PLANTAR FASCIITIS TREATMENT IN SPARTA, NJ
If you live in Sparta, you chose this place for a reason — the lake communities, the hiking trails through the Sussex County Highlands, the golf at SkyView or Lake Mohawk Golf Club, the quiet roads perfect for a morning run. But when plantar fasciitis sets in, all of that can feel suddenly out of reach. The Iron Mine Trail is waiting, your buddies have a tee time at SkyView, and your first step out of bed sends a bolt of pain through your heel that makes you wonder whether any of it is worth it.
Here’s what matters: plantar fasciitis is among the most successfully treated musculoskeletal conditions physical therapy addresses. The vast majority of people who commit to the right treatment protocol recover fully — without surgery, without cortisone injections, without giving up the lifestyle that makes Sparta worth living in.
Trinity Rehab’s physical therapists work with Sparta residents who hike the Sparta Glen, run with the local club, work standing-intensive jobs in Sussex County, and push through ski season at Mountain Creek while their feet quietly accumulate stress. We know what’s at stake, and we build treatment plans around getting you back to exactly those things.

WHAT IS PLANTAR FASCIITIS?
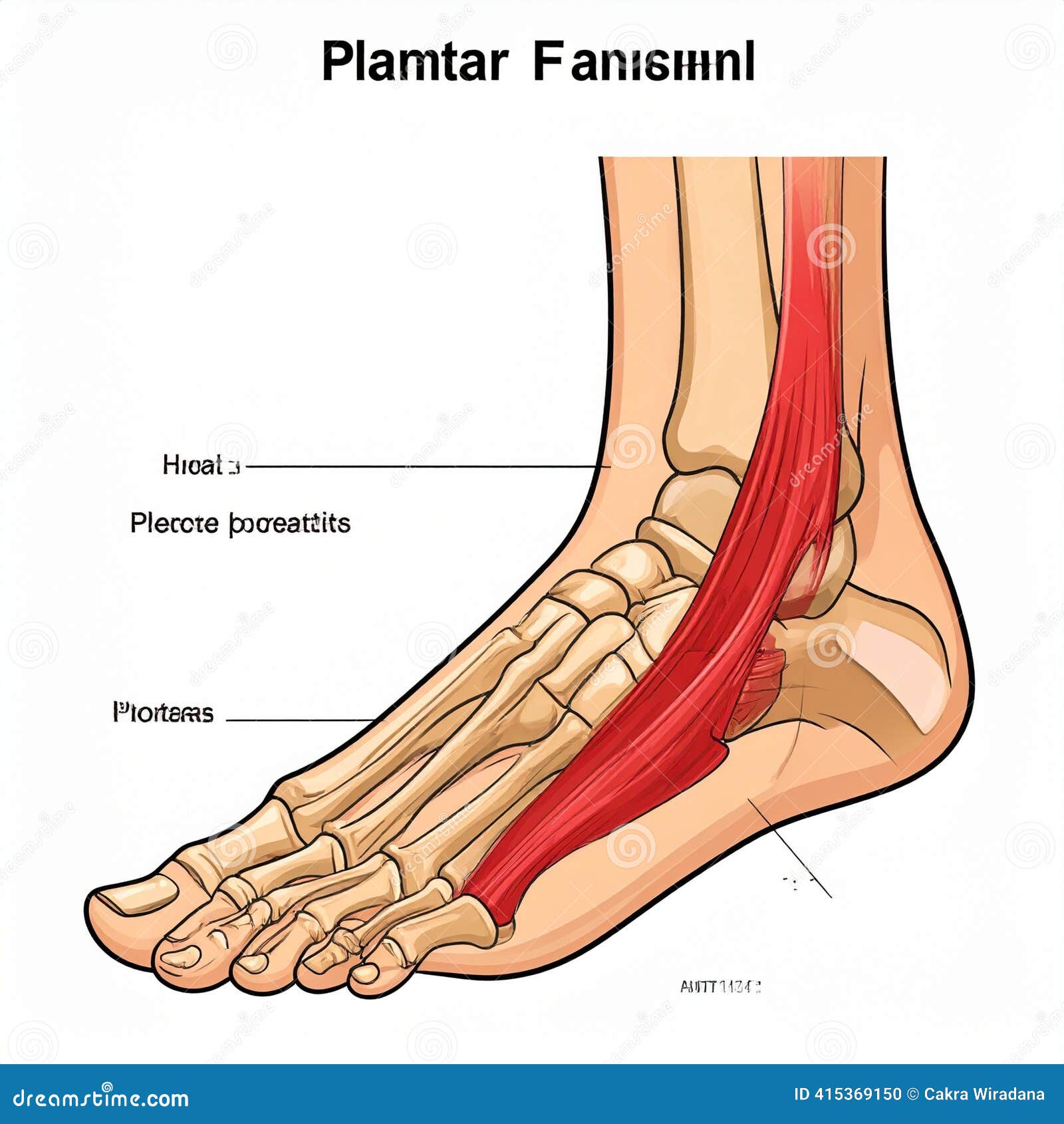
Your plantar fascia is a tough, fibrous band of connective tissue running the full length of your foot’s sole, from the base of the heel bone to the ball of the foot. It functions as a dynamic bowstring — supporting your arch, absorbing the shock of each footfall, and enabling the propulsive mechanics your foot needs to move you forward efficiently.
Plantar fasciitis occurs when the cumulative stress placed on this tissue outpaces its ability to repair itself. Micro-tears accumulate in the fascia, particularly at the point where it attaches to the calcaneus (heel bone), triggering an inflammatory response that the body struggles to fully resolve under continued loading. Over time, the tissue can thicken and degenerate — a process clinicians sometimes call plantar fasciopathy — making even basic walking increasingly uncomfortable.
Left unaddressed, this becomes a self-perpetuating cycle. The American Academy of Orthopaedic Surgeons reports that roughly 2 million Americans seek treatment for plantar fasciitis annually. Physical therapy, when applied correctly and early, resolves most cases within three to six months.
RELATED CONDITIONS & TREATMENTS
Plantar fasciitis is just one of the many conditions we treat at Trinity Rehab Sparta. Explore our full range of conditions we treat or learn more about specific treatment approaches:
WHY SPARTA RESIDENTS ARE SUSCEPTIBLE
Sparta’s geography and culture — while genuinely wonderful — create conditions that are particularly hard on the plantar fascia.
Trail hiking and running on routes like the Iron Mine Trail, Sparta Glen, and the Kittatinny Ridge sections nearby involve uneven terrain, root-covered surfaces, and elevation changes that recruit the foot in highly variable ways. Every landing on an uneven surface creates unpredictable fascial loading. Over the course of a long hike or trail run, those micro-variations compound into significant cumulative stress.
Golf at Lake Mohawk Golf Club and SkyView Golf Club demands miles of walking over 18 holes — often on slightly sloped fairways — combined with the rotational forces of the swing. Golfers in Sparta routinely walk 5 to 7 miles on a Saturday morning, frequently in footwear that prioritizes traction over cushioning. The repetitive loading pattern over uneven terrain is a recognized plantar fasciitis trigger.
Skiing and snowboarding at Mountain Creek puts the ankle and foot in a fixed, plantar-flexed position for hours at a time. When ski boots come off, the foot transitions abruptly to unrestricted movement, and the shortened, stiffened calf muscles that develop through a ski season dramatically increase strain on the plantar fascia.
Sparta High School Spartan athletes — particularly those in football, wrestling, cross-country, and track — experience significant lower limb loading during their seasons. Athletes who compete year-round in multiple sports are especially prone to overuse injuries that include plantar fasciitis.
Lake community residents often do considerable walking on docks, boat launches, and uneven lakeside terrain in flat, unsupportive footwear. Flip-flops and boat shoes are among the worst options for plantar fascia health, yet they’re the default choice around Lake Mohawk and the other private lake communities.
RECOGNIZING THE SIGNS
The symptom picture of plantar fasciitis is distinctive enough that many patients recognize it before they receive a formal diagnosis:
- Searing first-step pain in the morning — the classic sign. The fascia stiffens overnight, and the abrupt stretch of initial weight-bearing creates an intense, stabbing pain under the heel that’s often described as stepping on a sharp stone.
- Pain that eases after 10 to 15 minutes of walking — as the tissue warms, the acute stiffness diminishes, though it often returns later in the day.
- Soreness after sitting — the same stiffening that occurs overnight also happens in a car, at a desk, or on a chairlift. The first steps after any period of rest are notoriously uncomfortable.
- Tenderness at the heel’s inner edge — pressing on the inside of the heel, where the fascia attaches, typically reproduces the characteristic pain.
- Post-activity achiness — hikers and runners often notice that heel pain is worse an hour or two after completing a trail, rather than during it.
A Sparta resident who regularly hikes the Kittatinny Ridge described noticing the pattern after a particularly long day on the trail: “The hike felt fine, but by dinner my heel was so sore I couldn’t stand to cook. The next morning stepping out of bed was awful.” That delayed post-activity pain combined with morning stiffness is a classic plantar fasciitis presentation, and it responds well to targeted physical therapy.
Don’t wait until the pain is severe enough to keep you completely off the trail. Earlier treatment means faster recovery and lower risk of the condition becoming chronic.
MANUAL THERAPY FOR PLANTAR FASCIITIS
Manual therapy is often the most immediate and impactful intervention in a plantar fasciitis treatment plan. At Trinity Rehab, our hands-on techniques go well beyond generic massage:
Joint mobilization of the ankle and subtalar joints restores the dorsiflexion range of motion that tight structures progressively steal. Clinical research published in the Journal of Orthopaedic & Sports Physical Therapy demonstrates that subtalar mobilization combined with stretching produces significantly better outcomes than stretching alone — a finding that directly shapes how our therapists structure your early sessions.
Instrument-assisted soft tissue mobilization (IASTM) uses specialized tools to address adhesions and scar tissue in the plantar fascia itself, as well as through the calf and Achilles complex. By creating a controlled microtrauma in the targeted tissue, IASTM stimulates fresh collagen production and healthy tissue remodeling.
Myofascial release targets the trigger points in the gastrocnemius, soleus, and foot intrinsic muscles that maintain fascial tension even at rest. Releasing these points reduces the resting load on the plantar fascia and gives the tissue room to heal.

TARGETED STRETCHING AND FLEXIBILITY WORK
The stretching program your therapist designs for you isn’t a generic handout — it’s calibrated to your specific deficits. The most important components:
Plantar fascia-specific stretch: Before your feet touch the floor in the morning, grasp your foot, pull the toes back into dorsiflexion, and hold for 30 seconds. This loads the windlass mechanism and pre-stretches the fascia before it takes your body weight. Performing this consistently reduces the severity of morning pain significantly.
Gastrocnemius and soleus stretching: Restricted ankle dorsiflexion — often caused by tight calf muscles developed through hiking, skiing, or running — is one of the most consistent biomechanical drivers of plantar fasciitis. Wall stretches, step drops, and towel-assisted stretches are prescribed based on which portion of the calf is most restricted.
Achilles tendon loading: The mechanical connection between the Achilles tendon and the plantar fascia means that Achilles mobility directly affects fascial stress. Dynamic stretches and controlled eccentric loading address this kinetic chain link.
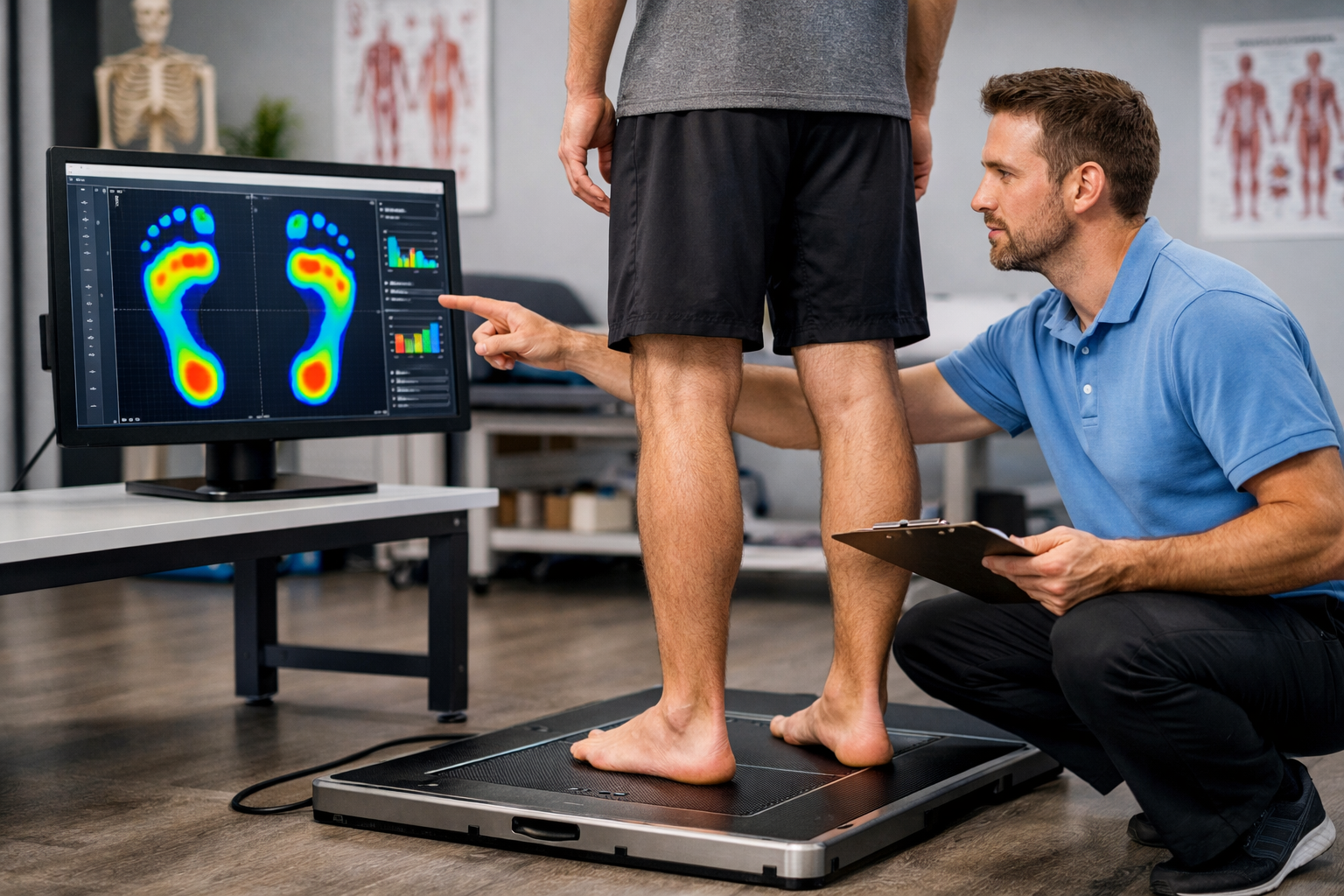
PROGRESSIVE STRENGTHENING AND EPAT
Once pain is managed, strengthening the foot and lower leg is what makes recovery stick:
Eccentric calf raises on a step edge build the tendon and fascial resilience that allows the plantar fascia to handle load without breaking down. Intrinsic foot exercises — towel scrunches, marble pickups, and the “short foot” maneuver — strengthen the small muscles that provide the arch’s internal support. Single-leg balance progressions on unstable surfaces improve proprioception and correct the compensatory loading patterns that often develop around a painful heel.
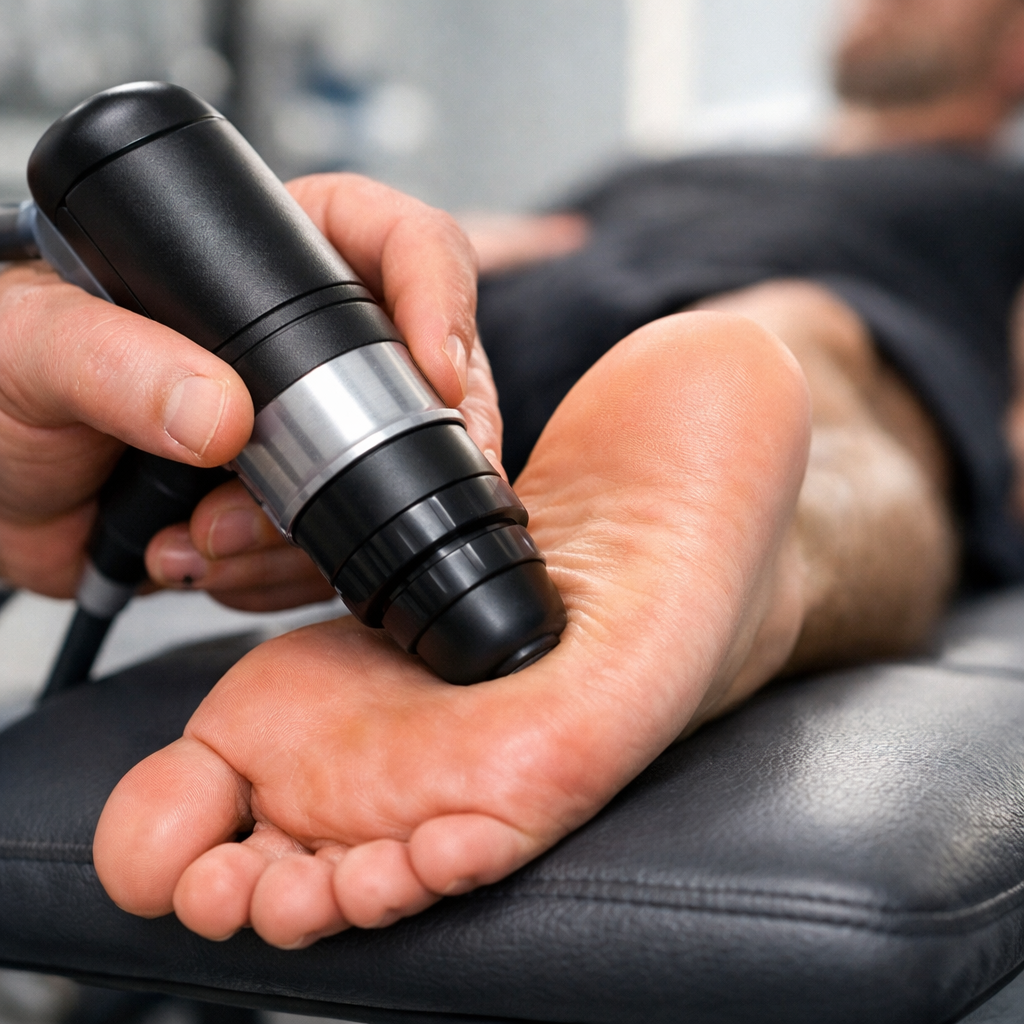
For Sparta patients with chronic or treatment-resistant plantar fasciitis, EPAT shockwave therapy is available at Trinity Rehab. High-energy acoustic waves penetrate the damaged fascia, stimulating blood flow and triggering the body’s natural tissue repair mechanisms. The Mayo Clinic identifies shockwave therapy as an effective option for patients whose symptoms have persisted despite conservative care. Dry needling is another option for cases complicated by significant trigger points in the calf musculature — a common finding in patients who ski or run regularly.
PREVENTION STRATEGIES FOR ACTIVE SPARTA RESIDENTS
Protecting your plantar fascia in Sparta’s active environment takes some deliberate planning:
- Trail footwear matters. Hiking boots and trail runners with substantial arch support and cushioned midsoles buffer the uneven terrain forces that accumulate on the Iron Mine Trail and Sparta Glen. Replace trail shoes when the midsole compresses visibly — usually well before the outsole tread wears through.
- Warm up before morning hikes. A few minutes of calf stretching and plantar fascia work before lacing up can prevent the abrupt stretch that initiates injury.
- Reconsider your lake footwear. Around Lake Mohawk and your dock, choose supportive sandals over flat flip-flops, especially for extended walking.
- Post-ski calf care. After a day at Mountain Creek, stretch your calves and Achilles thoroughly — the sustained shortened position in ski boots creates the tightness that feeds plantar fasciitis.
- Don’t ramp up trail miles too quickly. If you’ve been relatively inactive over winter and want to get back on the trails in spring, follow the 10% rule: increase weekly hiking or running volume by no more than 10% per week.
WHY SPARTA PATIENTS CHOOSE TRINITY REHAB
At Trinity Rehab, your sessions are spent one-on-one with your licensed physical therapist — not handed to a technician or left to do exercises unsupervised while your therapist works with another patient. That direct attention means your plan is constantly adjusted based on how you’re responding, and you have an expert present to answer questions and troubleshoot any setbacks.
We work with most major insurance plans and require no physician referral to begin treatment. Our team has deep experience treating the full range of foot and ankle conditions that affect active adults in the Sussex County area, and we understand the specific demands that Sparta’s outdoor lifestyle places on the feet and ankles. We also see how compensatory patterns from heel pain can create downstream problems — from back pain to sciatica — and we address the whole picture.
Inside Our Sparta Clinic


FREQUENTLY ASKED QUESTIONS
Where can I get plantar fasciitis treatment near Sparta, NJ?
Will I need to stop hiking and trail running during treatment?
How is plantar fasciitis different from a heel spur?
Can tight calves from skiing cause plantar fasciitis?
How long before I can get back to the trails pain-free?
RECLAIM YOUR SPARTA LIFESTYLE
The trails, the golf courses, the lake paths, the ski runs — all of it is still waiting for you. Plantar fasciitis is a real and significant condition, but it is also one that physical therapy addresses with a high success rate when treatment is started at the right time.
Trinity Rehab is here to get you back to the activities that drew you to Sparta in the first place. Request your appointment today and take the first step toward a pain-free heel — and a fully reclaimed outdoor life.
Sources: JOSPT Clinical Practice Guidelines for Heel Pain/Plantar Fasciitis, 2023 | Mayo Clinic — Plantar Fasciitis | American Academy of Orthopaedic Surgeons | NIH/PMC — Management of Plantar Fasciitis
What Our Patients Say




