Meniscus Tear Treatment in Flemington, NJ
Meniscus tear symptoms can make ordinary Flemington routines feel uncertain: uneven outdoor walking, longer drives, yard work, hills and stairs, return to hiking or fitness. Trinity Rehab Flemington helps patients understand what is driving knee pain, swelling, catching, stiffness, or twisting limits and build a careful plan for daily life, work, sport, and recovery.
Local Meniscus Tear Care in Flemington
Trinity Rehab Flemington is located at 276 US-202, Flemington, NJ 08822. Patients commonly visit from Flemington, Raritan Township, Readington, Clinton, Ringoes, Lebanon, and nearby communities for knee pain, meniscus tear symptoms, post-surgical knee rehab, swelling, catching, and difficulty with stairs or squatting.
The local pattern matters. Hunterdon County patients who need the knee to handle hills, outdoor property tasks, driving, and active weekends. That means the plan should reflect how your knee behaves during the actual routines you need to return to, not only a generic list of exercises.
A good Flemington meniscus tear plan asks what happens with stairs, turns, uneven ground, sit-to-stand movement, work tasks, exercise, driving, and the first steps after sitting. The answer shapes the starting point and the progression.
Meniscus Tear Symptoms We Watch For in Flemington
A meniscus tear can cause knee pain along the joint line, swelling, stiffness, catching, clicking, locking, buckling, or pain with twisting and squatting. Some patients can walk but cannot trust the knee on stairs. Others feel fine in straight-line walking but flare with pivots, kneeling, sports, or a long workday.
Swelling, Locking, and Catching
Swelling that returns after activity tells us the knee is still irritated or overloaded. Catching may reflect tissue irritation, movement control, swelling, or a mechanical issue. A truly locked knee, major trauma, or inability to bear weight should be medically evaluated.
Stairs, Squatting, and Twisting
For many Flemington patients, the problem shows up with uneven outdoor walking, longer drives, yard work. The evaluation should test the movement carefully and then rebuild strength and control in the same direction the patient needs in real life.
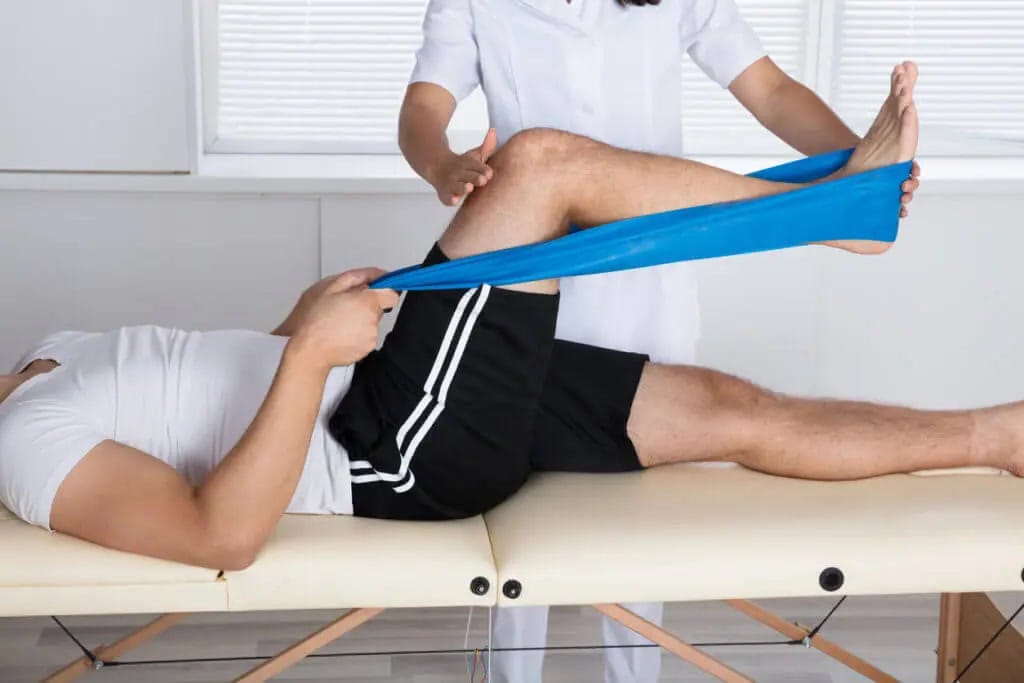
How The First Visit Works
Your first visit at Trinity Rehab Flemington is meant to make the knee problem clearer. Your therapist reviews how symptoms started, what has changed, whether swelling or locking is present, what medical care you have already had, and what activity you need to return to.
- Knee motion testing for bending, straightening, stiffness, and end-range pain.
- Swelling, tenderness, gait, stairs, squat mechanics, and sit-to-stand assessment.
- Quadriceps, hamstring, hip, calf, and balance testing to see what is contributing to knee load.
- Review of work, sport, commute, home, and recreation demands in the context of your symptoms.
- Red-flag screening for trauma, locked knee, unsafe weight bearing, infection signs, calf symptoms, or worsening pain.
- A practical home plan that matches the knee’s irritability level.
What Makes This More Than A City-Swap Knee Page
The Flemington page has to do more than name the town. It should reflect the real problems patients bring in: uneven outdoor walking, longer drives, yard work, hills and stairs, and return to hiking or fitness. Those details change how quickly therapy loads the knee and which movements need practice first.
Your therapist may use a balance task that compares the involved side with the other knee as an early checkpoint, then progress toward lighter work tasks before heavier lifts, carries, and long shifts. If the response is not right, the plan should change. Pushing through repeated swelling is not the same as productive strengthening.
For post-surgical patients from Flemington and nearby Readington, the key is matching protocol limits with practical daily milestones. A meaningful sign of improvement is a clearer plan for what to do if the knee flares. If pain follows a traumatic twist or fall and weight bearing is unsafe, medical evaluation comes first.
Treatment For Meniscus Tear Symptoms at Trinity Rehab Flemington
Treatment should be staged. Early care may focus on calming swelling, restoring comfortable motion, improving walking, and protecting the knee from repeated irritation. As symptoms allow, the plan should build quadriceps strength, hip control, balance, stair tolerance, squat mechanics, and return-to-work or return-to-sport capacity.
Conservative Physical Therapy
When conservative care is appropriate, therapy may include manual therapy, knee mobility work, strength training, balance, gait training, stair progression, activity modification, and a home program. The goal is not to pretend the tear does not matter; it is to improve the factors that the knee can adapt to safely.
Post-Surgical Meniscus Rehab
If you had surgery, rehab should follow your surgeon’s protocol. Your Flemington therapist may help progress motion, swelling control, weight bearing, strength, walking, stairs, squatting, and eventual return to work or sport. This is also where related post-surgical rehabilitation principles matter.

Flemington Goals That Shape The Plan
Your plan should be measured by life outside the clinic. In Flemington, that may mean uneven outdoor walking, longer drives, yard work, hills and stairs, return to hiking or fitness. Progress should be tracked by swelling response, walking tolerance, stairs, strength, balance, confidence, and whether the knee can handle the next level without a setback.
Related factors can matter too. Hip weakness, ankle mobility, hip pain, ankle pain, osteoarthritis, or a history of ACL injury can change how the knee is loaded. The plan should connect those pieces without turning the page into a generic knee article.
Adjunct treatments such as dry needling or EPAT/shockwave should only be discussed when clinically appropriate. They should support the broader movement plan, not replace strength, mobility, and functional progression.
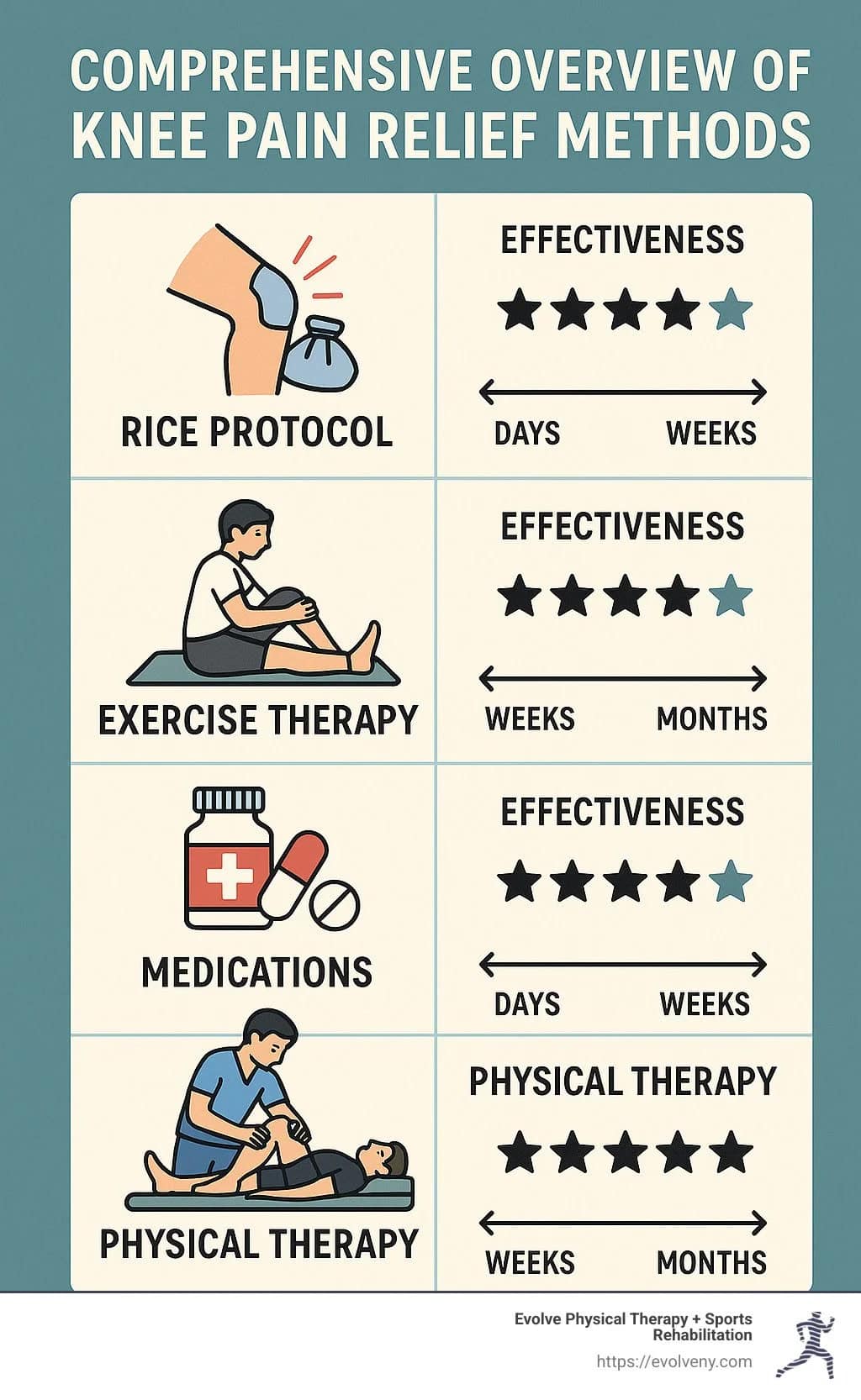
How We Progress Meniscus Rehab in Flemington
Phase 1: Calm The Knee Without Losing Motion
Early rehab usually focuses on swelling, comfortable range of motion, walking mechanics, and safe daily activity. For a Flemington patient, that may mean adjusting stairs, driving, work shifts, errands, or exercise volume so the knee can settle while still moving enough to avoid unnecessary stiffness.
This phase may include gentle mobility, quadriceps activation, gait work, swelling strategies, symptom-guided home exercises, and education about which movements are worth modifying for now. The goal is not to make the patient fearful of bending the knee; it is to find the level of motion and loading the knee can tolerate today.
Phase 2: Rebuild Strength and Control
As symptoms allow, the plan should build quadriceps strength, hamstring support, hip control, calf strength, balance, and better squat and stair mechanics. Meniscus symptoms often flare when the knee rotates or compresses under poor control, so strengthening should be paired with movement quality.
This is where local goals become useful. uneven outdoor walking, longer drives, yard work require more than a simple straight-leg raise. The knee needs graded practice with the positions, distances, and surfaces that make sense for the patient’s week.
Phase 3: Return To Work, Sport, and Life
The later phase should bridge the gap between feeling better and being ready. A runner may need a walk-jog progression. A court-sport athlete may need lateral movement, cutting, and deceleration. A worker may need kneeling, lifting, stairs, or prolonged standing. A post-surgical patient may need protocol-based milestones before returning to deeper squatting or pivoting.
What To Avoid While The Knee Is Irritable
The goal is not to scare patients away from movement. The goal is to avoid repeatedly provoking the same irritated tissue while the knee is trying to calm down. Deep twisting, repeated pivoting, sudden jumps in walking distance, aggressive kneeling, heavy squats, or pushing through swelling may slow progress for some patients.
Your Flemington therapist can help you decide what to keep, what to modify, and what to delay. For example, one person may continue upper-body gym work and flat walking while avoiding pivoting drills. Another may need a temporary stair strategy, shorter errands, or modified work tasks. These choices should be based on symptoms and goals, not a one-size-fits-all restriction list.
If symptoms include a locked knee, major trauma, inability to bear weight, fever, calf swelling, numbness, or rapidly worsening pain, that is a medical-evaluation situation. The safest rehab plan is the one that knows when PT is appropriate and when the next step should involve a physician.
Clinic Proof for Flemington
Trinity Rehab Flemington serves patients in Flemington, Raritan Township, Readington, Clinton, Ringoes, Lebanon, and nearby communities. The clinic proof on this page is intentionally specific: address, map context, local review widget, nearby towns, and realistic local knee goals instead of a city-swap paragraph.
- Clinic: Trinity Rehab Flemington
- Address: 276 US-202, Flemington, NJ 08822
- Phone: (908) 751-7330
- Map: View Trinity Rehab Flemington on Google Maps
Patient Reviews
Local reviews help Flemington patients see real clinic experience before scheduling. This spoke uses the location-specific Trinity Rehab review widget rather than a generic placeholder.
Flemington Meniscus Rehab For Walking, Stairs, And Knee Confidence
For Flemington patients with meniscus symptoms, the practical goal is often to walk, use stairs, return to work, and exercise with less catching, swelling, or uncertainty.
Your therapist may assess knee motion, swelling, quad and hip strength, balance, walking mechanics, and sport or work demands. Locking, major swelling, or traumatic instability may need medical review first.
Related options include knee pain physical therapy, ACL rehab, and the Flemington physical therapy clinic page.
Frequently Asked Questions
What makes meniscus tear therapy in Flemington local?
Can I start PT in NJ without a referral?
What if my knee catches or locks?
Will therapy help if I already had meniscus surgery?
How long does meniscus rehab take in Flemington?
Start With A Clear Knee Plan
If knee pain, swelling, catching, stiffness, stairs, squatting, twisting, sport, or work limits are changing your Flemington routine, start with an evaluation. The goal is to understand what is driving symptoms and rebuild the knee for the activity you actually need.




