Meniscus Tear Treatment in Hamilton, NJ — Trinity Rehab
Hamilton is a Mercer County community where diversity defines the character — a place where families from numerous backgrounds work in varied industries, raise children with different visions of success, and maintain health through different approaches to activity and fitness. Whether you’re involved in Hamilton West or Hamilton East athletics, enjoy Veterans Park for recreation and fitness, or maintain physical activity through your workplace and personal pursuits, a meniscus tear disrupts the rhythm of your life.
The injury might have happened during a recreational game at a neighborhood park, while navigating your physically demanding profession, or during a moment when your knee caught in a way that sent pain radiating through your joint. The immediate questions are both practical and emotional: Will I need surgery? How long until I can return to normal? The encouraging reality is that meniscus tears are highly treatable without surgery. Most Hamilton residents recover completely with targeted physical therapy and resume their activities within 8-12 weeks. Your recovery is achievable, predictable, and doesn’t require the disruption that surgery would bring.
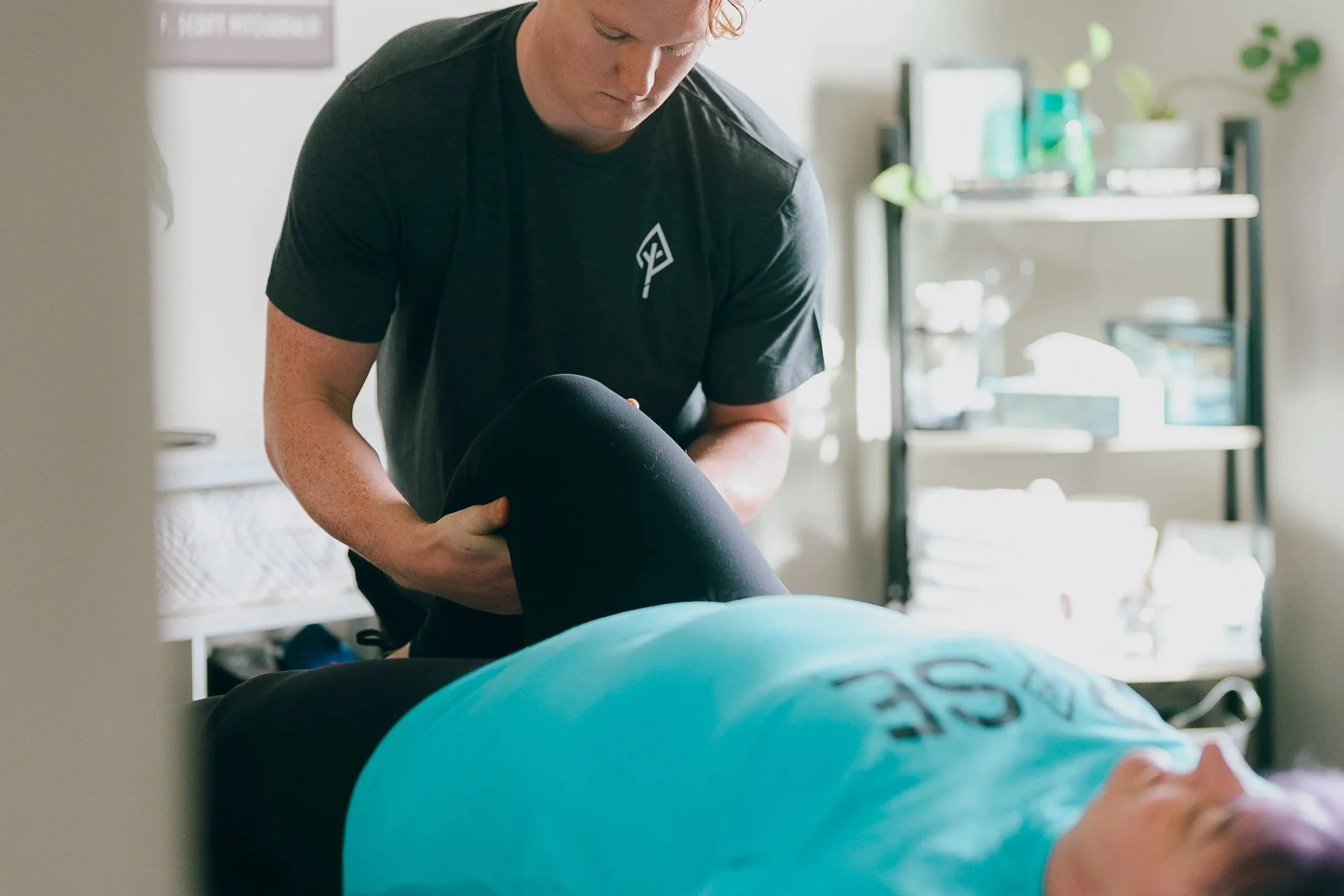
Understanding Your Meniscus and Its Critical Role
Your knee contains two menisci — crescent-shaped cartilage structures that perform three essential functions. They absorb shock (which is why impact-loading activities don’t immediately hurt), distribute weight evenly (which prevents cartilage wear and maintains joint longevity), and provide stability (which prevents your knee from shifting during movement). These small structures handle enormous forces throughout your day.
When a meniscus tears, these protective functions deteriorate. The knee becomes less stable, less cushioned, and more vulnerable to additional damage. Without treatment, this can progress to chronic pain and increased risk of developing osteoarthritis years later. The good news is that this cascade is entirely preventable. Research from the New England Journal of Medicine demonstrates that physical therapy produces outcomes comparable to surgery for most meniscus tears, particularly in adults. For athletes facing this injury, implementing effective meniscus tear recovery strategies for athletes is essential for a timely return to sport. This could include a combination of targeted physical therapy, strength training, and modified activity to allow for healing while maintaining fitness levels. Collaborating with a sports medicine specialist can further optimize rehabilitation approaches tailored to individual needs. meniscus tear diagnosis and treatment options can vary depending on the severity of the injury. In many cases, conservative approaches like physical therapy and rehabilitation exercises are effective in restoring knee function. However, for more severe tears, surgical intervention may be necessary to ensure proper healing and stability. In addition to physical therapy, meniscus tear treatment options available may include corticosteroid injections to reduce inflammation and promote healing. Some patients may also consider the option of arthroscopic surgery if conservative treatments do not yield sufficient relief. It’s essential to consult with a healthcare professional to determine the best approach tailored to individual needs and conditions. meniscus tear symptoms and diagnosis can vary greatly among individuals. Common symptoms include swelling, pain during movement, and difficulty straightening the knee. Early diagnosis is crucial, as it allows for timely intervention and decreases the likelihood of long-term consequences. Incorporating meniscus tear rehabilitation exercises into a recovery plan can significantly enhance the healing process. These exercises focus on strengthening the muscles around the knee, improving stability and flexibility, which are critical for preventing further injury. Additionally, a tailored rehabilitation program can help patients regain full function and return to their normal activities more swiftly.
Why Hamilton’s Diverse Population Experiences Meniscus Tears
Hamilton’s character creates multiple pathways to meniscus injuries:
- Athletic programs — Hamilton West and Hamilton East athletics involve plant-and-cut movements, jumping, and directional changes that create acute meniscus tears during competition or practice
- Workplace demands — Many Hamilton residents work in physically demanding professions (manufacturing, healthcare, construction, maintenance) requiring repetitive kneeling, squatting, or heavy lifting. These activities create overuse stress and acute injury risk
- Multi-generational sports participation — Parents staying active alongside sports-participating children, family recreational activities, and intergenerational involvement create diverse injury patterns
- Recreation at Veterans Park — The community park hosts walking, running, recreational sports, and family activities that can precipitate injuries
- Commuter fitness — Professionals balancing demanding work schedules with fitness maintenance sometimes sustain injuries through rushed or fatigued exercise
- Age-related degenerative changes — Hamilton’s older population develops meniscus tears from progressive cartilage weakening, where routine activities (stepping, squatting) can cause tears in compromised tissue
How You’ll Know You’ve Torn Your Meniscus
The injury usually announces itself with clear signs:
- A pop, snap, or tearing sensation at the moment of injury
- Swelling that develops within 30 minutes to 2 hours, or gradually over 24 hours
- Sharp, well-localized pain on the inner or outer edge of your knee
- Difficulty fully straightening or bending your knee
- A catching, clicking, grinding, or locking sensation during movement, especially with rotation
- Instability — a sensation your knee might give way or buckle
- Pain that worsens with stairs, squatting, kneeling, or any activity involving rotation
- Pain that’s activity-specific (certain movements hurt while others are fine)
For Hamilton residents, whatever your profession or lifestyle, the frustration is the same: suddenly you can’t do the things you normally do. The relief comes from knowing that recovery is usually rapid and complete.

Trinity Rehab Hamilton’s Evidence-Based Recovery Pathway
Your meniscus tear treatment is personalized, but follows proven progression that systematically rebuilds your knee’s function and your confidence.
Phase 1: Control Swelling and Protect Healing (Weeks 1-3)
Your initial priorities are protecting the healing tissue and controlling inflammation:
- RICE protocol — Rest (modified, not complete immobilization), Ice (frequent intervals), Compression (knee sleeve or wrap for stability), Elevation (above heart level)
- Non-narcotic pain management — Over-the-counter medications support comfort
- Manual therapy — Gentle hands-on techniques including joint mobilization and soft tissue massage reduce stiffness and promote healing
- Modality support — Electrical stimulation and therapeutic ultrasound decrease inflammation
- Protected movement — Careful, supervised exercises maintain knee mobility without stressing the tear
- Gait retraining — Correcting walking patterns to prevent compensatory strain on your other leg
Phase 2: Build Strength and Movement Control (Weeks 4-8)
This is the work phase where your knee becomes resilient:
- Progressive quadriceps strengthening — Systematic advancement from simple isometric contractions through dynamic exercises with increasing resistance. Strong quads are your primary shock absorbers and injury prevention
- Hamstring and hip strengthening — Balanced lower extremity strength ensures proper force distribution across the knee
- Core and glute activation — Your abdominal, back, and hip muscles contribute significantly to knee stability and movement quality
- Proprioceptive training — Balance exercises on unstable surfaces retrain your knee’s position sense and automatic stabilization reflexes
- Dry needling — Targeted trigger point therapy releases compensatory muscle tension
- Functional movement patterns — Advancing from simple exercises to complex, job-relevant or activity-relevant movements
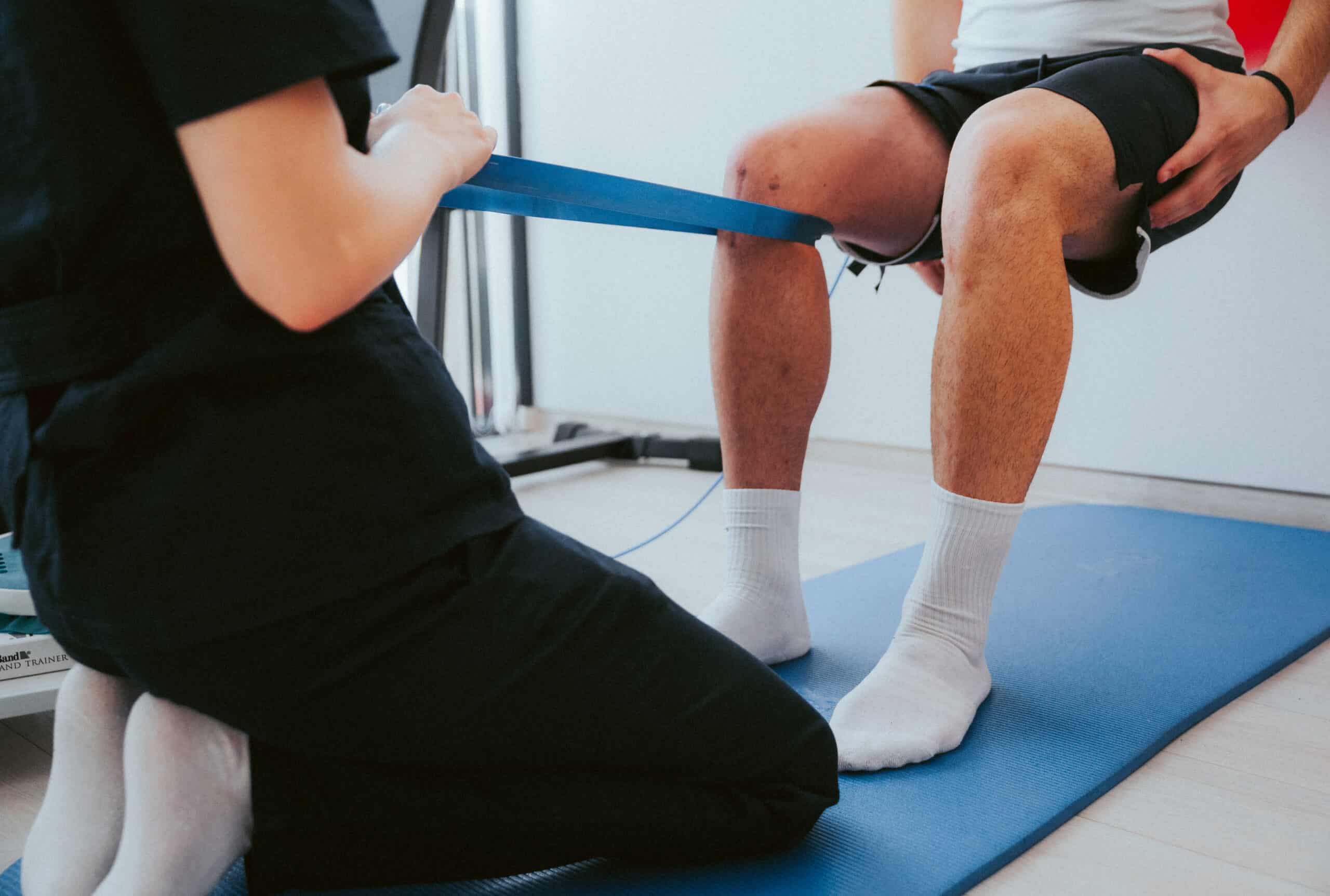
Phase 3: Return to Your Specific Activities (Weeks 9-12+)
The final phase systematically reintroduces your particular activities:
- Work-specific or activity-specific training — If your activity is professionally related (kneeling, climbing, heavy lifting), we train those movements. If it’s recreational or athletic, we train sport-specific movements. Your progression is tailored to your specific demands
- Progressive intensity increases — Gradually increasing demands so tissues adapt without re-injury risk
- Movement quality assurance — Ensuring proper form even as intensity increases
- Confidence building — Psychological readiness for return to activity, addressing any fear of re-injury
- Return-to-work or return-to-activity clearance — Objective testing of strength, proprioception, and activity-specific movements before full return
- EPAT/Shockwave therapy — When appropriate, this regenerative treatment uses acoustic pressure waves to stimulate tissue healing and optimize tissue quality
Understanding Your Tear Type
The specific pattern of your meniscus tear influences treatment approach:
- Radial tears — Most common. Cut across the meniscus fibers, usually from sudden twisting. Small tears in the outer (red) zone, which has blood supply, respond excellently to physical therapy
- Horizontal tears — Run along the meniscus length. Often associated with degenerative changes. These respond very well to conservative care
- Bucket-handle tears — A large vertical tear where part of the meniscus displaces. More likely to cause mechanical locking and potentially require arthroscopy. Physical therapy is still essential for recovery
- Flap tears — A meniscus section folding over. Usually manageable with physical therapy
- Complex tears — Multiple tear patterns. Require longer rehabilitation but generally respond to nonsurgical treatment
Long-Term Knee Health and Prevention
Maintaining meniscus health prevents future injuries:
- Year-round strength maintenance — Consistent quadriceps and hamstring strength protects your meniscus. This is especially important if your profession demands repetitive stress on your knees
- Movement quality focus — Proper technique for your specific activities (whether work or recreation) prevents future injuries. This might include proper lifting technique, squat form, or sport-specific movement patterns
- Appropriate footwear — Shoes matched to your activity type reduce abnormal knee loading
- Gradual intensity progression — Whether increasing work demands, training intensity, or recreational activity difficulty, progression should be gradual (approximately 10% per week)
- Recovery emphasis — Adequate rest between intense work or activity allows tissue adaptation. Consecutive days of high-demand activity increase injury risk
- Dynamic warm-up — Preparation before intense activity primes tissues and neuromuscular system
- Pain as communication — Persistent knee pain or swelling after activity or work is your body’s signal to modify demands, not push through
- Weight management — Maintaining healthy body weight significantly reduces knee stress. Every pound of excess weight translates to four pounds of force across the knee during walking
Why Hamilton Residents Choose Trinity Rehab Hamilton
Our clinic aligns with your community:
- Licensed physical therapists exclusively — Every session is one-on-one with a licensed clinician, not an aide or assistant
- No referral required — Begin treatment immediately in New Jersey without physician approval
- Work and activity-specific expertise — Our therapists understand the demands of various professions and recreational activities
- Evidence-based treatment — Our protocols reflect current research on meniscus tear recovery
- Culturally competent care — Our team serves Hamilton’s diverse population respectfully and effectively
- Flexible scheduling — Early morning, evening, and weekend appointments accommodate work and family schedules
- Insurance coordination — We work with most major plans and verify coverage upfront
- Accessible location — Conveniently serving Hamilton and Mercer County residents
Resume Your Life
At Trinity Rehab Hamilton, we understand what meniscus tear recovery means for our diverse community. Whether you’re an athlete, a worker in a demanding profession, a parent staying active, or someone whose meniscus tear has disrupted your routine, we’re committed to restoring your function and your life.
Common Questions About Meniscus Tears for Hamilton Residents
Can I continue working while recovering?
How long does recovery actually take?
Do I need an MRI before starting therapy?
What if my work is physically demanding?
Is surgery necessary?
Can I prevent meniscus re-injury?
What if I already have chronic pain from an older meniscus tear?
How does age affect recovery?
Schedule Your Evaluation
Start your recovery:
- Book your appointment at Trinity Rehab Hamilton
- Comprehensive assessment — Detailed knee and movement evaluation
- Personalized plan — Your specific recovery timeline and goals
No referral required. Schedule now.
Sources
- Katz, J. N., et al. (2013). Surgery versus physical therapy for a meniscal tear and osteoarthritis. New England Journal of Medicine, 368(18), 1675-1684.
- Sihvonen, R., et al. (2018). Arthroscopic partial meniscectomy for a degenerative meniscus tear: A 5-year follow-up of the FIDELITY randomized trial. British Journal of Sports Medicine, 52(21).
- American Academy of Orthopaedic Surgeons. (2024). Meniscus tears. OrthoInfo.




