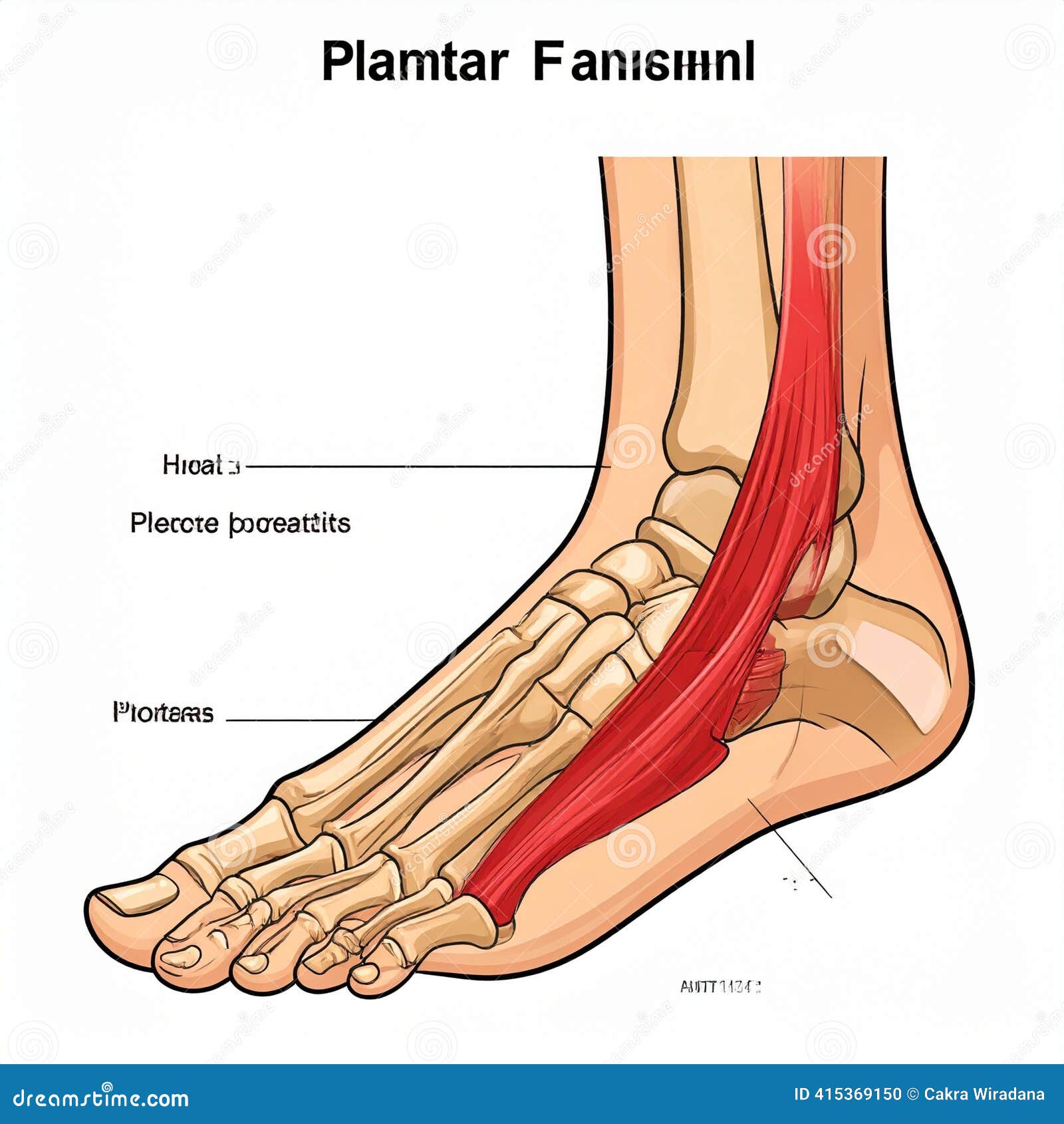
The plantar fascia is a thick band of connective tissue stretching the length of your foot’s underside — from the heel bone to the ball of the foot. Think of it as a structural cable that simultaneously supports your arch, cushions the shock of impact, and enables the spring-like energy transfer your foot uses during walking and running.
Plantar fasciitis develops when the load placed on that tissue consistently exceeds what it can repair between uses. Micro-tears accumulate at the calcaneal attachment (the point where the fascia meets the heel bone), triggering an inflammatory response that the body never quite resolves under continued loading. The tissue thickens and degenerates — a state clinicians sometimes describe as plantar fasciopathy — and the result is pain that becomes increasingly disruptive over weeks and months.
The American Academy of Orthopaedic Surgeons reports that about 2 million patients receive plantar fasciitis treatment annually in the United States. The condition disproportionately affects adults aged 40 to 60, a demographic well-represented in Warren’s affluent, active population. Research consistently shows that physical therapy — particularly when begun before symptoms become chronic — resolves the vast majority of cases without surgical intervention.
RELATED CONDITIONS & TREATMENTS
Plantar fasciitis is just one of the many conditions we treat at Trinity Rehab Warren. Explore our full range of conditions we treat or learn more about specific treatment approaches:
WHY WARREN RESIDENTS DEVELOP PLANTAR FASCIITIS
Warren’s particular mix of lifestyle and occupation creates several distinct risk patterns.
Trail runners and hikers who use East County Park’s nature trails and the broader Warren Trails network do exactly the kind of repetitive-impact, varied-surface activity that loads the plantar fascia most heavily. The rolling terrain between the Watchung Mountain ridges means every stride involves slight elevation changes that recruit the foot in different ways — building fitness, but also accumulating micro-stress with each outing. When training volume increases too quickly heading into race season, or when athletes transition from winter inactivity to spring running without adequate ramp-up time, plantar fasciitis is a predictable consequence.
Corporate office workers at the professional services firms clustered in and around Warren — and at the pharmaceutical and biotech companies along the Route 22 corridor — often present with a different pattern. Extended sitting at a desk stiffens the calf-Achilles-fascia chain, and the combination of tight structures plus an abrupt transition to significant walking (a long meeting, a commute on foot, or a lunchtime walk) creates the kind of loading mismatch that the plantar fascia doesn’t handle well.
Tennis and pickleball players at the Warren Health & Racquet Club make the kind of lateral moves, quick stops, and explosive pushoffs that place sharp, repetitive demands on the plantar fascia. The hard court surface amplifies every impact force. Court athletes who play frequently without adequate calf flexibility or foot strength conditioning are at elevated risk.
Golfers at Warrenbrook Golf Course walk 18 holes at a time — often five to seven miles — on gently sloped terrain in footwear that typically prioritizes traction over cushioning. The repetitive loading on the same tissue, over hours on slightly uneven ground, is a well-established plantar fasciitis risk factor.
Watchung Hills Regional High School Warriors — across football, wrestling, track and field, and lacrosse — face the overuse patterns inherent to year-round athletic competition. Wrestlers and track athletes especially accumulate significant lower limb stress through their seasons, and plantar fasciitis often develops at the edges of competitive training blocks.
THE SYMPTOM PATTERN
Plantar fasciitis has a recognizable signature. If you’ve been living with it, these details will likely feel familiar:
The defining feature is sharp, stabbing heel pain with the first steps of the morning. The fascia stiffens and shortens overnight; the sudden load of weight-bearing creates an intense stretch at the calcaneal attachment that many patients describe as the worst moment of their day. After ten to fifteen minutes of movement, the tissue warms and the acute pain subsides — only to return after the next period of rest.
Pain after sitting mirrors the morning pattern. A long client meeting, a drive down Route 78, a two-hour stretch at the desk — any of these can trigger the same stiffening cycle. The first steps out of the chair or out of the car are reliably the worst.
Other characteristic signs:
- Point tenderness directly under the heel, toward the inner side
- Arch stiffness that persists through morning even after the acute heel pain eases
- Aching that worsens after — not during — a run or long walk
- Slight limping or favoring of one foot, which you may not notice consciously but your family does
A Warren resident who competes in a local corporate tennis league described the progression: “I’d play fine, feel okay for a few hours, then by evening my heel was burning. The next morning was miserable. I started parking closer, taking the elevator — basically organizing my day around my heel.” That combination of post-activity soreness and morning stiffness is classic plantar fasciitis, and it responds well to the right treatment.
HOW PHYSICAL THERAPY RESTORES FUNCTION
MANUAL THERAPY AND TISSUE MOBILIZATION
Manual therapy is the cornerstone of early plantar fasciitis treatment at Trinity Rehab. Restricted ankle dorsiflexion — often caused by tight calf muscles from running, tennis, or prolonged sitting — is one of the most consistent mechanical drivers of plantar fasciitis. When the ankle can’t move through its full range of motion, every step transfers excessive strain to the plantar fascia as compensation.
Subtalar and ankle joint mobilization restores this range of motion directly. Clinical research published in the Journal of Orthopaedic & Sports Physical Therapy demonstrates that joint mobilization combined with stretching produces significantly greater pain reduction and functional improvement than stretching alone.
Instrument-assisted soft tissue mobilization (IASTM) uses specialized tools to work through the adhesions and scar tissue that form in chronically irritated fascial tissue. This technique stimulates healthy tissue remodeling by creating a controlled microtrauma that recruits the body’s repair mechanisms.
Myofascial release and trigger point therapy address the knotted tissue in the gastrocnemius, soleus, and intrinsic foot muscles that maintains constant fascial tension. When these trigger points are released, the resting load on the plantar fascia drops significantly — often producing immediate pain relief.

TARGETED STRETCHING PROTOCOL
Your therapist will design a stretching program based on your specific mobility deficits:
Plantar fascia-specific stretching performed before the first step of the morning — dorsiflexing the toes and holding for 30 seconds — reduces morning pain by pre-loading the windlass mechanism before the fascia takes full body weight. This single intervention has strong clinical support for reducing the severity of first-step pain.
Calf stretching for gastrocnemius and soleus addresses the upstream tightness that drives so much of plantar fasciitis. Wall stretches targeting each muscle separately, step drops, and progressive stretching under load help restore the ankle dorsiflexion that protects the fascia.
PROGRESSIVE STRENGTHENING AND ADVANCED INTERVENTIONS
Eccentric calf raises — lowering the heel slowly off the edge of a step — build the load-tolerating capacity of the entire calf-Achilles-fascia unit. This is the most evidence-supported strengthening intervention for plantar fasciitis and a key reason why physical therapy produces better long-term outcomes than rest alone.
Intrinsic foot strengthening (towel scrunches, short-foot exercises, marble pickups) builds the internal arch support that reduces the load the plantar fascia must bear. Single-leg balance progressions restore the proprioceptive function that is often compromised when pain has altered your gait.
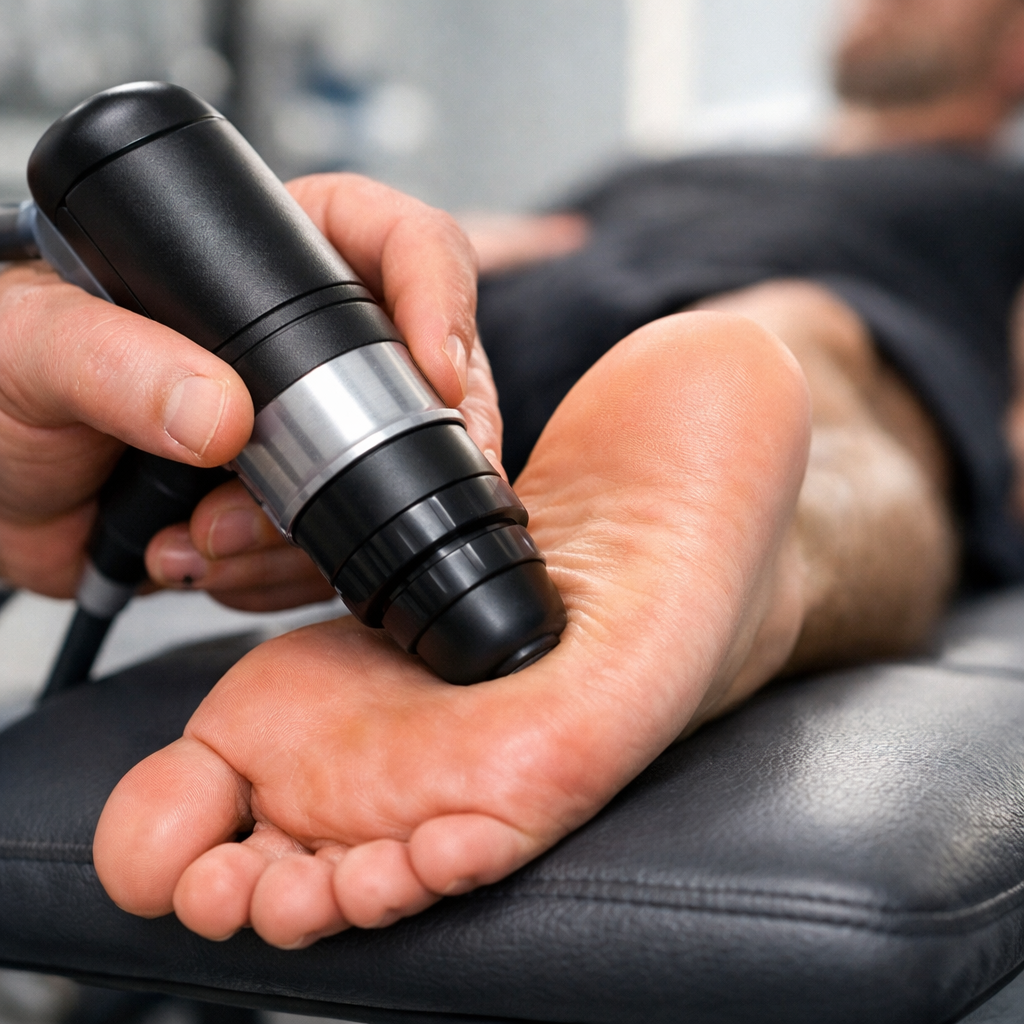
For Warren patients with persistent heel pain that has not responded to conventional treatment, Trinity Rehab offers EPAT shockwave therapy — acoustic pressure waves that stimulate blood flow and regeneration in damaged fascial tissue. The Mayo Clinic identifies EPAT as an effective option for chronic cases. Dry needling is available for patients with significant myofascial trigger points contributing to persistent pain.
RETURN TO YOUR SPORT
The final component of your treatment plan is a structured return-to-activity protocol calibrated to your specific goals. Getting back to the Warren Trails, the Warrenbrook fairways, or the Racquet Club courts requires a systematic, progressive loading strategy — not simply stopping as soon as pain eases and hoping it holds. Your Trinity Rehab therapist will guide every step of this transition.
STAYING AHEAD OF PLANTAR FASCIITIS
Recurrence is preventable with the right habits:
- Replace running shoes before they fail, not after. Track your mileage on the Warren Trails and retire athletic shoes at 300 to 500 miles — well before the uppers look worn.
- Warm up your calves before morning trail sessions. A brief calf stretch and plantar fascia mobilization before you step out the door dramatically reduces the abrupt first-load stress that initiates injury.
- Wear genuine support at the office. Long days in flat dress shoes or worn loafers are as hard on your plantar fascia as an overloaded run. Invest in dress footwear with arch support, particularly for days with heavy walking.
- Don’t add court time too quickly. When returning to tennis or pickleball after time off, ease back over two to three weeks rather than jumping straight into competitive play.
- Stretch after golf. Five to seven miles on slightly sloped ground stiffens the calf chain. A ten-minute post-round stretching routine prevents that tightness from accumulating into fascial stress.
WHY WARREN PATIENTS TRUST TRINITY REHAB
Every appointment at Trinity Rehab is a genuine one-on-one session with your licensed physical therapist. This isn’t a model where your initial evaluation is followed by sessions with assistants or aides — your therapist is with you throughout, adjusting your plan based on how your tissue is actually responding. In a condition like plantar fasciitis, where the pacing of progressive loading matters enormously, that continuity of expert attention makes a meaningful clinical difference.
We accept most major insurance plans and require no physician referral. Our therapists are deeply experienced with the full spectrum of foot and ankle conditions affecting active adults, and we understand the compensatory chain reaction that untreated plantar fasciitis can create — from altered gait to back pain and even sciatica. We address all of it.
Inside Our Warren Clinic


FREQUENTLY ASKED QUESTIONS
Where can I get plantar fasciitis treatment in Warren, NJ?
How is plantar fasciitis different from a heel spur?
Can I keep playing tennis or golf during treatment?
How long until I see improvement?
Will I need orthotics?
TAKE THE FIRST STEP TOWARD PAIN-FREE LIVING
The Warren Trails, the Warrenbrook fairways, the courts at the Racquet Club — all of it is still on the table. Plantar fasciitis is a real condition with real functional consequences, but it is also one that physical therapy resolves with a high success rate when treatment begins at the right time.
Trinity Rehab is ready to help. Request your appointment today — no referral required, most insurance accepted.
Sources: JOSPT Clinical Practice Guidelines for Heel Pain/Plantar Fasciitis, 2023 | Mayo Clinic — Plantar Fasciitis | American Academy of Orthopaedic Surgeons | APTA Clinical Practice Guidelines
What Our Patients Say




