Somerset sits in the heart of central New Jersey’s Raritan Valley, where the wide-open grounds of Colonial Park and Duke Farms invite walkers, cyclists, and gardeners year-round, and where Robert Wood Johnson University Hospital anchors a significant healthcare community. It is a diverse, working-class and professional suburb where families and retirees share neighborhood streets, community parks, and the region’s pharmaceutical and biotech employment corridor. And it is a place where osteoarthritis is a daily reality for a meaningful slice of residents — whether they are standing eight-hour shifts in a Branchburg warehouse, logging miles on the fitness parcourse at Colonial Park, or simply waking up with knees that hurt before breakfast.
Osteoarthritis is the most common degenerative joint disease in the United States, affecting more than 32.5 million adults and representing the leading cause of chronic pain and disability in adults over 45. The cartilage that cushions your joints — in the knees, hips, hands, and spine most commonly — gradually breaks down over years of use, injury, and mechanical stress. What remains is bone grinding against bone: painful, progressive, and capable of dismantling the quality of life you have worked hard to build.
The good news is that physical therapy is one of the most effective tools available for managing osteoarthritis. Recommended as a first-line treatment by the American College of Rheumatology and the Arthritis Foundation — ahead of escalating medication and well before surgery — physical therapy builds strength, restores flexibility, and equips you to manage your joint health for the long term. At Trinity Rehab, we serve Somerset-area patients with one-on-one, individualized osteoarthritis treatment that goes beyond generic exercises.
How Physical Therapy Treats Osteoarthritis
Phase 1: Assessment and Pain Relief
Every osteoarthritis treatment journey at Trinity Rehab begins with a thorough initial evaluation. Your physical therapist will assess your affected joint’s range of motion, the strength of surrounding muscle groups, your gait pattern, balance, and how your condition affects your daily function and recreational activities. This is not a generic intake — it is a detailed clinical picture that drives every subsequent decision.
For Somerset patients presenting with knee osteoarthritis or hip osteoarthritis, Phase 1 focuses on reducing pain and swelling that have been limiting your movement. The goal is to reduce pain quickly enough that exercise becomes possible, restore joint flexibility to the affected joint, and ease the morning stiffness that many patients describe as the first thing they notice each day. This phase typically spans the first two to three weeks and includes:
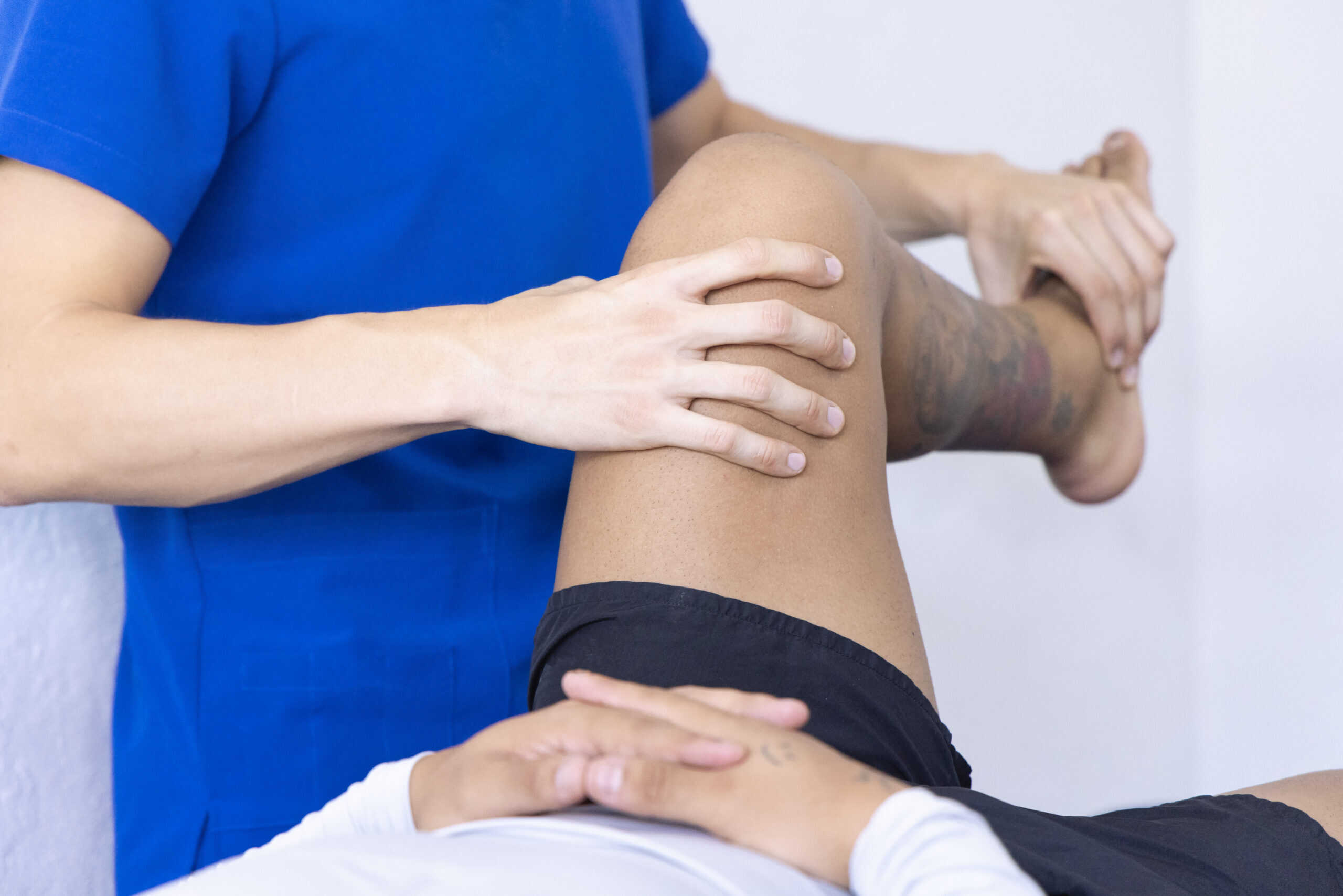
Manual therapy for immediate relief: Manual therapy techniques — joint mobilization, soft tissue mobilization, and passive range of motion work — are initiated early because they deliver rapid results. Joint mobilization applies gentle, graded oscillatory movements directly to the arthritic joint to reduce stiffness and improve the mechanical quality of joint motion. Soft tissue mobilization releases the tight muscles and dense fascia that form around a chronically painful joint. Somerset patients who have been guarding a painful hip or knee for months often find that several sessions of manual therapy restore range of motion to the affected joint — more than they expected — before they have even progressed to formal strengthening.
Transcutaneous electrical nerve stimulation (TENS): TENS is a non-invasive pain management modality that delivers low-voltage electrical current through surface electrodes to interrupt pain signals at the nerve level. It is effective for acute flares and can be used alongside manual therapy and early exercise to make movement more comfortable.
Patient education: Understanding your osteoarthritis diagnosis reduces fear and sets realistic expectations. Your physical therapist explains what is happening at the joint level, what the evidence says about physical therapy outcomes, and why movement — even when uncomfortable — is ultimately protective for arthritic joints.
Phase 2: Strength and Stability
The muscles surrounding an arthritic joint are its primary defense against further cartilage wear. Strong quadriceps, for instance, reduce bone-on-bone pressure at the knee during every step you take. Strong hip abductors reduce the compensatory lateral shift that sends excess load through both the hip joint and the lower back. When pain causes someone to move less — as is almost universally the case with osteoarthritis — these muscles weaken rapidly, accelerating the very joint deterioration they should be preventing.
Phase 2 of your osteoarthritis treatment at Trinity Rehab targets this weakness directly through a progressive, individualized exercise program:
Quadriceps and hamstring strengthening: For patients with knee arthritis, quad strengthening is the single most evidence-supported exercise intervention available. Research is clear: stronger quadriceps equal less knee pain, better function on stairs, and significantly delayed need for knee replacement surgery. Your program builds quadriceps strength progressively — starting from positions that minimize joint compression and advancing as your pain allows. Hamstring strengthening and PNF flexibility work complement quad training by improving the muscle balance around the knee joint.
Hip stabilization exercises: Hip abductor and gluteal strengthening reduces medial knee thrust during gait — a common mechanical fault that accelerates cartilage breakdown on the inner side of the knee. For patients with hip osteoarthritis, these exercises directly reduce the compressive forces through the hip joint during walking and stair use.
Core stabilization: A stable pelvis reduces shear forces on both the hip and lumbar spine. Core exercises appropriate for arthritis patients — which avoid excessive spinal flexion or high joint-loading positions — are integrated throughout the treatment plan.
Aerobic exercise conditioning: Low-impact aerobic exercise is one of the most important ongoing interventions for long-term osteoarthritis management. Your therapist prescribes walking, cycling, aquatic exercise, or anti-gravity treadmill training in volumes appropriate for your current level. Aerobic conditioning supports healthy weight maintenance, improves joint fluid circulation, and boosts mood — all of which matter for arthritis patients.
A Somerset resident who has worked at Robert Wood Johnson University Hospital Somerset for over a decade describes the turning point: “I was compensating so much for my hip that my lower back started to go too. When we addressed the hip weakness specifically, both areas improved together.”
Phase 3: Function, Technology, and Long-Term Management
Phase 3 focuses on translating your strength and flexibility gains into real-world function — and on using Trinity Rehab’s advanced treatment technology to go further than standard physical therapy alone.
AlterG Anti-Gravity Treadmill: Somerset patients who want to resume walking for exercise but find full weight-bearing aggravates their knee or hip pain have a particularly powerful option in the AlterG. This technology uses air pressure to precisely reduce effective body weight by up to 80%, allowing pain-free gait and aerobic exercise at whatever load your joints can handle. Clinical studies show 20–30% pain reduction and improved endurance for osteoarthritis patients using anti-gravity treadmill training. For golfers who walk the courses at Spooky Brook, Quail Brook, or Green Knoll Golf Courses, regaining the endurance to walk 18 holes without flaring is a goal the AlterG makes achievable.
EPAT Shockwave Therapy: Extracorporeal Pulse Activation Technology delivers high-energy acoustic pressure waves into damaged tissues surrounding arthritic joints. EPAT stimulates collagen production and natural tissue regeneration, addressing the tendon and soft tissue degeneration that frequently accompanies chronic knee arthritis and hip osteoarthritis. Research demonstrates 60–80% pain relief for associated soft tissue conditions. Patients who have reached a plateau in standard physical therapy often see renewed progress after incorporating EPAT.
Dry Needling: Chronically painful joints produce chronically tight muscles. Dry needling targets the myofascial trigger points that accumulate in muscles like the quadriceps, iliotibial band, piriformis, and calf — muscles that protect a painful joint but become painful themselves over time. By releasing these trigger points, dry needling improves flexibility, reduces the referred pain patterns that confuse diagnosis, and allows the strengthening exercises in Phase 2 to be more effective.
Activity modification coaching: Your therapist works through your specific daily activities — the pharmaceutical warehouse shift, the Saturday walk at Colonial Park’s 685-acre grounds, the garden work at Duke Farms volunteer days — and identifies joint protection strategies, pacing techniques, and body mechanic adjustments that reduce cumulative cartilage stress without forcing you to give up what you love.
Preventing Osteoarthritis from Getting Worse
Physical therapy at Trinity Rehab gives you more than symptom relief — it gives you a self-management framework for life. Strategies your therapist will teach include:
- Maintaining an appropriate body weight to reduce mechanical load on weight-bearing joints (every 10% weight reduction can cut knee pain by up to 50%)
- A consistent home exercise program — three to four sessions per week maintains the strength gains achieved in therapy
- Proper footwear and joint protection techniques during work and recreational activities
- How to recognize an inflammatory flare early and respond appropriately to prevent setbacks
- When to return for periodic reassessment as your condition evolves
- Information on dietary supplements (glucosamine, chondroitin) — your therapist can guide an evidence-based conversation about what the research does and does not support
It is worth noting that there are currently no proven disease-modifying agents for osteoarthritis treatment. The most effective interventions remain exercise, manual therapy, weight management, and structured physical therapy — all of which are central to your care at Trinity Rehab.
Why Somerset Patients Choose Trinity Rehab
One-on-one care with a licensed physical therapist at every session is not the standard at all clinics. At Trinity Rehab, it is non-negotiable. Your therapist observes every exercise repetition, adjusts cueing and resistance in real time, and ensures you are building strength safely without stressing cartilage you cannot afford to lose.
Our clinical expertise spans the full arthritis spectrum — from early knee arthritis managed conservatively all the way to post-surgical recovery following joint replacement. Geriatric physical therapy for older Somerset residents managing multiple joint conditions simultaneously, and sports medicine-informed programming for active adults who want to stay on the golf course or the trails — both are part of what we do.
We accept most major insurance plans and handle insurance verification for you. Most patients have physical therapy coverage with modest out-of-pocket costs.

Inside Our Somerset Clinic




Related Conditions & Treatments
Osteoarthritis is just one of the many conditions we treat at Trinity Rehab Somerset. Explore our full range of conditions we treat or learn more about specific treatment approaches:
Frequently Asked Questions
Do I need a doctor's referral to start physical therapy for osteoarthritis in Somerset, NJ?
What is osteoarthritis, and how is it different from other types of arthritis?
Can physical therapy help me avoid joint replacement surgery?
How does the AlterG Anti-Gravity Treadmill help with osteoarthritis?
What should I expect at my first physical therapy appointment in Somerset?
Getting Back to Your Somerset Life
Whether you are a long-time Somerset resident who walks Duke Farms trails on weekends, a healthcare professional on your feet at RWJ Somerset, or a retiree who wants to keep tending your garden without waking up the next morning unable to straighten your knees — you deserve more than pills and rest. You deserve a plan.
Physical therapy at Trinity Rehab gives you that plan. Evidence-based osteoarthritis care, one-on-one with a physical therapist who knows your goals and monitors your progress at every session. Back pain, knee pain, and hip and knee conditions — we treat them all within a coordinated, personalized program.
Your Next Steps
- Request an appointment online or call the Trinity Rehab location nearest Somerset.
- Complete a brief intake form — minimal paperwork so you can focus on getting better.
- Meet your physical therapist for a full evaluation and begin your personalized treatment plan.
Same-week appointments are frequently available. New Jersey Direct Access means no referral, no delay — just call and we will handle the rest.
Sources: Centers for Disease Control and Prevention. Osteoarthritis. https://www.cdc.gov/arthritis/osteoarthritis/ | Journal of Orthopaedic & Sports Physical Therapy. https://www.jospt.org/ | Frontiers in Physiology. Physical therapy as a promising treatment for osteoarthritis. https://pmc.ncbi.nlm.nih.gov/articles/PMC9614272/