PLANTAR FASCIITIS TREATMENT IN WAYNE, NJ
Wayne is a town that keeps people moving. The Wayne Walks club logs weekly miles through High Mountain Park Preserve and Packanack Lake. The Wayne PAL keeps hundreds of young athletes on fields and courts through every season. Wayne Hills Patriots and Wayne Valley Indians athletes push hard through their competitive schedules. And at St. Joseph’s Wayne Medical Center, at the Valley National Bank campus, at Costco, UPS, and the Amazon facility, thousands of Wayne residents spend their workdays predominantly on their feet.
Plantar fasciitis is the heel pain condition that can bring all of that to a painful halt — or at minimum, reshape every day around the dread of that first step out of bed. The sharp, searing pain that radiates up from the heel, the stiffness that takes 15 minutes to shake loose every morning, the aching that returns after sitting through a long meeting or a commute — it’s a cycle that grinds people down.
Trinity Rehab’s physical therapists help Wayne residents identify exactly what is driving their plantar fasciitis and treat it at the source. With one-on-one care grounded in current clinical evidence, the majority of patients recover fully and return to all the activities they value — without surgery, injections, or indefinite limitation.

WHAT IS PLANTAR FASCIITIS?
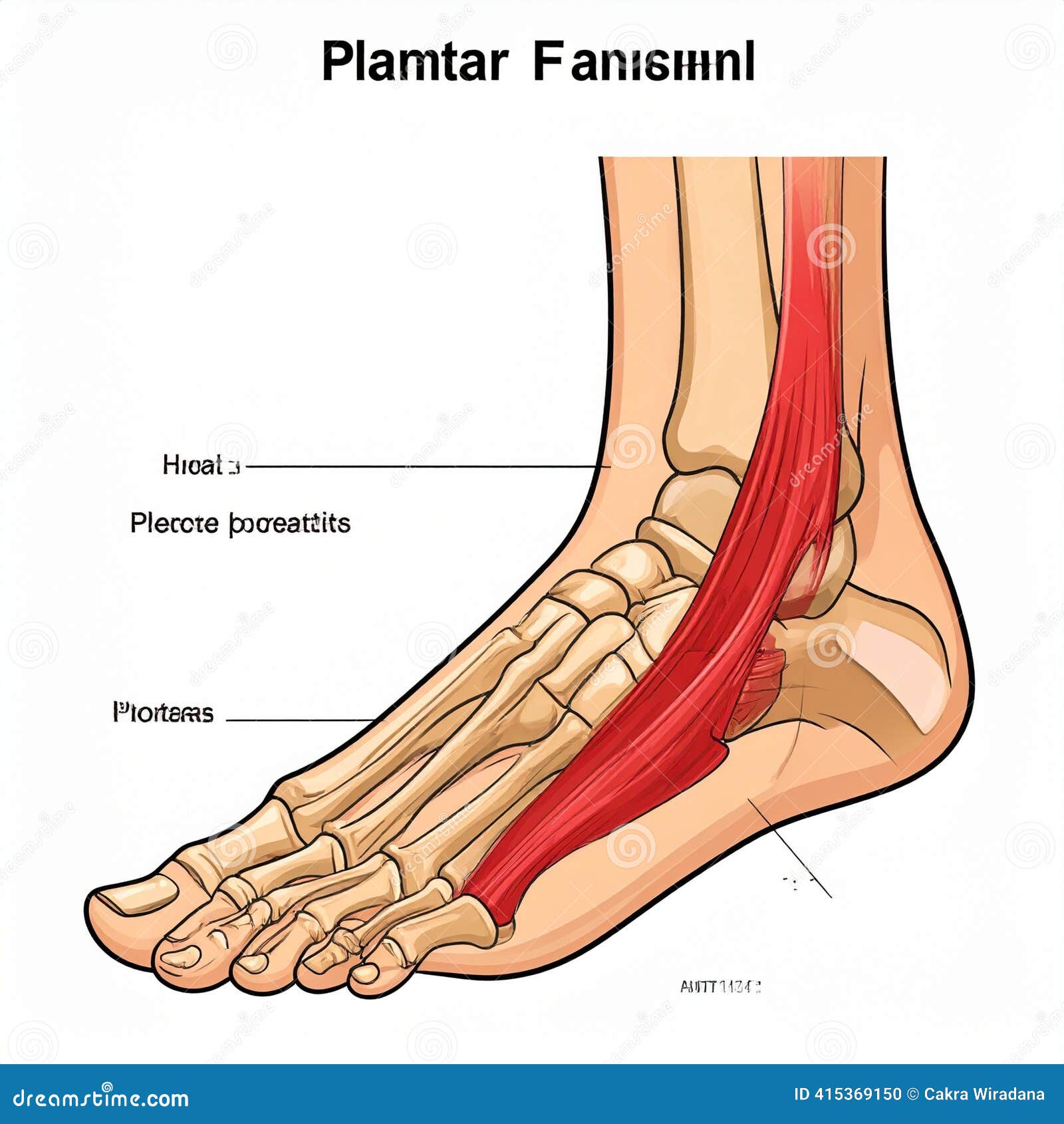
The plantar fascia is the thick, fibrous connective tissue band that runs along the sole of your foot from the heel bone to the ball of the foot. It functions as a dynamic arch support and shock absorber, enabling the efficient biomechanics your foot uses with every step through a mechanism called the windlass effect.
When the tissue is loaded beyond its capacity to repair itself — through repetitive impact, prolonged standing, or biomechanical inefficiencies — micro-tears accumulate at the calcaneal attachment, triggering inflammation. Over time, without adequate recovery and treatment, this progresses to fascial thickening and degeneration, extending the pain cycle far beyond what most patients expect when symptoms first appear.
The American Academy of Orthopaedic Surgeons estimates that plantar fasciitis accounts for 11 to 15 percent of all foot complaints requiring professional care, with roughly 2 million Americans treated annually. Physical therapy, when applied with the right techniques at the right time, resolves most cases without invasive intervention.
RELATED CONDITIONS & TREATMENTS
Plantar fasciitis is just one of the many conditions we treat at Trinity Rehab Wayne. Explore our full range of conditions we treat or learn more about specific treatment approaches:
WAYNE’S SPECIFIC RISK FACTORS
Wayne’s particular combination of active recreation, busy employment landscape, and high school athletics creates several distinct paths to plantar fasciitis.
High Mountain Park Preserve hikers and runners enjoy 1,153 acres of trails that climb from Wayne’s valley terrain to exposed ridgeline views. The varied surface — including rooted single-track, rocky ridge sections, and soft meadow paths — demands constant foot adaptation, loading the plantar fascia in highly variable ways. The Wayne Walks club, which hosts organized walks in High Mountain Preserve, Laurelwood Arboretum, and around Packanack Lake, brings people onto these surfaces consistently throughout the year. An uptick in spring walking volume is frequently the trigger event for plantar fasciitis.
Wayne PAL youth sport families — parents, coaches, and young athletes themselves — spend significant time on their feet at games, practices, and tournaments. Coaches who stand for hours on hard gym floors or grass fields, and adolescent athletes in football, basketball, and soccer who train year-round, both accumulate the kinds of lower limb stress that predispose toward plantar fasciitis.
Wayne Hills and Wayne Valley student-athletes competing across football, soccer, field hockey, track, and cross-country carry the overuse injury risks inherent to high school athletic competition. Cross-country runners training for the Passaic County circuit log significant weekly mileage on varied terrain — a classic context for plantar fasciitis development when recovery isn’t prioritized alongside training.
Healthcare workers at St. Joseph’s Wayne Medical Center — a 229-bed hospital employing hundreds of clinical and support staff — spend extended shifts on hard institutional floors. The combination of long hours, clinical grade footwear requirements, and limited sitting time creates the sustained fascial loading that precedes plantar fasciitis.
Retail and warehouse workers at Costco, UPS, and Amazon distribution sites throughout Wayne face a similar occupational hazard on an even harder surface. Concrete warehouse floors offer virtually no give, and the combination of carrying loads, prolonged standing, and repetitive walking significantly stresses the plantar fascia. Work-related foot conditions like plantar fasciitis are disproportionately common in these environments.
Golfers at Preakness Valley Golf Course and Packanack Golf Club log miles of walking across 18 holes of gently sloped terrain, often in footwear designed more for traction than cushioning. The sustained, repetitive loading on the same tissue over a four-hour round is a recognized plantar fasciitis trigger.
RECOGNIZING PLANTAR FASCIITIS SYMPTOMS
The symptom pattern is distinctive — though recognizing it is not the same as treating it:
The defining symptom is sharp, stabbing heel pain with the first steps of the morning. The plantar fascia stiffens overnight as it contracts without load; the sudden weight of your first steps creates an abrupt, intense stretch at the calcaneal attachment. Many patients describe it as stepping on broken glass or a hot coal. This “first-step pain” typically eases over the first 10 to 20 minutes as the tissue warms, then returns after the next period of rest.
Other signs to watch for:
- Pain after sitting in traffic, at a desk, or in a meeting room — the same stiffening-and-sudden-stretch cycle as mornings
- Tenderness when pressing on the inner edge of the heel, directly at the origin of the plantar fascia
- A dull, aching tightness along the arch that develops through the day
- Pain that peaks 30 to 60 minutes after completing a run or long hike, rather than during it
- Noticeable changes in how you walk — a shortened stride, limping, or weight-shifting to avoid heel contact
A Wayne resident who leads Wayne Walks hikes described the progression: “I started noticing it at the end of longer hikes — my heel would ache on the drive home. Then it started hurting in the morning. Eventually I was stretching my heel before I’d even gotten out of bed, just trying to take the edge off.” That trajectory — from post-activity aching to persistent morning pain — is classic plantar fasciitis, and it responds well to physical therapy when addressed before it becomes fully chronic.
PHYSICAL THERAPY TREATMENT: A TOPIC-BASED APPROACH
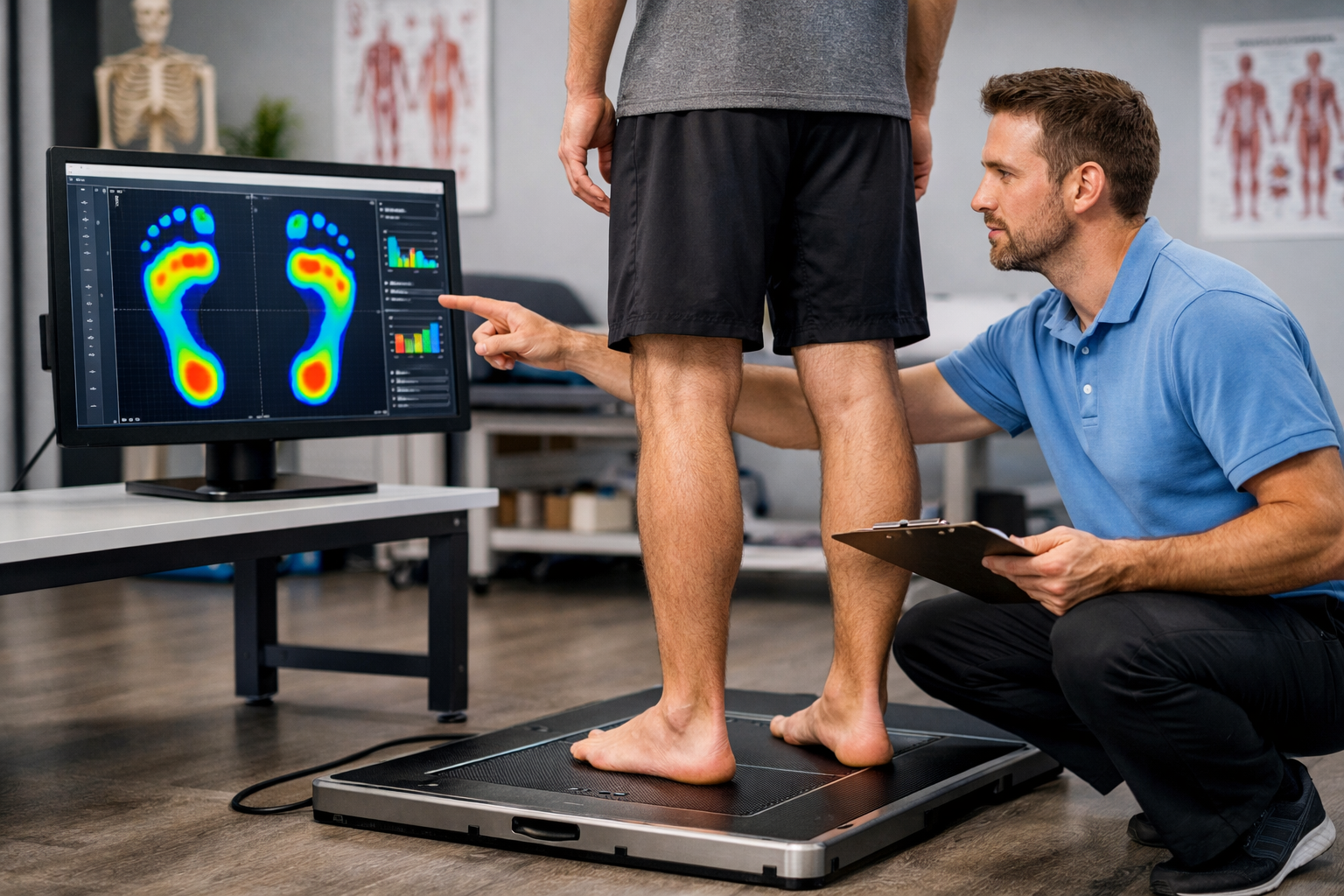
At Trinity Rehab Wayne, your treatment plan is built around your specific drivers, not a generic protocol. An evaluation of your foot mechanics, ankle mobility, gait pattern, and activity history guides every component.
MANUAL THERAPY
Manual therapy is often the intervention that produces the fastest initial relief. Restricted ankle dorsiflexion — caused by tight calf muscles from running, hiking, or prolonged sitting — is among the most consistent mechanical drivers of plantar fasciitis. When the ankle cannot complete its full range of motion, each step transfers disproportionate strain to the plantar fascia as compensation.
Your therapist uses ankle and subtalar joint mobilization to restore this lost motion. Clinical research in the Journal of Orthopaedic & Sports Physical Therapy confirms that joint mobilization combined with stretching produces significantly better outcomes than stretching alone — making hands-on work a clinically essential component, not a luxury.
Instrument-assisted soft tissue mobilization (IASTM) addresses the adhesions and scar tissue that accumulate in chronically loaded fascia. Specialized tools create a controlled stimulus that triggers fresh collagen production and healthy tissue remodeling. Myofascial release targeting trigger points in the gastrocnemius, soleus, and foot intrinsic muscles reduces resting fascial tension and creates the tissue slack necessary for healing.

TARGETED STRETCHING
Your home stretching program is prescribed based on your specific deficits. The plantar fascia-specific stretch — dorsiflexing the toes before the first step of the morning — has strong clinical support for reducing first-step pain. Gastrocnemius and soleus stretching addresses the calf tightness that drives so much plantar fasciitis pathology. Your therapist will assess whether your restriction is primarily in the gastrocnemius or soleus (or both) and prescribe stretches that target each appropriately.
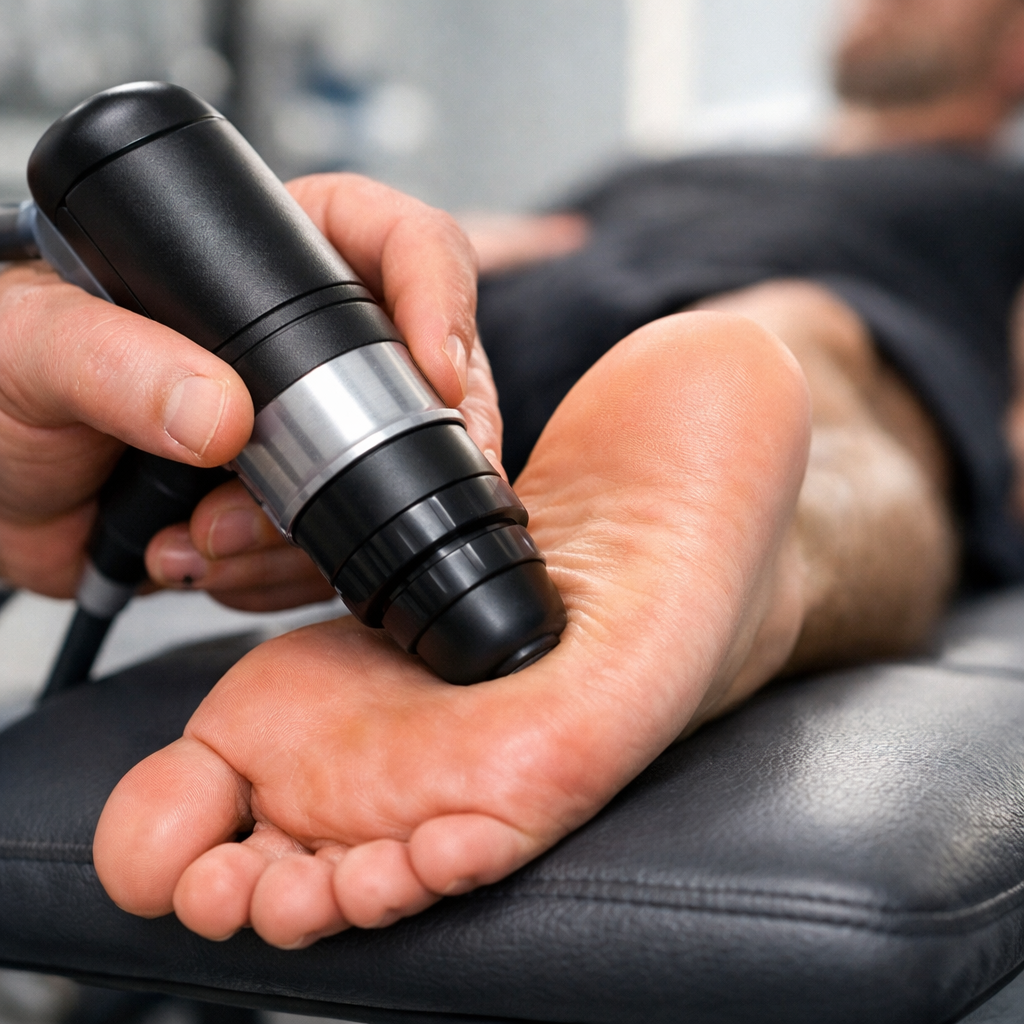
EPAT SHOCKWAVE THERAPY
For Wayne patients with chronic plantar fasciitis — symptoms lasting six months or more without adequate improvement from conservative care — EPAT shockwave therapy is available at Trinity Rehab. High-energy acoustic pressure waves stimulate blood flow and activate the body’s cellular repair mechanisms in the damaged fascial tissue. The Mayo Clinic identifies EPAT as an effective option for chronic, treatment-resistant cases. It is a non-invasive procedure performed in-clinic, with most patients completing a short course of sessions.
DRY NEEDLING
Dry needling is a precise technique in which thin filament needles are inserted into trigger points within the calf, Achilles, and foot musculature. By mechanically stimulating these tight bands, dry needling releases the muscular tension that perpetuates fascial overload. For patients with significant myofascial involvement — particularly common in runners and hikers whose calf muscles carry chronic tension — dry needling accelerates tissue recovery in a way that stretching alone cannot replicate.
ECCENTRIC LOADING AND STRENGTHENING
Strengthening the foot and calf complex is what converts a pain-managed foot back into a resilient, load-tolerant one. Eccentric calf raises on a step edge are the gold standard for building the tensile strength in the calf-Achilles-fascia chain. Intrinsic foot exercises (towel scrunches, short-foot maneuvers, marble pickups) develop the arch’s internal muscular support. Progressive single-leg balance training restores the neuromuscular control that degrades when pain alters your gait pattern.
PREVENTION TIPS FOR WAYNE RESIDENTS
- Track mileage on your Wayne Walks hikes. Replace hiking footwear and trail runners based on miles logged, not how the outsole looks. Midsole cushioning deteriorates long before outsole tread wears through.
- Invest in proper footwear for hospital or warehouse work. A full shift at St. Joseph’s Wayne or a day at a warehouse requires footwear with genuine arch support and cushioning. Fashion athletic shoes and flat retail sneakers are not adequate substitutes.
- Add calf stretching to your post-hike routine. Five minutes of gastrocnemius and soleus stretching after every High Mountain Preserve hike prevents the progressive tightness that feeds plantar fasciitis.
- Warm up before PAL-coached sessions. Whether you’re a parent coaching the sideline or a Wayne Hills athlete before practice, a plantar fascia stretch and heel cord mobilization before activity reduces first-load tissue stress.
- Progress running volume by no more than 10% per week. This is the most effective single training practice for preventing overuse-related plantar fasciitis in Wayne’s running community.
WHY WAYNE PATIENTS CHOOSE TRINITY REHAB
Trinity Rehab’s Wayne-area clinic delivers the one-on-one care model that produces better outcomes in plantar fasciitis treatment. Every session is with your licensed physical therapist — not an aide or assistant working from your initial evaluation notes. Your therapist is present to observe how you move, adjust techniques based on your response, and ensure you’re progressing at a rate that builds resilience without aggravating tissue that’s still healing.
We work with most major insurance plans, require no physician referral, and offer scheduling options that accommodate Wayne’s working families and commuters. Our treatment protocols reflect the current evidence-based guidelines from the American Physical Therapy Association. Beyond the foot, we address the compensatory downstream effects that plantar fasciitis commonly creates — including lower back pain and sciatica — as part of a whole-body recovery approach. See our full list of foot and ankle conditions and what we treat.
Inside Our Wayne Clinic



Wayne Foot And Heel Pain Care For Walking Comfort
Plantar fasciitis can make the first steps of the morning, work shifts, shopping, walking exercise, and standing-heavy days difficult for Wayne patients. Local rehab should connect foot symptoms to calf mobility, footwear, activity load, and the way you move.
Your evaluation may include foot and ankle mobility, calf strength, balance, walking mechanics, hip control, tenderness patterns, and screening for symptoms that may need medical care first, such as major trauma, suspected fracture, severe swelling, or inability to bear weight.
Related Wayne pages include ankle pain treatment, sports injury physical therapy, and the main Wayne clinic page.
FREQUENTLY ASKED QUESTIONS
Where can I receive plantar fasciitis treatment in Wayne, NJ?
How long does plantar fasciitis take to heal with physical therapy?
Can I still hike at High Mountain Park during treatment?
Do I need surgery if conservative treatment hasn’t worked?
Will I need orthotics?
YOUR RETURN TO WAYNE’S ACTIVE LIFE
High Mountain’s trails are worth hiking. The Wayne PAL seasons are worth coaching. The morning walks with the Wayne Walks club are worth resuming. Plantar fasciitis stands between you and all of that — but it doesn’t have to stay there.
Request your appointment at Trinity Rehab today and take the first step toward recovering your heel and reclaiming your full, active Wayne lifestyle.
Sources: JOSPT Clinical Practice Guidelines for Heel Pain/Plantar Fasciitis, 2023 | Mayo Clinic — Plantar Fasciitis | American Academy of Orthopaedic Surgeons | APTA Clinical Practice Guidelines




