Meniscus Tear Treatment in East Brunswick, NJ — Trinity Rehab
East Brunswick is a thriving Middlesex County community where families prioritize their children’s athletic development and personal fitness. The East Brunswick Bears athletics program is a source of community pride, and youth sports participation rates here are notably high. Parents and kids alike invest time in competitive sports, recreational activities, and the fitness culture that makes this community thrive. Add Crystal Springs community pool, neighborhood running clubs, and casual recreational sports, and you have a population that values movement and physical activity.
This commitment to active living is wonderful — until the moment something goes wrong. A meniscus tear during an East Brunswick Bears practice, during recreational tennis at a local court, or while running to stay fit can feel like your entire identity is temporarily stripped away. The initial panic — “Do I need surgery? How long am I sidelined?” — is quickly followed by a more hopeful realization: the vast majority of meniscus tears respond beautifully to structured physical therapy. You’ll return to your sport, your fitness routine, and your active lifestyle, typically without ever visiting an operating room. Understanding meniscus tear symptoms is crucial for anyone engaged in physical activity. Recognizing signs such as swelling, pain in the knee joint, or difficulty moving the leg can lead to quicker and more effective treatment options. By consulting with a healthcare professional as soon as these symptoms arise, you can ensure a smoother recovery process and get back to your favorite activities in no time. Understanding the causes of meniscus tear injuries can help in prevention and rehabilitation. Common factors include sudden twists of the knee, heavy lifting, or degenerative changes due to aging. By recognizing these risks, athletes and active individuals can take proactive measures to protect their knees and maintain their passion for sports and exercise. Understanding the common symptoms of meniscus tear can help you identify the injury early on. Typical signs include pain, swelling, and difficulty in bending or straightening the knee, which can start to limit your activities. By being aware of these symptoms, you can seek appropriate care sooner and improve your chances of a full recovery. Understanding the symptoms of meniscus tear injuries can be crucial for a quick recovery. Common signs include swelling, pain, and a decreased range of motion, which can help in determining the next steps. Early recognition of these symptoms may lead to more effective treatment options and a faster return to the activities you love. Understanding meniscus tear symptoms and diagnosis can help you identify the injury early and seek appropriate care. Recognizing signs like swelling, stiffness, or a popping sensation can guide your next steps. This awareness not only aids in recovery but also empowers you to prevent future injuries, ensuring that your active lifestyle remains uninterrupted.
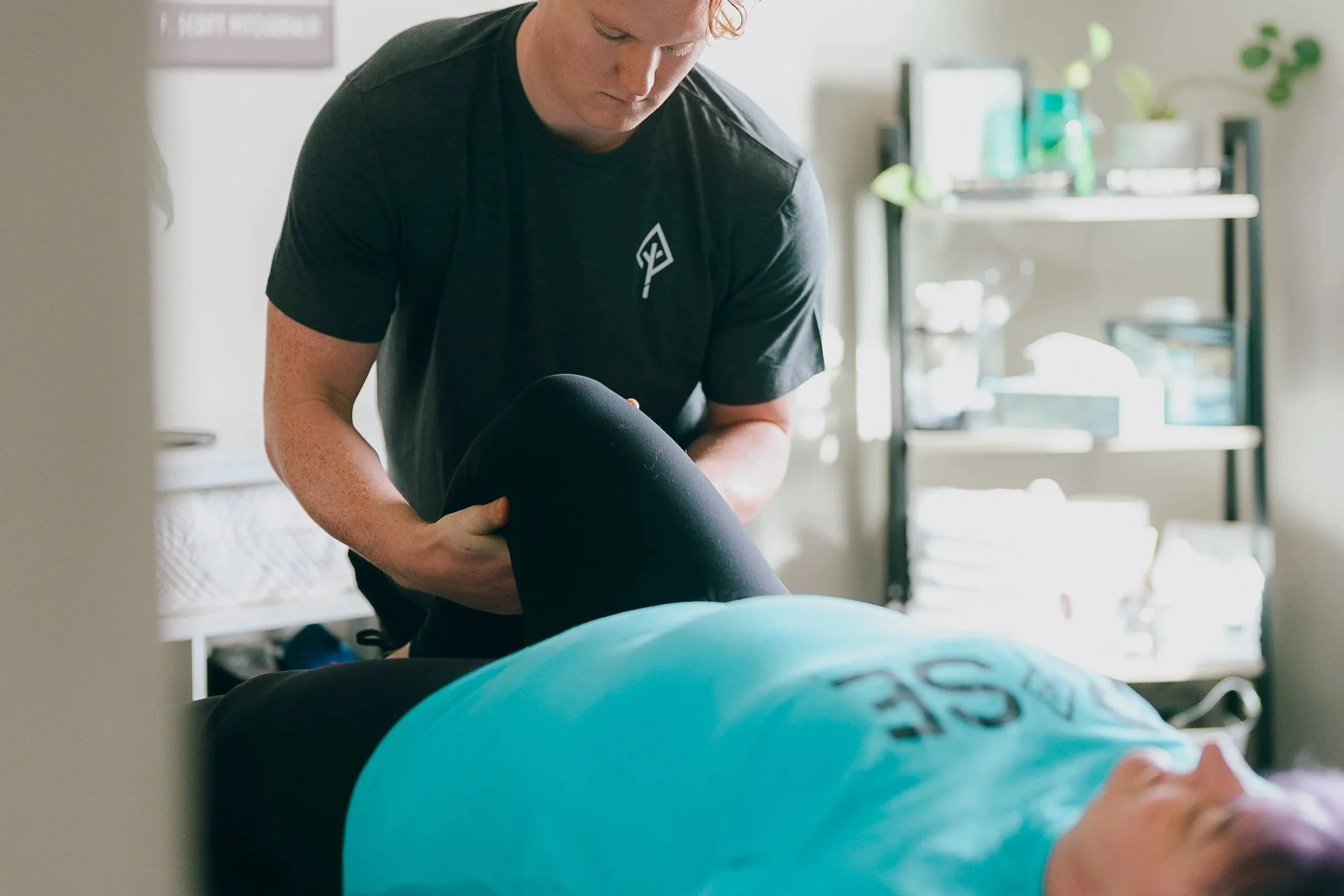
The Meniscus: Your Knee’s Built-in Shock Absorber
Your knee’s meniscus is a C-shaped cartilage disc that sits between your thighbone and shinbone, performing three critical functions. First, it absorbs shock — which is why landing from a jump or running doesn’t hurt your bones. Second, it distributes weight evenly across the joint, preventing cartilage wear. Third, it provides stability, preventing your knee from shifting unexpectedly. You have two menisci per knee: medial (inner) and lateral (outer).
When a meniscus tears, these protective functions diminish immediately. Your knee becomes less stable, less cushioned, and more vulnerable to progressive cartilage wear. However, this cascade is entirely preventable with proper treatment. Modern research shows physical therapy produces outcomes matching or exceeding surgery for most meniscus tears, particularly in adults.
Why East Brunswick Athletes and Active Adults Develop Meniscus Tears
The East Brunswick lifestyle creates predictable injury patterns:
- Bears athletics and youth sports — Competitive programs emphasizing cutting, pivoting, and directional changes create acute meniscus tears during plant-and-cut movements. These are high-velocity rotational injuries
- Multi-sport participation — Young athletes competing in multiple sports increase training volume without adequate recovery, leading to fatigue-induced overuse injuries and acute tears
- Parent-athlete synchronization — Parents staying active alongside their sports-participating children sometimes sustain injuries during family athletic activities
- Swimming and water activities — While swimming is generally low-impact, certain strokes and pool-side activities create rotational stress on knees
- Recreational fitness growth — More adults choosing running, cycling, and fitness classes creates overuse injury opportunities, particularly in people who rapidly increase intensity
- Age-related tissue changes — In older East Brunswick residents, degenerative meniscus tears develop from cartilage weakening, where routine activities (kneeling, squatting) can precipitate tears in compromised tissue
Recognizing a Meniscus Tear in East Brunswick Athletes
The injury pattern is usually distinctive:
- A pop, snap, or tearing sensation at the moment of injury
- Rapid or gradual swelling (sometimes within 30 minutes, sometimes over 24 hours)
- Sharp, well-localized pain on the inner or outer side of the knee
- Difficulty fully straightening or bending your knee; some athletes describe feeling “stuck” in a bent position
- A catching, clicking, grinding, or clunking sensation during movement, especially with twisting
- Instability — a sensation the knee might give way or buckle
- Pain that worsens with stairs, running, jumping, or any activity involving rotation
- Pain during certain movements but not others (for example, straight-line running might be okay, but cutting is painful)
For East Brunswick athletes, particularly those in the Bears programs, the psychological impact is significant. Being sidelined during season is frustrating and isolating. The good news: with proper rehabilitation, most athletes return to full competition within 8-12 weeks.

Trinity Rehab East Brunswick’s Rehabilitation Pathway
Your meniscus tear treatment is individualized but follows proven progression designed to restore your knee’s function systematically.
Phase 1: Pain Management and Protection (Weeks 1-3)
The immediate focus is controlling inflammation and protecting healing tissue:
- RICE protocol — Rest (modified activity, not complete immobilization), Ice (regular intervals to reduce swelling), Compression (knee sleeve or wrap for stability and comfort), Elevation (above heart level when possible)
- Pain management — Non-narcotic medications support comfort during healing
- Manual therapy — Gentle joint mobilization and soft tissue techniques reduce stiffness, improve circulation, and promote healing
- Modality support — Electrical stimulation and therapeutic ultrasound decrease inflammation
- Range-of-motion preservation — Careful, supervised exercises maintain knee mobility without stressing the tear
- Gait normalization — Retraining your walking pattern to prevent compensatory strain on your healthy leg
Phase 2: Strength Development and Proprioception (Weeks 4-8)
This is the work phase where your knee becomes resilient:
- Progressive quadriceps strengthening — Systematic progression from isometric contractions to dynamic, weight-bearing exercises. Quad strength is your primary injury prevention tool
- Hamstring and hip strengthening — Balanced lower extremity strength ensures proper force distribution across the knee
- Core and glute activation — Your abdominal, back, and hip muscles contribute significantly to knee stability and movement quality
- Proprioceptive training — Balance exercises on unstable surfaces (balance pads, foam rollers, single-leg stands) retrain automatic stabilization reflexes that prevent re-injury
- Dry needling — Targeted trigger point therapy releases compensatory muscle tension that accumulates during the injury and altered movement phase
- Functional movement progression — Advancing from simple exercises to complex, sport-relevant movements performed with perfect technique
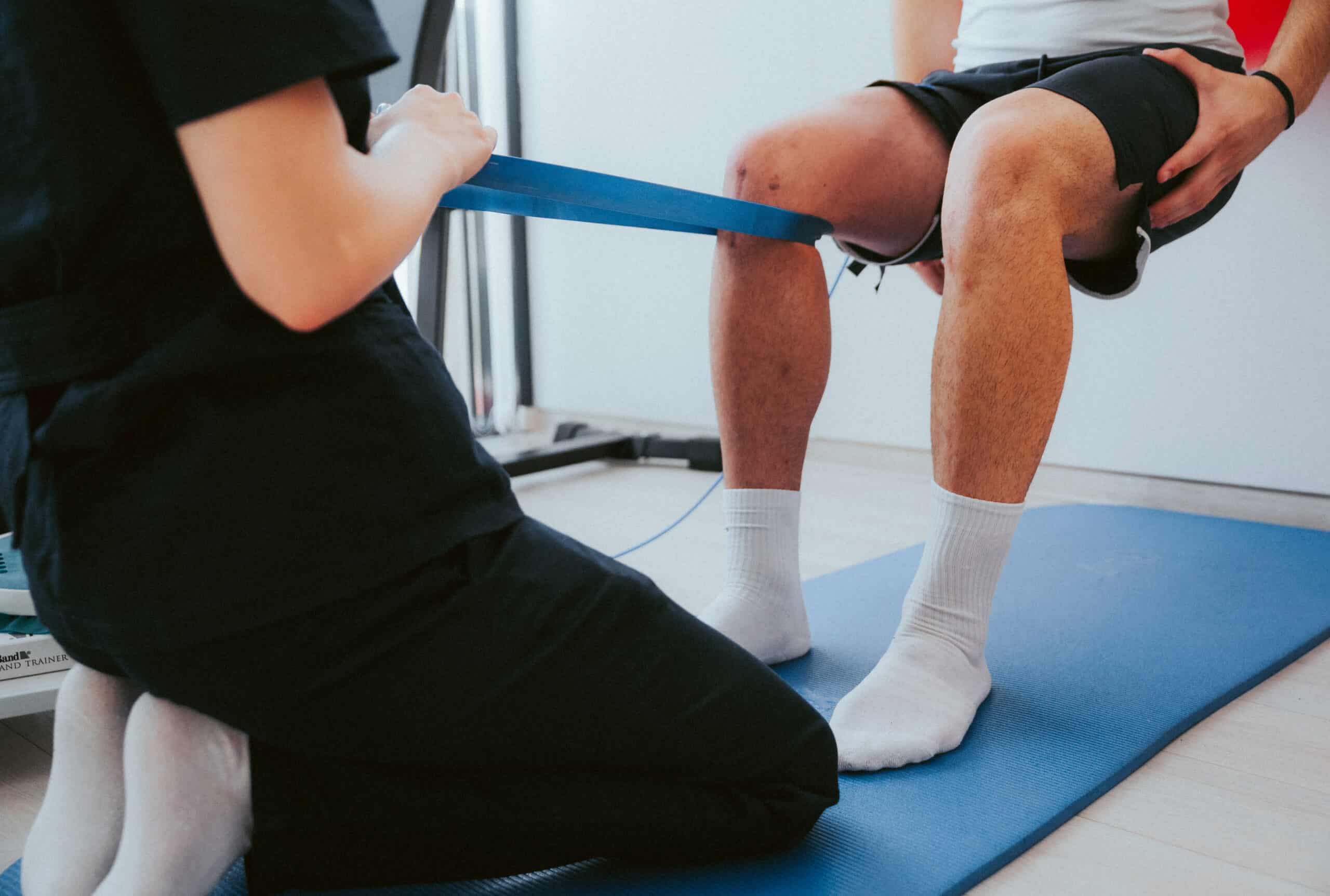
Phase 3: Return to Sport (Weeks 9-12+)
The final phase bridges clinical recovery and actual sport participation:
- Sport-specific training — Cutting drills, acceleration/deceleration work, lateral movement, and directional changes specific to your sport. For Bears athletes: linebacker drills, cutting patterns, agility work matching practice demands
- Plyometric progression — Controlled jumping and landing drills prepare tissues for sport demands. Progression is methodical: bilateral hops, single-leg hops, directional changes, cutting
- Competitive simulation — By the end of this phase, you’re performing movements closely matching game conditions
- Psychological readiness — Confidence-building is part of return-to-sport. Your therapist addresses fear of re-injury and builds trust in your knee
- EPAT/Shockwave therapy — For appropriate cases, this advanced regenerative treatment uses acoustic pressure waves to stimulate tissue healing and optimize tissue quality
Understanding Tear Types and Treatment Paths
Your specific tear pattern influences treatment strategy:
- Radial tears — Most common in young athletes. Cut across the meniscus fibers, usually from sudden twisting. Small tears in the vascular outer zone respond excellently to physical therapy
- Horizontal tears — Run along the meniscus length. Often associated with degenerative changes but can occur in young athletes with repetitive compressive loading. These respond very well to conservative care
- Bucket-handle tears — A large vertical tear where part of the meniscus flips into the joint center. More likely to cause mechanical locking and potentially require arthroscopy, though physical therapy remains essential for post-surgical recovery
- Flap tears — A meniscus section folding over. Usually manageable with physical therapy
- Complex tears — Multiple tear patterns. Typically require longer rehabilitation but generally respond to nonsurgical treatment
Long-Term Knee Health and Re-Injury Prevention
Your recovery goal isn’t just returning to sport — it’s preventing meniscus re-injury:
- Year-round strength maintenance — Off-season training prevents deconditioning and injury risk when you return to sport. A key finding: athletes who maintain strength across seasons have dramatically lower re-injury rates
- Movement quality focus — Poor landing mechanics, inward knee collapse, and asymmetrical movement patterns are primary re-injury risk factors. Conscious technique practice prevents problems
- Gradual intensity progression — Increasing training volume or intensity too rapidly creates re-injury risk. Professional guidelines suggest 10% weekly increases maximum
- Recovery emphasis — Training without adequate rest creates fatigue-induced movement degradation. Rest days are injury prevention, not laziness
- Sport-specific warm-up routines — Dynamic preparation before practice or games primes neuromuscular stability and injury prevention
- Footwear optimization — Shoes matched to your sport and foot type reduce abnormal loading
- Early pain recognition — Persistent knee pain after practice or games is your body’s signal to modify activity, not something to push through
Why East Brunswick Families Trust Trinity Rehab East Brunswick
Our clinic is built for your community:
- Licensed physical therapists exclusively — Every session is one-on-one with a licensed clinician, not an aide or assistant
- No referral required — Begin treatment immediately in New Jersey without waiting for physician approval — critical when you’re eager to return to your sport
- Sport-specific expertise — Our therapists understand the specific demands of Bears athletics, competitive youth sports, and recreational fitness
- Evidence-based protocols — Our treatment reflects current research on meniscus tear recovery and return-to-sport
- Flexible scheduling — Early morning, after-school, and evening appointments accommodate youth sports schedules and family needs
- Insurance coordination — We verify coverage upfront so you understand costs before your first visit
- Parent education — We teach families about recovery expectations, re-injury prevention, and appropriate return-to-sport timelines
- Convenient location — Serving East Brunswick families and nearby communities
Return to the Game
At Trinity Rehab East Brunswick, we understand what meniscus tear recovery means for young athletes and their families. Your goal is clear: return to your sport stronger and more resilient. That’s our goal too.
Frequently Asked Questions for East Brunswick Athletes
When can I return to Bears athletics or my competitive sport?
Can my child participate in other sports while recovering from a meniscus tear?
Do we need an MRI before starting therapy?
What causes meniscus tears in young athletes?
Can my child re-injure the meniscus?
Is surgery necessary?
How do we know if recovery is progressing appropriately?
What if my child feels pain during return-to-sport?
Schedule Your Evaluation
Start your recovery:
- Book your appointment at Trinity Rehab East Brunswick
- Comprehensive assessment — Detailed knee and movement evaluation
- Sport-specific planning — Your return-to-sport timeline and protocol
No referral required. Schedule now.
Sources
- Katz, J. N., et al. (2013). Surgery versus physical therapy for a meniscal tear and osteoarthritis. New England Journal of Medicine, 368(18), 1675-1684.
- Sihvonen, R., et al. (2018). Arthroscopic partial meniscectomy for a degenerative meniscus tear: A 5-year follow-up of the FIDELITY randomized trial. British Journal of Sports Medicine, 52(21).
- American Academy of Orthopaedic Surgeons. (2024). Meniscus tears. OrthoInfo.





