Meniscus Tear Treatment in Clark, NJ — Trinity Rehab
Clark sits at the crossroads of suburban life and urban commuter culture — a place where Union County residents balance demanding work schedules with the pursuit of fitness and family recreation. For many of you, staying active isn’t optional; it’s how you manage stress, maintain energy, and create healthy habits for your families. You might cycle commute along local routes, run at Oak Ridge Park before heading to the city, or participate in recreational leagues that give structure to your evenings.
Then comes that single moment that changes everything: a twist during an early morning run, a plant-and-cut during a weekend soccer game, or an awkward step that creates that unmistakable pop in your knee. Suddenly, the activities that ground your life are off-limits. The commute bike sits unused. The running shoes collect dust. The thought of letting fitness slip becomes as frustrating as the knee pain itself. If you’re facing a meniscus tear, the encouraging news is that most cases resolve completely with targeted physical therapy — no surgery required — and you’ll return to your normal routine stronger and more resilient than before.
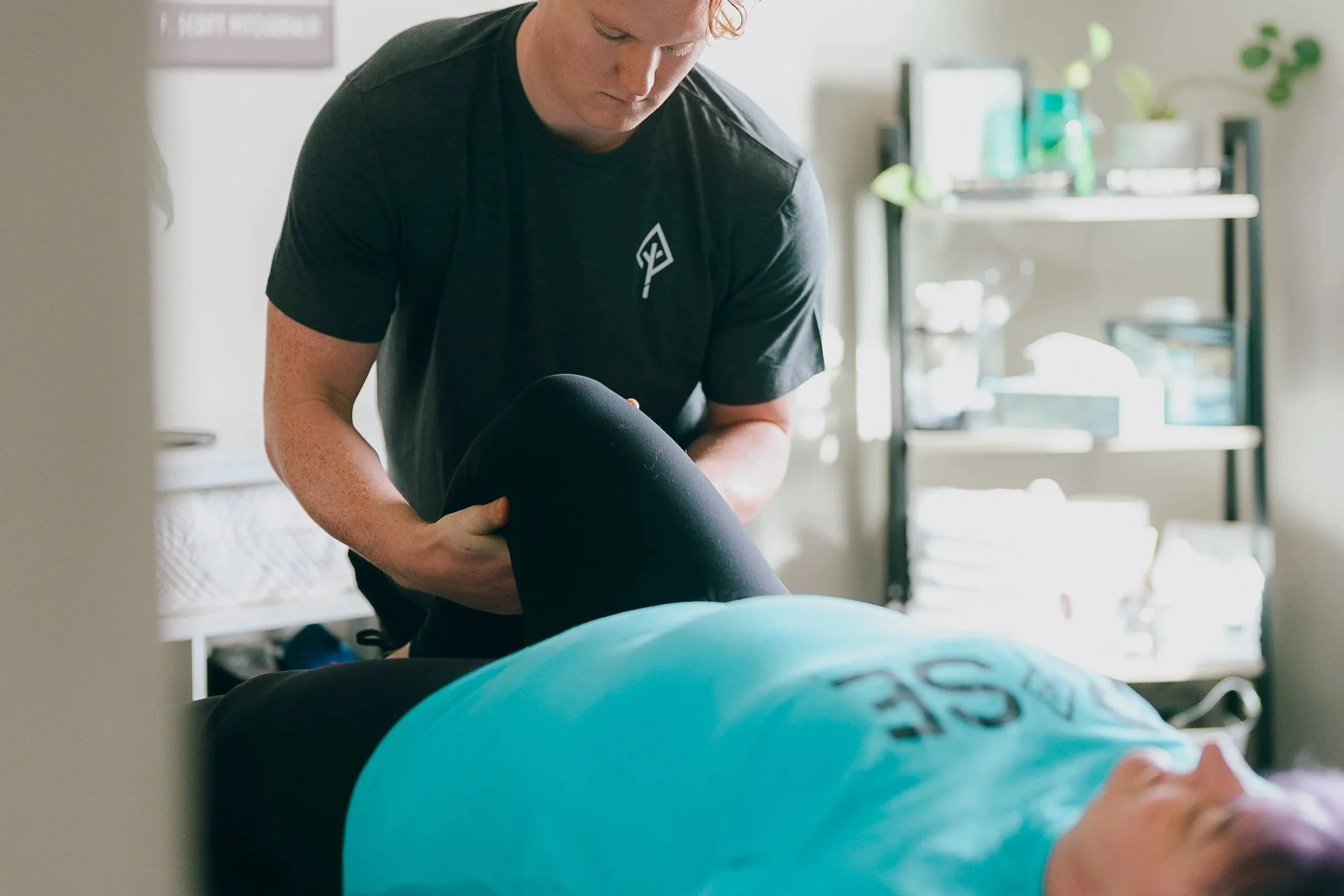
Understanding Your Meniscus and Why It Matters
Your meniscus is one of your knee’s most important structures — a crescent-shaped piece of cartilage that sits between your thighbone and shinbone, functioning as both a shock absorber and a force distributor. You have two menisci per knee: the medial (inner) meniscus and the lateral (outer) meniscus. Together, they handle the constant stress of movement, absorb impacts, reduce friction, and maintain joint stability.
When a meniscus tears, you immediately lose part of that protective system. The knee becomes less stable, shock absorption decreases, and pain develops as inflammation spreads through the joint. Left untreated, this can lead to progressive cartilage wear and the eventual development of osteoarthritis. In recent years, advancements in meniscus repair techniques for athletes have shown promising results in restoring knee function and enhancing recovery. These innovative methods prioritize not only the immediate stabilization of the joint but also aim to reduce the risk of long-term complications, allowing athletes to return to their sport with greater confidence. Emphasizing rehabilitation post-surgery is also crucial, as it aids in building strength and flexibility in the knee. understanding meniscus tear symptoms is crucial for early diagnosis and effective treatment. Common indicators include swelling, joint stiffness, and difficulty bearing weight on the affected knee. Recognizing these signs can help prevent further damage and guide you toward appropriate medical care.
The evidence is clear: physical therapy is as effective as surgery for most meniscus tears, particularly in adults. A landmark New England Journal of Medicine study found that conservative care and surgical intervention produced nearly identical outcomes for degenerative tears and peripheral tears in patients over 40.
Why Clark Residents Experience Meniscus Tears
The Clark lifestyle — balancing professional ambition with health consciousness — creates specific injury patterns:
- Commuter fitness routines — Many Clark residents use cycling or running as commuting and fitness combined. The repetitive loading of cycling or the impact of running can cause both acute tears (sudden twisting) and overuse tears (progressive stress)
- Garden State Parkway strain — Living along a major corridor means desk jobs with long sitting periods. When you suddenly exercise hard after static work, you’re loading tissues that haven’t been adequately prepared, increasing injury risk
- Suburban family sports — Youth leagues, recreational adult soccer, and tennis create dynamic movement patterns that sometimes result in meniscus tears
- Fitness gap phenomenon — Clark’s active population sometimes oscillates between busy work periods (sedentary) and ambitious fitness goals (sudden high intensity). The mismatch creates injury risk
- Weekend warrior injuries — Professionals who sit most of the week and then attempt intense activity on weekends are particularly vulnerable to meniscus tears
- Oak Ridge Park recreation — The popular local park hosts walking, running, cycling, and recreational activities that can precipitate injuries in people not properly conditioned for the activity intensity
Recognizing a Meniscus Tear
The injury often announces itself clearly:
- A pop, crack, or tearing sensation during movement (especially twisting, pivoting, or jumping)
- Swelling that develops over hours or 24-48 hours
- Sharp pain localized to the inner or outer edge of your knee
- Stiffness that makes straightening your knee difficult
- A catching, clicking, or grinding sensation, especially with rotational movements
- Instability or a sensation that your knee might give way
- Pain that worsens with stairs, squatting, or kneeling
- Progressive difficulty with the activity that caused the injury
For Clark’s commuters and fitness enthusiasts, the frustration is real: you suddenly can’t do the activities that manage your stress. The relief comes when you discover that recovery is usually rapid and complete.

Trinity Rehab Clark’s Three-Phase Rehabilitation Approach
Your meniscus tear treatment follows evidence-based protocols adapted to your specific goals — whether that’s returning to your commute cycling, resuming running, or simply moving without pain.
Phase 1: Acute Management (Weeks 1-3)
Your immediate priorities are controlling swelling and protecting the healing tissue:
- RICE protocol implementation — Rest (modified, not complete immobilization), Ice (regular intervals to reduce swelling), Compression (knee sleeve or wrap for stability), Elevation (above heart level)
- Non-narcotic pain management — Medications like ibuprofen or naproxen support comfort without sedation
- Manual therapy — Gentle joint mobilization and soft tissue techniques restore normal knee motion and reduce stiffness
- Modality support — Electrical stimulation and therapeutic ultrasound decrease inflammation and promote healing
- Gait retraining — Correcting walking compensations that develop immediately after injury to prevent secondary problems in your good leg
- Motion preservation — Careful, guided movements maintain your knee’s range without stressing the meniscus
Phase 2: Strength and Proprioception (Weeks 4-8)
This is where real recovery happens. Your therapist progressively rebuilds the muscular stabilization system:
- Quadriceps strengthening progression — From simple isometric contractions (quad sets) to dynamic exercises against increasing resistance. Strong quads are your primary shock absorbers
- Hamstring and hip strengthening — Balanced strength in all thigh muscles ensures forces distribute evenly and your knee doesn’t compensate
- Core stabilization — Your abdominal and back muscles contribute significantly to lower extremity stability
- Proprioceptive training — Balance exercises on unstable surfaces (balance pads, foam rollers) retrain automatic stabilization reflexes. This is critical for preventing re-injury
- Dry needling — Trigger point therapy releases compensatory muscle tension that accumulates during injury and altered movement
- Functional movement patterns — Progressing from simple exercises to complex movements (lunges, step-ups) performed with perfect form
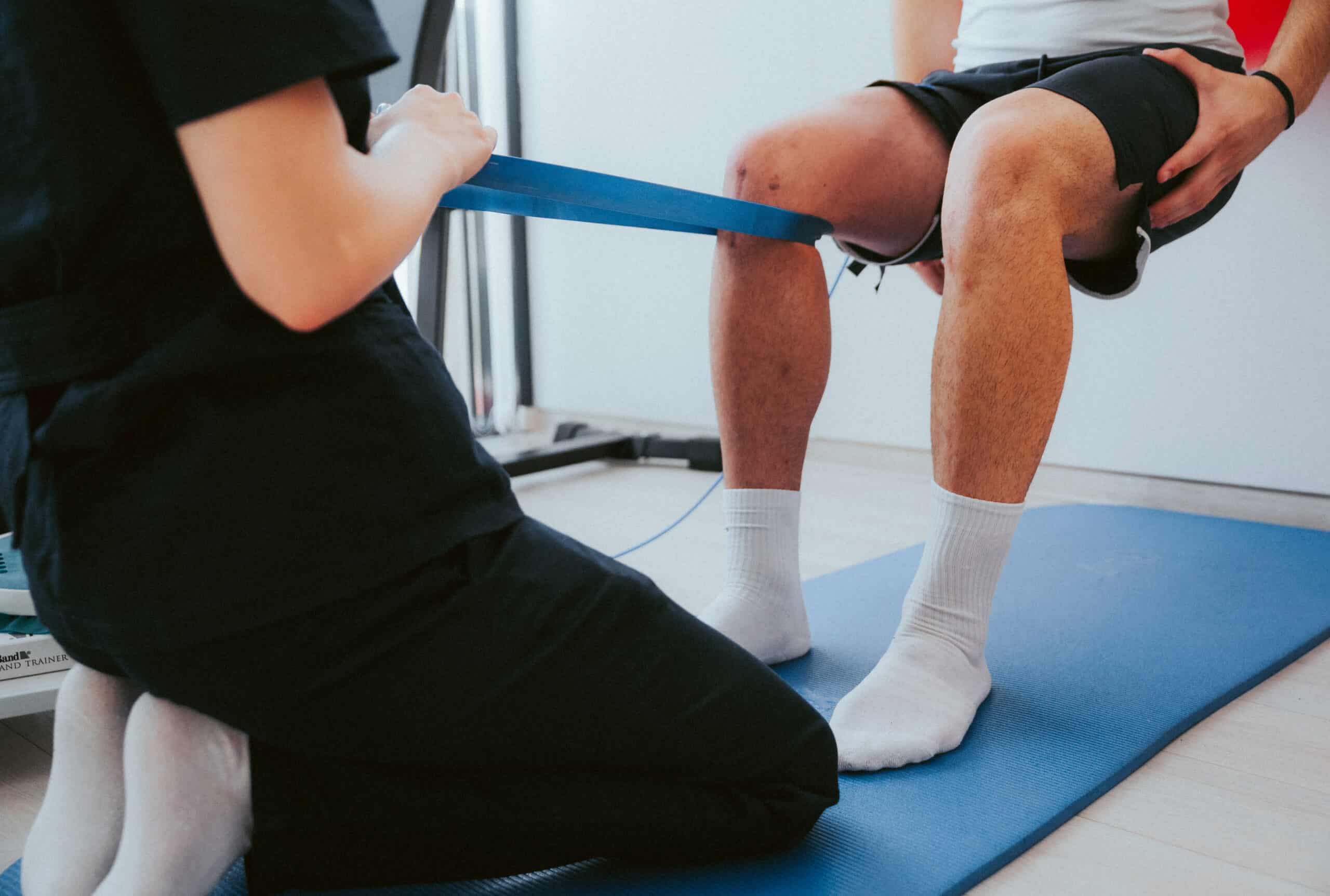
Phase 3: Return to Activity (Weeks 9-12+)
By this phase, you’re ready to systematically reintroduce the activities that define your life:
- Activity-specific training — If cycling is your commute, we progress from stationary cycling to actual riding. If running is your stress management, we systematically increase running distance and intensity. Every progression is data-driven
- Progressive loading — Gradually increasing demands so your knee adapts without re-injury risk
- Movement quality maintenance — Ensuring you’re not reverting to compensatory patterns even as intensity increases
- Return-to-sport/activity clearance — Objective testing of strength symmetry, proprioception, and activity-specific movements before full return
- EPAT/Shockwave therapy — When indicated, this advanced regenerative treatment uses acoustic pressure waves to stimulate tissue healing and optimize tissue quality
Tear Classification and Treatment Implications
The specific pattern of your meniscus tear influences how we treat and how quickly you recover:
- Radial tears — Most common, cutting across the meniscus fibers. Usually caused by sudden twisting. Small tears in the vascular outer zone respond excellently to physical therapy
- Horizontal tears — Running along the meniscus length. Often associated with degenerative changes. These typically respond very well to conservative care
- Bucket-handle tears — A large vertical tear where part of the meniscus displaces into the joint center. More likely to cause mechanical symptoms, sometimes requiring arthroscopy. Physical therapy remains central to recovery
- Flap tears — A section of meniscus folding over. Usually manageable with physical therapy
- Complex tears — Multiple tear patterns. Typically require longer rehabilitation but generally respond to nonsurgical treatment
Preventing Re-Injury: Your Long-Term Knee Strategy
Recovery doesn’t end when pain resolves. Maintaining meniscus health long-term prevents re-injury:
- Consistent strength maintenance — Year-round quadriceps and hamstring strength protects your meniscus from future injury, especially important if you cycle commute or run regularly
- Proper warm-up protocols — Dynamic stretching and light activity before intense exercise prepares tissues and primes neuromuscular stability
- Movement quality awareness — Poor landing mechanics, inward knee collapse, and asymmetrical movement patterns increase injury risk. Conscious attention to technique prevents problems
- Gradual intensity increases — Whether you’re increasing running mileage or cycling intensity, progression should be 10% per week maximum
- Recovery integration — Training without adequate recovery creates fatigue-induced movement degradation and injury risk. Rest days are injury prevention
- Footwear optimization — The right shoes for your activity type reduce abnormal knee loading
- Pain as a signal — Persistent discomfort after activity is your body requesting activity modification, not something to push through
Why Clark Commuters and Fitness Enthusiasts Choose Trinity Rehab Clark
Our clinic is designed for your lifestyle:
- Licensed physical therapists only — Every session is one-on-one with a licensed clinician. No aides, no group sessions. You receive full professional attention
- No referral requirement — Begin treatment immediately in New Jersey without physician approval — critical when you’re eager to return to your routine
- Early morning and evening appointments — Scheduling around your work commute is straightforward
- Evidence-based protocols — Our treatment reflects current research showing physical therapy’s effectiveness for meniscus tears
- Insurance coordination — We verify your coverage before your first visit
- Individualized progression — Your return-to-activity timeline is based on your specific injury and goals, not a generic protocol
- Accessible location — Convenient to Clark residents and commuters using the Garden State Parkway
Return to the Activities You Love
At Trinity Rehab Clark, we understand what your activity means to you — whether it’s your commute cycling, your stress-relief running, or your weekend recreational sports. Your meniscus tear recovery is designed around getting you back to those activities stronger and more resilient.
Frequently Asked Questions for Clark Residents
How long before I can cycle commute again?
Can I run during recovery?
What if I have to go back to my desk job immediately?
Do I need an MRI before starting therapy?
What's the risk of chronic knee problems after a meniscus tear?
Can I work around the injury while healing?
If I need surgery, do I still need physical therapy?
Schedule Your Evaluation
Start your recovery today:
- Book your appointment at Trinity Rehab Clark
- Comprehensive assessment — Your first visit includes detailed knee and movement evaluation
- Personalized plan — Your therapist develops your specific recovery timeline
No referral required. Schedule now.
Sources
- Katz, J. N., et al. (2013). Surgery versus physical therapy for a meniscal tear and osteoarthritis. New England Journal of Medicine, 368(18), 1675-1684.
- Sihvonen, R., et al. (2018). Arthroscopic partial meniscectomy for a degenerative meniscus tear: A 5-year follow-up of the FIDELITY randomized trial. British Journal of Sports Medicine, 52(21).
- American Academy of Orthopaedic Surgeons. (2024). Meniscus tears. OrthoInfo.





