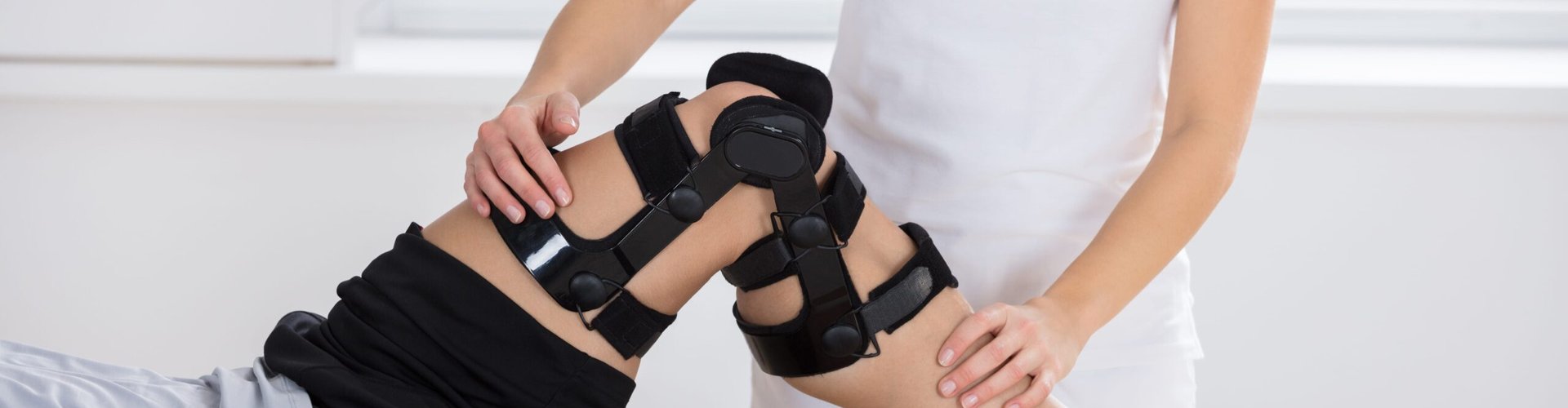
ACL TREATMENT PHYSICAL THERAPY IN EAST BRUNSWICK, NJ
Friday nights under the lights at East Brunswick High School carry a particular weight here. The Bears’ girls soccer program has built a dynasty — multiple state championships earned through thousands of hours of cuts, pivots, and all-out sprints on fields that demand everything from a young athlete’s knees. But it only takes one awkward landing, one sudden change of direction on rain-soaked turf, for an anterior cruciate ligament injury to rewrite a season. And ACL tears don’t just happen to high school athletes. They happen to the Wipro engineer who joined a weekend basketball league to stay active, to the Strides Pharma lab technician who slipped on a wet warehouse floor, and to the parent who twisted a knee chasing their kids through Crystal Springs Family Waterpark on a July afternoon.
If you or someone in your family is facing an ACL injury in East Brunswick, understanding what comes next — and why physical therapy is the backbone of every successful recovery — is the first step toward getting back to the life you know.
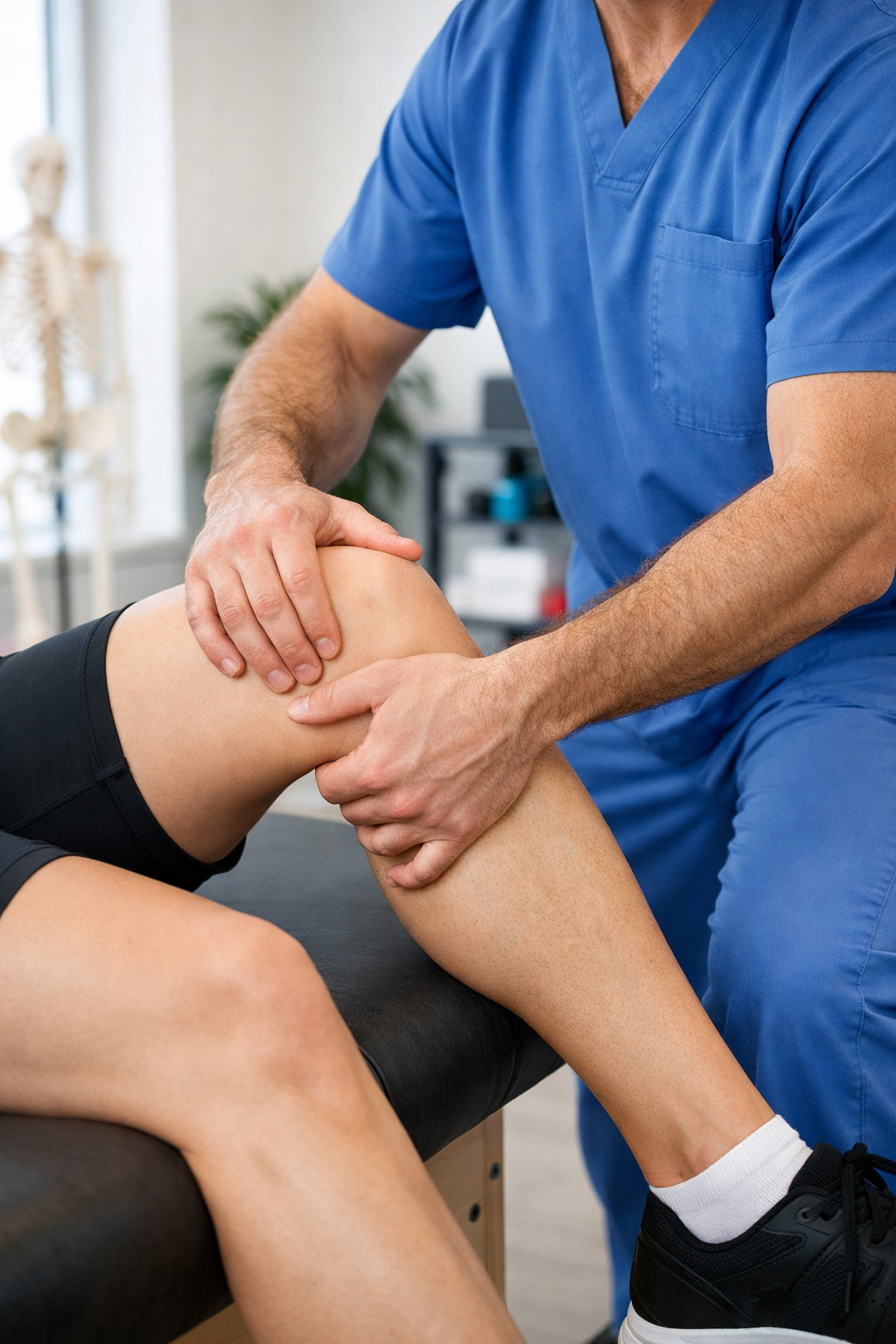
WHY ACL RECOVERY MATTERS MORE THAN YOU THINK
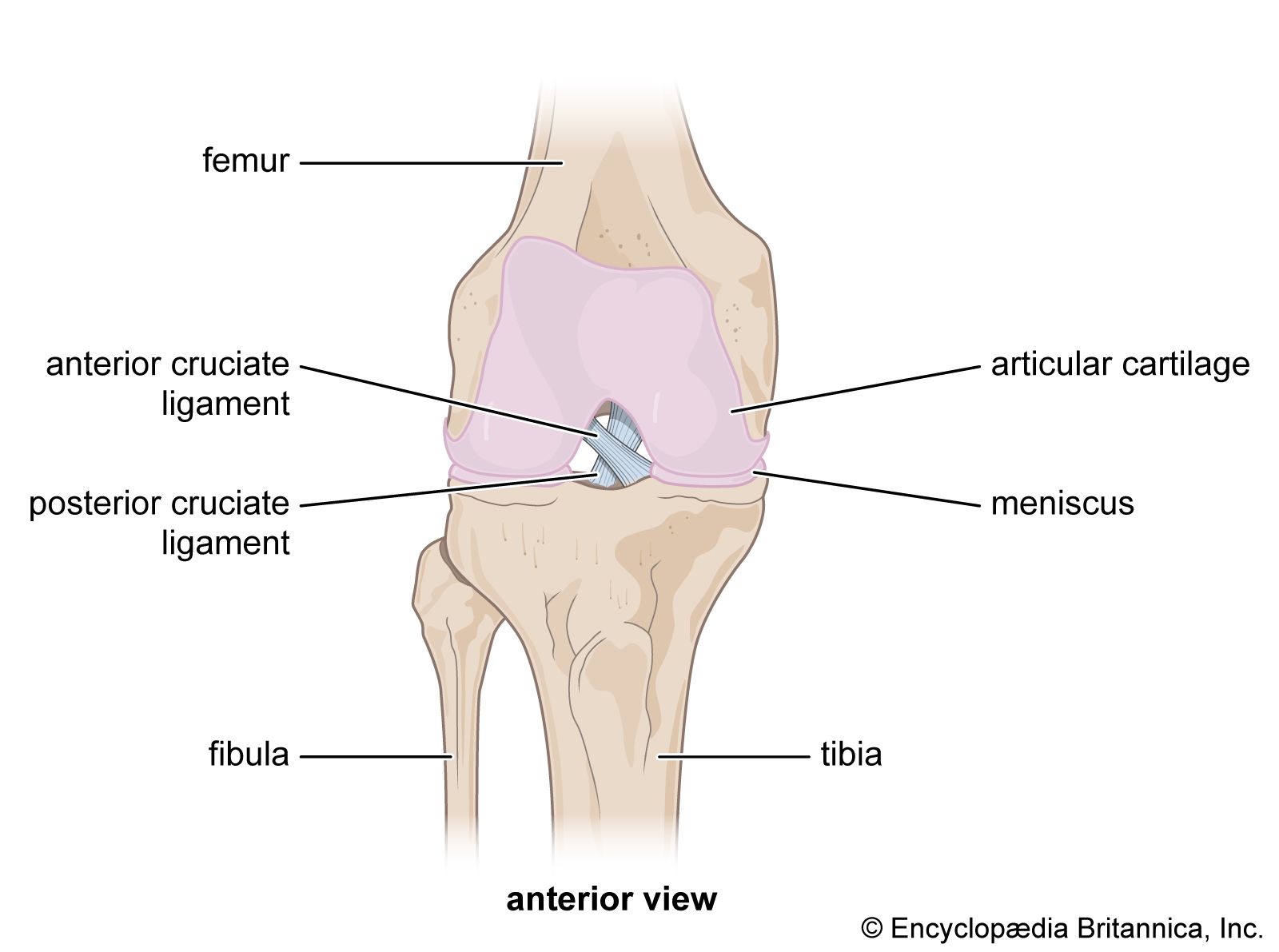
The anterior cruciate ligament is a short, powerful band of tissue inside the knee joint that prevents the shinbone from sliding forward and keeps the knee stable during rotation. When it tears, the immediate damage is obvious: pain, swelling, a feeling that the knee “gave out.” But the longer-term consequences are what make proper rehabilitation essential.
Without structured recovery, an ACL tear leads to chronic knee instability, accelerated cartilage breakdown, and a significantly higher risk of early-onset arthritis. Research consistently shows that patients who complete full rehabilitation — whether after anterior cruciate ligament reconstruction or through a non-surgical pathway — return to higher levels of knee function, report less pain, and sustain fewer re-injuries than those who cut corners.
In East Brunswick, where families are active year-round and nearly one in four residents is under 18, protecting long-term knee health isn’t abstract. It determines whether a Bears lacrosse player competes in college, whether a SciSafe biostorage technician can stay on their feet through a full shift, or whether a retiree can keep walking the trails at Frost Woods without pain.
COMMON CAUSES OF ACL INJURIES IN EAST BRUNSWICK
ACL tears follow predictable patterns, and many of them map directly onto life in this community.
Youth and High School Sports
East Brunswick’s athletic programs are a point of pride — and a source of real orthopedic risk. The Bears’ girls soccer team, with its history of state championships, places enormous rotational stress on the knee joint every season. Boys volleyball, another powerhouse with five state titles, demands explosive jumping and landing. Football, boys tennis, girls basketball, and lacrosse all contribute to a sports culture where anterior cruciate ligament injuries are not rare. Female athletes, particularly in soccer and basketball, face ACL tear rates two to four times higher than males due to differences in biomechanics and neuromuscular control.
Recreational and Community Activity
Hiking at Tamarack Hollow Preserve, running trails through Frost Woods, playing pickup games at Tices Lane Park or Great Oak Park — these keep residents active but also create exposure. An uneven trail surface, a misstep at Pine Ridge Park, or an aggressive move at East Brunswick Racquet Club can produce the sudden force that ruptures an ACL.
Workplace and Commuter Injuries
East Brunswick is a commuter town with a significant professional workforce. Employees at Wipro Limited, Strides Pharma, AnnexMed, Alpha Consulting, and East Brunswick Public Schools navigate industrial environments or rush through transit hubs daily. Slips, falls, and awkward landings at work are a meaningful source of ACL injuries — and they qualify for work injury rehabilitation pathways that get employees back to their jobs safely.
SIGNS AND SYMPTOMS OF AN ACL TEAR
Recognizing an ACL injury early changes outcomes. Watch for:
- A “pop” at the moment of injury — most patients hear or feel a distinct pop in the knee
- Rapid swelling — the knee typically swells within hours, not days
- Instability — the knee buckles or feels like it cannot support weight
- Loss of range of motion — difficulty fully straightening or bending the knee
- Pain along the joint line — particularly with any attempt to pivot or change direction
If you notice these symptoms after a sports play, a fall at Bicentennial Park, or a slip at work, seek evaluation promptly. Early assessment by a physical therapist allows rehabilitation to begin sooner, which directly improves outcomes.
HOW PHYSICAL THERAPY HELPS: THE PHASE-BASED APPROACH
ACL treatment physical therapy is not a single protocol. It is a structured, progressive journey managed by a physical therapist who adapts each phase to the patient’s goals and timeline. At Trinity Rehab East Brunswick, we follow an evidence-based, phase-based model whether you are recovering from ACL surgery or pursuing a non-surgical path.
Prehabilitation: Starting Before Surgery
For patients scheduled for anterior cruciate ligament reconstruction, prehabilitation begins before the operating room. The goal is to reduce swelling, restore knee motion, and build quadriceps and hamstring strength so the knee enters surgery in the best possible condition.
Prehab typically includes:
- Gentle range of motion exercises to maintain knee flexibility
- Quadriceps activation drills (the quad often “shuts down” after an ACL tear)
- Hamstring curls and isometric holds to preserve hamstring strength
- Swelling management through elevation, compression, and ice
A Bears football player facing reconstruction after a sectional playoff injury and a Ceres Terminals logistics worker recovering from a loading dock fall both benefit from prehab — it shortens recovery time and improves outcomes.

Phase 1: Protection and Early Mobility (Weeks 0-2)
Immediately after ACL reconstruction, the priority is protecting the healing graft while preventing the joint from stiffening.
- Restoring passive range of motion, especially full knee extension
- Light quadriceps activation to combat muscle inhibition
- Gentle manual therapy to manage scar tissue and maintain joint mobility
- Patellar mobilization to keep the kneecap tracking properly
- Pain and swelling control
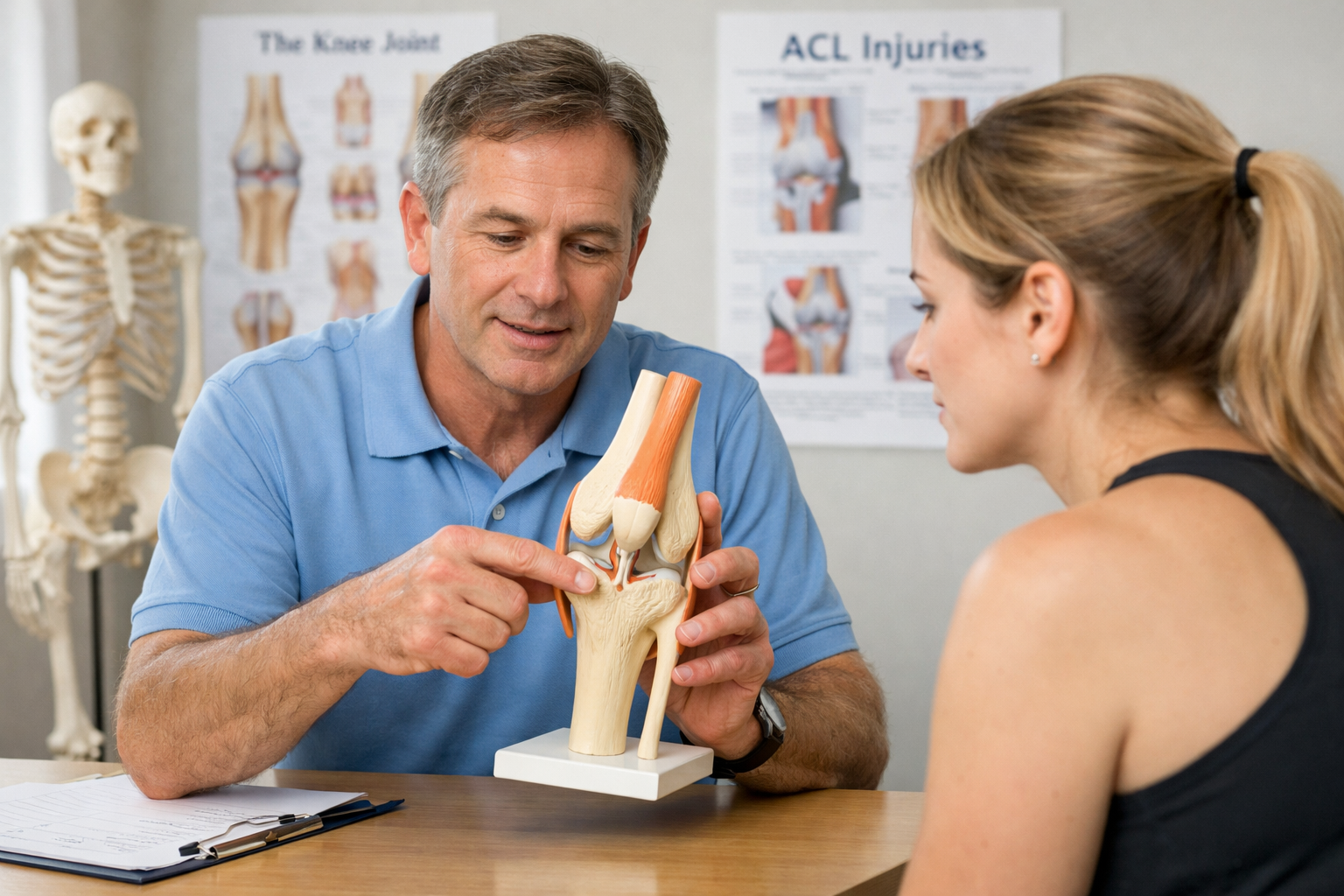
Phase 2: Building a Foundation (Weeks 2-6)
As healing progresses, treatment shifts toward rebuilding basic muscle strength and restoring functional knee motion.
- Progressive strengthening exercises for the quadriceps, hamstrings, glutes, and hip stabilizers
- Stationary cycling and pool-based exercise for low-impact conditioning
- Balance exercises on stable surfaces to begin retraining proprioception — the knee’s ability to sense its position in space
- Continued manual therapy to address stiffness and soft tissue restrictions
Phase 3: Strengthening and Neuromuscular Control (Weeks 6-12)
This phase marks a significant shift. Patients begin loading the knee more aggressively and training the neuromuscular patterns that prevent re-injury.
- Single-leg strengthening: step-ups, lunges, single-leg squats
- Progressive balance exercises on unstable surfaces
- Introduction of light agility drills — lateral shuffles, cone work
- Proprioception training that mimics real-world demands
- Continued focus on hamstring strength, which acts as a critical stabilizer for the ACL
For a Bears girls basketball player aiming to return for her senior season, this phase is where the knee starts feeling like a knee again — not a liability.
Phase 4: Sport-Specific and Functional Training (Weeks 12-20)
Rehabilitation now targets the specific demands the patient will face when they return to activity.
- Running progression: from jogging to tempo runs to sprinting
- Plyometric training: box jumps, depth jumps, bounding — the explosive movements that replicate sport demands
- Sport-specific drills tailored to the patient’s activity (cutting patterns for soccer, jumping mechanics for volleyball, lateral movement for tennis)
- Advanced proprioception and reaction-time training
- Ongoing strengthening to ensure quadriceps and hamstring muscle strength meets benchmarks
A Bears boys tennis player returning after an ACL tear needs lateral agility and rapid deceleration. A weekend trail runner at Tamarack Hollow needs confidence on uneven terrain. This phase builds both.
Phase 5: Return to Sport and Long-Term Maintenance (Weeks 20+)
Clearance for full return to sport is based on objective testing, not just time on the calendar. We assess:
- Limb symmetry index: the injured leg must produce at least 90% of the strength and power of the healthy leg
- Hop test battery: single-leg hop, triple hop, crossover hop
- Dynamic movement quality during cutting, pivoting, and landing
- Psychological readiness — confidence in the knee matters as much as physical benchmarks
Patients who pass these criteria have significantly lower re-injury rates. Those who return before meeting them face substantially elevated risk for a second ACL tear.
THE NON-SURGICAL PATHWAY
Not every ACL tear requires surgery. For patients with partial tears, lower activity demands, or specific medical considerations, a structured non-surgical rehabilitation program can restore knee stability and function. The same phase-based progression applies, with emphasis on building the muscular strength and proprioception that compensate for a compromised ligament.
A Wipro software engineer who tore an ACL hiking at Frost Woods and primarily needs to walk, cycle, and work comfortably may be an excellent candidate for non-surgical management. The decision is always individualized and made collaboratively between patient, surgeon, and physical therapist.
ADVANCED TECHNIQUES THAT ACCELERATE RECOVERY
Trinity Rehab East Brunswick offers evidence-based technologies that complement traditional rehabilitation.
Blood Flow Restriction (BFR) Training
Blood flow restriction uses a specialized tourniquet to partially restrict venous blood flow during low-load exercise, allowing patients to build meaningful muscle strength — particularly in the quadriceps — without the heavy loads that could stress a healing graft. BFR is especially valuable in early post-surgical phases when the knee cannot tolerate high resistance.
Neuromuscular Electrical Stimulation (NMES)
Neuromuscular electrical stimulation delivers controlled electrical impulses to the quadriceps to combat muscle inhibition after ACL surgery. When the brain “forgets” how to activate the quad, NMES bridges the gap, helping patients regain muscle strength faster than exercise alone.
Dry Needling
Dry needling targets myofascial trigger points in the muscles surrounding the knee — particularly the quadriceps, hamstrings, IT band, and calf. By releasing these painful knots, dry needling restores muscle function and reduces compensatory movement patterns that develop after an ACL injury.
EPAT / Shockwave Therapy
EPAT (Extracorporeal Pulse Activation Technology) delivers acoustic pressure waves to injured tissue, stimulating blood flow and cellular repair. Shockwave therapy is particularly effective for addressing lingering patellar tendon pain and soft tissue restrictions that can stall ACL recovery.
INJURY PREVENTION: PROTECTING THE ACL BEFORE IT TEARS
In a community where youth sports participation is high and families are active at places like East Brunswick Soccer Club, Raritan Valley YMCA, and Tamarack Golf Course, prevention matters as much as treatment.
Evidence-based ACL injury prevention programs focus on:
- Neuromuscular training — teaching athletes to land, cut, and decelerate with proper knee alignment
- Hamstring and hip strengthening — reducing the quad-dominant movement patterns that increase ACL risk
- Plyometric training with coaching — building explosive power while reinforcing safe mechanics
- Balance and proprioception drills — improving the body’s ability to react and stabilize in real time
- Education — helping athletes, coaches, and parents recognize risk factors early
These programs reduce ACL tear rates by 50-70% in at-risk populations. For East Brunswick High School athletes competing at the state championship level, a structured injury prevention program is essential.
WHY CHOOSE TRINITY REHAB EAST BRUNSWICK
Trinity Rehab East Brunswick offers:
- One-on-one treatment with a licensed physical therapist at every visit — no hand-offs to aides or technicians
- Evidence-based, phase-specific protocols that follow current research on ACL rehabilitation
- Advanced treatment options including blood flow restriction, neuromuscular electrical stimulation, dry needling, and EPAT
- Sport-specific return-to-play programs designed for the sports East Brunswick athletes actually play — soccer, volleyball, tennis, football, basketball, lacrosse
- Work injury rehabilitation for employees at Wipro, Strides Pharma, SciSafe, AnnexMed, and other local employers
- A convenient location at 465 Cranbury Rd, Ste 103, East Brunswick, NJ 08816 — easily accessible from Route 18
We treat the full spectrum of sports injuries, hip and knee pain, and orthopedic conditions affecting East Brunswick residents at every stage of life.
Inside Our East Brunswick Clinic




RELATED CONDITIONS & TREATMENTS
ACL injuries are just one of the many conditions we treat at Trinity Rehab East Brunswick. Explore our full range of conditions we treat or learn more about specific treatment approaches:
FREQUENTLY ASKED QUESTIONS
How long does ACL rehabilitation take?
Can I avoid ACL surgery and recover with physical therapy alone?
My teenager plays soccer for East Brunswick High School. When can they return to competition after an ACL tear?
Does Trinity Rehab East Brunswick treat work-related ACL injuries?
What makes blood flow restriction training effective for ACL recovery?
An ACL tear does not have to define your season, your career, or your quality of life. Whether you are a Bears athlete, a professional in East Brunswick’s pharma and biotech corridor, or a parent who wants to keep up with your family at Dallenbach Lake and Frost Woods, structured ACL treatment physical therapy gets you there.
Schedule your appointment at Trinity Rehab East Brunswick to start your recovery with a physical therapist who understands what your knee needs — and what your life demands.
Trinity Rehab East Brunswick 465 Cranbury Rd, Ste 103 East Brunswick, NJ 08816
Learn more about our full range of physical therapy treatments and the conditions we treat, including our comprehensive ACL treatment program.
What Our Patients Say